Imaging plays major role in fight against head and neck cancers
Watch this session on ECR Live: Monday, March 11, 08:30–10:00, Room N/O
Tweet #ECR2013NO #SF16B
Organ-sparing surgery and radiation treatment such as intensity-modulated radiotherapy (IMRT) – often combined with chemotherapy – have increased the need for advanced imaging in the head and neck during pre-treament and post-treatment stages. Precision is vital as any tumour that remains undetected outside the treatment field could adversely affect the patients’ prognosis and survival, according to Professor Vincent Vandecaveye, from the department of radiology at the University Hospitals Leuven in Belgium.
It is important to spot any tumour recurrence as early as possible, especially in the post-treatment phase, in order give the patient the best possible chance of salvage treatment. The most common imaging methods in the head and neck area remain CT, MRI and PET-CT; each comes with its own advantages and disadvantages.
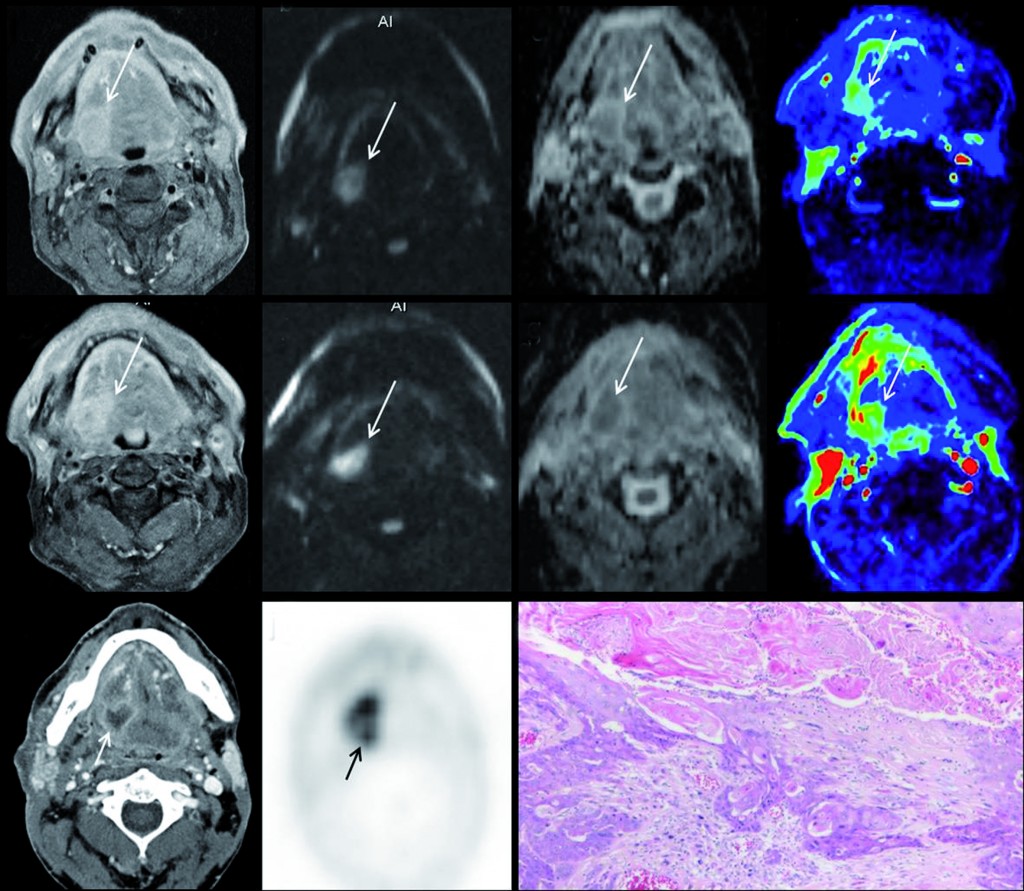
Multiparametric MRI for early treatment prediction of chemoradiation in oropharyngeal cancer: Upper row is pre-treatment MRI of right base of tongue cancer (a=contrast enhanced T1 as anatomical correlate; b=native b1000 diffusion-weighted image; c= ADC-map; d=perfusion-map of IUAC). Middle row is 2 weeks during chemoradiation: same imaging sets, tumour volume will not help. No significant change in b1000, ADC nor perfusion-MRI indicate non-response and thus high risk of tumour relapse after end of treatment. Tumour relapse at PET-CT 8 months after end of treatment, proven by histology (k). (Provided by Professor Vincent Vandecaveye)
When ECR Today asked Vandecaveye about his thoughts on the progress taking place in the field of MRI imaging and how this could influence head and neck imaging he gave us a very promising answer: “Personally, I think the increasing ability of MRI to provide functional imaging assessment, for example diffusion and perfusion-weighted MRI, of head and neck cancer for primary staging, recurrence imaging or treatment prediction holds great promise. MRI is not just a single modality; I believe functional MRI techniques can provide a better correlate to metabolic imaging than the classic anatomical imaging sequences. The latter are of major interest in the development of hybrid PET-MRI systems. Functional MRI is quite difficult to perform in the head and neck, from a technical point of view, but the vast progress made in MRI-technology, including hardware and software developments, and the gradual increase in knowledge and experience in several centres will improve it.“
In the struggle against cancer we tend to only look at the possibilities offered by technology and science, which have, without doubt, become extremely sophisticated and effective in modern medicine. However, modern clinical practice also depends very heavily on a multidisciplinary approach, which is only possible through the establishment of clear communication strategies and teamwork within a hospital or department.
