
Dear Friends,
Muppet is very happy with your progress. But, given his mean disposition, he wants to test you with this case:
Forty-year-old woman with a moderate cough.
Diagnosis:
1. Tuberculosis
2. Vascular malformation
3. Aspergillosis
4. None of the above
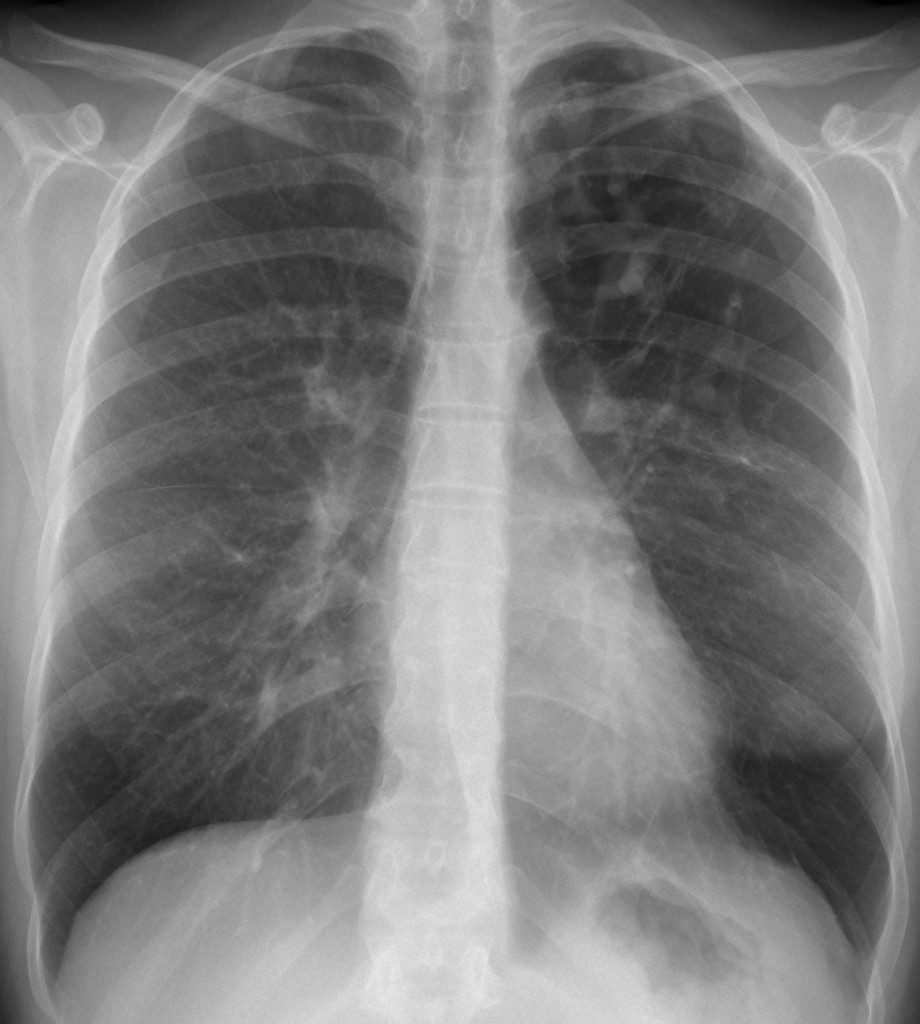
40-year-old woman, PA chest
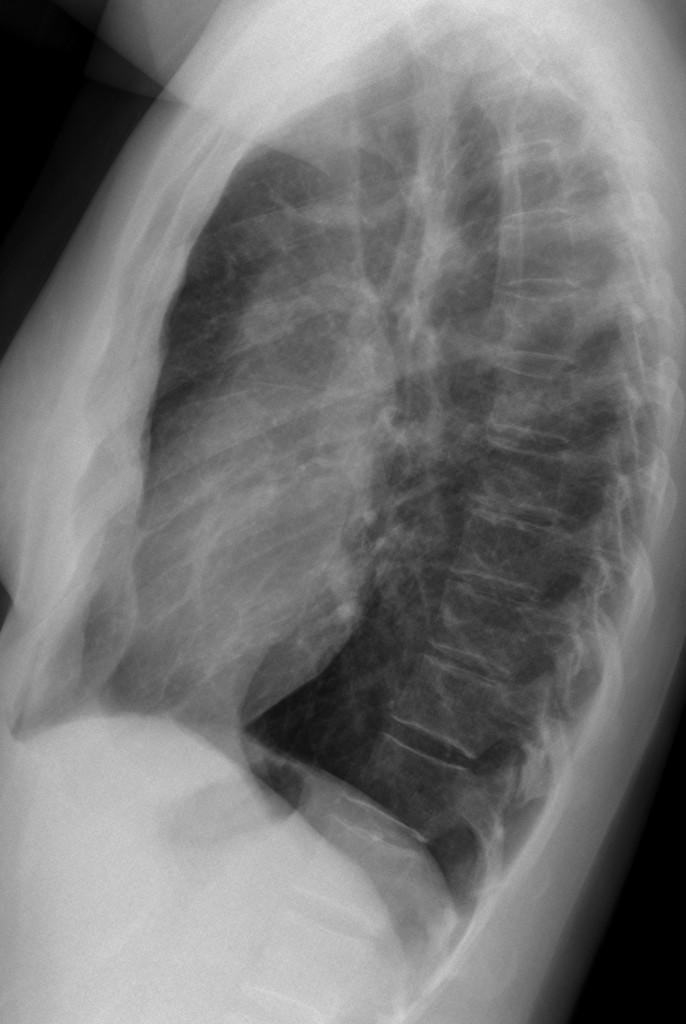
40-year-old woman, lateral chest
Click here for the answer to case #13
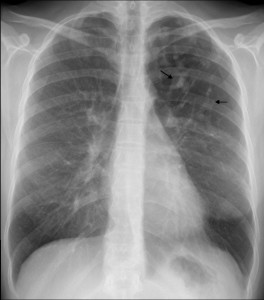
The PA chest film (fig. 1) shows an area of hyperlucency in the left upper lung, with branching, serpiginous shadows within (arrows). Whenever we see branching shadows, two possibilities should come to mind: vessels or dilated bronchi. Vascular malformations are not associated with hyperlucent lung, whereas the combination of branching shadows and hyperlucency should make segmental bronchial obstruction with mucous impaction the most likely possibility.
