
Dear Friends,
Today I am presenting radiographs of a 30-year-old man. They were taken because an abnormal ECG was found in a routine check-up. What do you see?
Check the images below, leave your thoughts in the comments section and come back on Friday for the answer.
Read more…

Dear Friends,
This week we are showing a relaxing case. Images belong to a 64-year-old man with a cough and fever. What do you see?
Check the images below, leave your thoughts in the comments section, and come back on Friday for the answer.
Read more…

Dear Friends,
Today we’ll start the second part of The Beauty of Basic Knowledge series, titled ‘To err is human: how to avoid slipping up’. In the next six chapters I intend to analyse the most common causes of errors in chest imaging and how to avoid them. As Cicero said: All men can err, but only the ignorant persevere in the error.
This week I am presenting two cases. Case 1 shows the PA radiograph of a 57-year-old man with a cough. Would you say the chest is normal?
1.Yes
2.No
3.Need a lateral view
4.Need a CT
Case 2 presents PA and lateral radiographs of the yearly check-up of a 70-year-old man. CT done in another institution was reported as chronic post-TB changes. Do you agree?
Check the images below, leave your thoughts in the comments section and come back on Friday for the full solution!
Read more…

Dear Friends,
Today we are showing chest radiographs of a 75-year-old man with a cough and haemoptysis.
What do you see? Check the images below, leave your thoughts in the comments section, and come back on Friday for the answer.
Read more…

Dear Friends,
Today I am presenting the last chapter of the Painless Approach to Interpretation. Showing chest radiographs taken during an annual check-up of a 70-year-old man.
What do you see? Check the images below, leave your thoughts in the comments section and come back on Friday for the answer.
Read more…

Dear Friends,
We are starting the new year with a warm-up case. Today we are presenting a PA chest radiograph of a 57-year-old woman with a cough and sputum production.
Check the image below, leave your thoughts in the comments section, and come back on Friday for the answer.
Diagnosis:
1. Changes post TB
2. Congenital right lung hypoplasia
3. Mesothelioma
4. None of the above
Read more…

Dear Friends,
Dr Pepe and I are very proud to have reached the 150th mark, which happens to be a case that we saw last month (honest!). The radiographs belong to a 68-year-old man, pre-op for cataracts.
What do you see? Check the images below, leave your thoughts for us in the comments section, and come back on Friday for the answer.
Read more…

Dear Friends,
Today I present the seventh chapter of the Painless Approach to Interpretation, which also happens to be case number 100 of Dr. Pepe’s Diploma Casebook. It makes me very proud to have shared with you one hundred cases and hope they have been useful.
Showing chest radiographs of a 47-year-old woman with mild fever and chest pain.
What do you see? Check the images below, leave me your thoughts in the comments section and come back on Friday for the answer.
Read more…

Dear Friends,
Today we are presenting a pre-op PA chest radiograph of a patient with inguinal hernia. What do you see?
Check the image below, leave your thoughts in the comments section and come back on Friday for the answer.
Read more…

Christina Harter-Felszeghy, co-creator of the amazing winner of our International Day of Radiology cake competition explains the inspiration and production of the winning cake. Don’t miss the photo gallery at the bottom of this post.
My Father, Dr. Scott Harter, is a radiologist and Chief of Radiology Consultants in Little Rock (Arkansas, USA) and I am a confectioner. While researching how Radiology Consultants could celebrate IDoR 2016, Radiology Consultants’ social media manager came across a post about the ESR’s Cake Competition on the International Day of Radiology website. My father and I volunteered to design and bake a cake to share with the group, thinking it would be a wonderful way to celebrate this special day! It turned out to be a truly unique project.
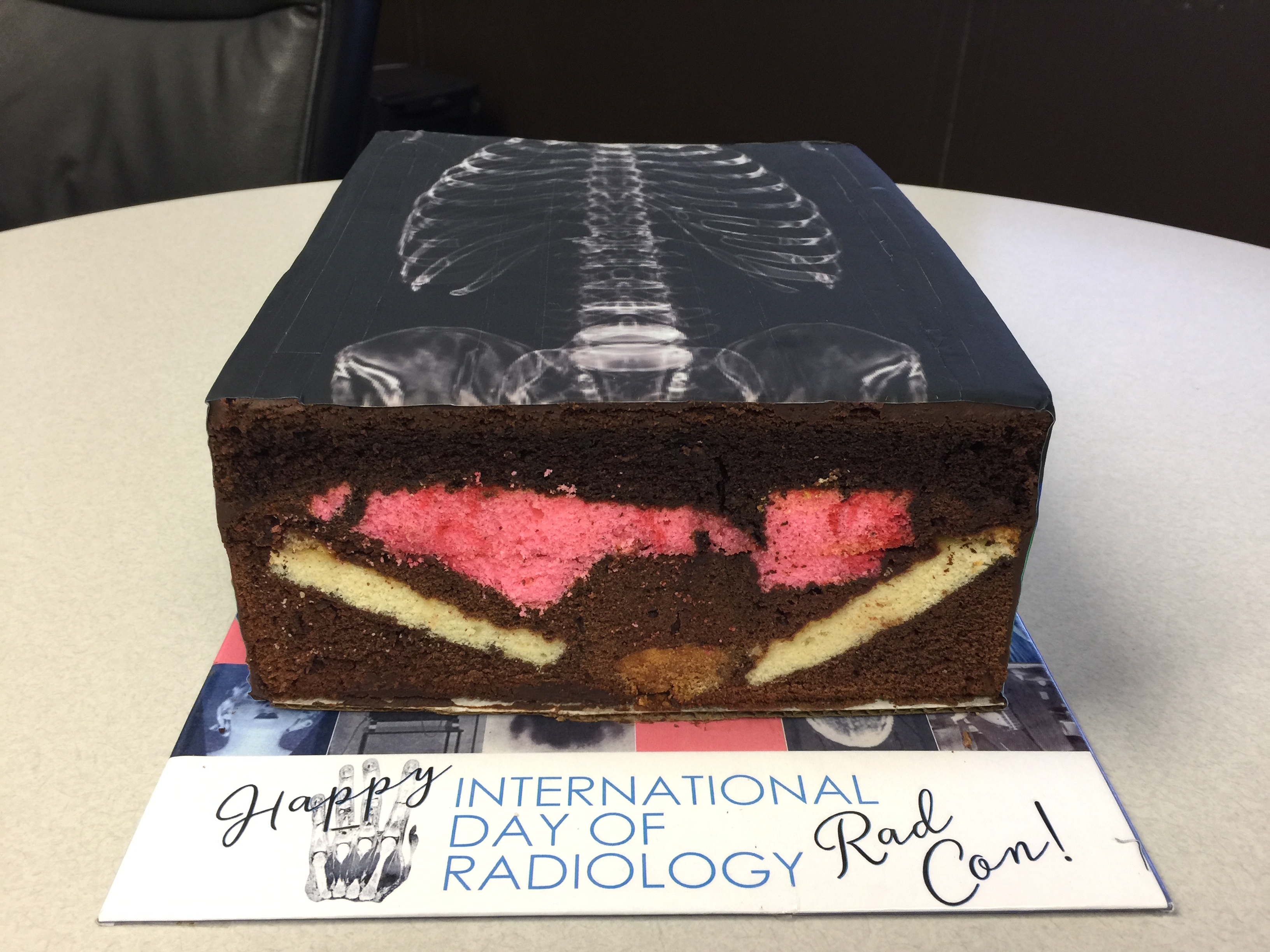
The winning cake (cross section)
Read more…