“I think the single most important component is direct communication with your clinician. Although there are clear guidelines for diagnosis and treatment; techniques and habits may vary depending on the individual surgeon, oncologist or radiation oncologist.
Your report should of course primarily contain what we usually do in the majority of cases, such as describing the extent of lesions. In addition to that, it is useful to indicate abnormalities that are decisive for treatment and highlight them,” said Prof. Vandecaveye.
Tumour boards represent the perfect opportunity to directly communicate with clinicians and to discuss reports, if anything remains unclear.
“From my experience, you can gain a lot of gratitude and consideration from your clinical colleagues for this, and at the same time a radiologist can learn a lot regarding treatment and patient management,” said Prof. Vandecaveye, recommending that radiologists join these boards.
As imaging is becoming more and more complex, radiologists have an evolving role as liaisons in the clinical setting and should become actively involved in diagnostic management and treatment planning. As radiologists often have a more general background than clinical organ specialists, they also have an important role in the identification of patients who will eventually have diseases other than those affecting the head and neck, and so they can help refer the patient to the correct physician.
Another issue that is becoming more and more important in modern medicine is cost efficiency and its influence on the quality of diagnosis. It is important to combine knowledge of the different imaging modalities’ abilities with clinical guidelines, which are quite well organised for head and neck cancer. For instance, the risk of distant metastases increases significantly with nodal metastases at the low neck levels, and for these patients more stringent staging should be done in order to rule out distant metastases before initiating local therapy, which should be done with PET-CT. However, there is no need to carry out advanced imaging for distant staging in patients with low risk locoregional disease, and in these cases costs can be safely reduced by just using chest x-ray and ultrasound of the liver for distant staging.
“Sometimes these discussions about cost-effectiveness worry me as they create a false idea of a so-called one-stop-shop imaging modality that can solve all diagnostic problems. Of course this would be the holy grail, but I have rarely seen this happen in clinical reality. Radiologists should combine their knowledge of guidelines with their common sense, clinical abilities and reasoning. We should be aware; however, of what extent advanced imaging truly helps the patient and clinician. We probably have a better chance of reducing costs by trying to avoid overdiagnosis,” said Prof. Vandecaveye.
The session on the fight against head and neck cancers will also feature talks by Doctor Frank Pameijer on ‘Building blocks for locoregional staging of head and neck tumours’, Professor Minerva Becker on ‘Detection of tumour recurrence in head and neck cancer: challenges and pitfalls’ and finally, Professor Roberto Maroldi on ‘Locoregional treatment failure in head and neck cancer: causes and clinical implications’.
Finally, when asked why he would recommend this session to ECR attendees, Prof. Vandecaveye had this to say: “I think we have excellent speakers who have major experience in the field of head and neck cancer imaging, each covering different but complementary areas of expertise. At the same time the lectures provide a good mixture of daily practice, advanced imaging and future developments. This means that the topic is varied and interesting for radiologists, who deal with head and neck cancer while working in a more general setting, and radiologists who work in a more specialised setting. Finally, we provide a close correlation between imaging and clinics which also brings the topic close to clinical practice.”
Special Focus Session
Monday, March 11, 08:30–10:00, Room N/O
SF 16b: Head and neck cancer battle: the power of imaging studies
• Chairman’s introduction
V. Vandecaveye; Leuven/BE
• Building blocks for locoregional staging of head and neck tumours
F.A. Pameijer; Utrecht/NL
• Detection of tumour recurrence in head and neck cancer: challenges and pitfalls
M. Becker; Geneva/CH
• Locoregional treatment failure in head and neck cancer: causes and clinical implications
R. Maroldi; Brescia/IT
P. Nicolai; Brescia/IT
• Panel discussion: Advanced imaging in clinical practice: how does it help the patient?



Really informative post on Head and Neck Cancer and i hope it’ll help the patient and also very helpful for hospital too.
Thank you
I like the section in your articles that talks about how MRIs are improving and increasing their ability to provide functioning imaging assessment. This would probably be important to allow doctors to give a more accurate assessment and maybe catch problems earlier. If you need to get an MRI, you’d probably want to ensure you go to someone who stays updated with the machinery and techniques to ensure you get the best imaging that will help you.