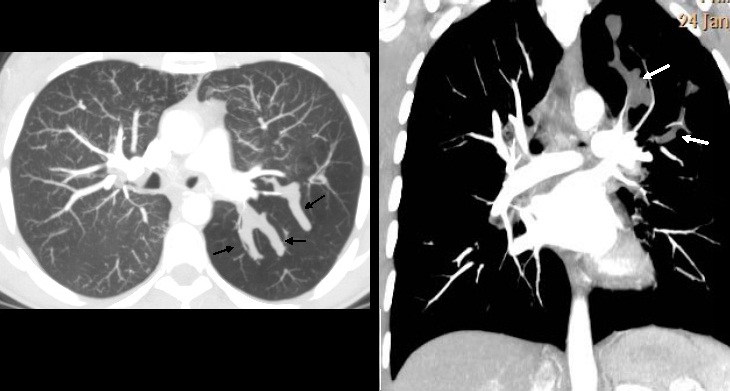
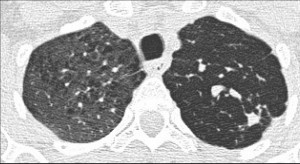
Axial and coronal enhanced CT confirms the unenhanced mucous plug (figs. 2,3 arrows) within the area of hyperlucency. Expiratory film confirms air trapping (fig. 4). Final diagnosis: congenital bronchial atresia, confirmed with bronchoscopy.
Teaching point: think of mucous impaction when you see branching shadows.
Remember that the most common cause of mucous impaction is lung carcinoma. When in doubt, perform bronchoscopy.








-Young woman with unspecific clinical presentation.
-The first thing I notice is a complex combination of nodular and tubular images on the left upper lobe (I would prefer it in lower lobes thinking in a pulmonary AVM, diagnosis which must guide us to rule out Rendu Osler Webber from my point of view).
– In a second view I think I can detect the underlying parenchyma is not normal, it seems like with fibrous thick tracts; the first diagnosis which come to my head now is ancient tuberculosis (previous granulomatous infection). I really like the upper location for TBC.
Trying to correlate the finding I described; my first option is a kind of vascular malformation secondary to previous inflammatory process (probably TBC). So a kind of COMPLEX RASMUSSEN ANEURYSM.
The second possibility is that I have invented the fibrotic parenchymal changes and that it was “only” a AVM (need in this case to rule out Rendu Osler Webber as I said before).
i’ll go with option 1 i.e tuberculosis
-Mild volume loss involving left upper lobe with cavitatory lesions,fibrotic,nodular and tubular opacities.
-Suggestion of narrowing of distal left main bronchus.
Aspergillosis on the background of chronic tuberculosis should be considered. few of the soft tissue opacities may represent rasmussen aneurysms.
Left hilum is not pulled up. Don’t you think this goes against chronic TB?
yes sir but there is definite volume loss. linear fibrotic strands also are seen.process is too focal for vasculitis(although bronchial wall narrowing has been described in WG) Otherwise it could be ABPA.
Aspergillosis with ?h/o TB from the nodular shadows.
Why do I miss the shadow of the richt breast?
Should we think about immunsupression as a result of chemotherapy due to breast cancer? Then an reactivatet, but not really typical tbc is also possible as an aspergilloma …
Sorry, “right” breast, of course 🙂 …
Why do I miss the shadow of the right breast? Should we think about immunosuppression in consequence to chemotherapy due to breast cancer? Then a not really typical tbc is also possible as an aspergilloma …
Patient has both breasts. No problem with them.
Aspergillosis
Extensive bronchocele in left upper lobe with reduced interstitial makings. Pectus excavatus.
Cause: ABPA? Atresia of culmen bronchia with collateral air drift?
Hyperlucency of left UL (apicoposterior) with nodular/tubular structures – segmental bronchial artresia with Air-trapping and mucoid impaction?
Vascular malformation. Probably anomalous return of the polmunary vein of the left upper lobe.
I see apicoposterior hyperlucent upper lobe,with fibrotic changes in a border of it…there is a one central positioned round calcification within it,which possibly be a tuberculoma…dilatated vascular structures locoregional is a probably due tu fibrotic changes which surround them…cut off left hila indicated fibrosis or compression…i vote for old drainaged abscessus,aspergiloma 🙂
Don’t you think fibrotic changes will pull up the hilum?
of course,but there is another slow expansive process,which defeated the force of athesion and traction…
Don’t complicate things. What process gives hyperlucency and finger-like shadows?
ABPA
It´s true bronchial atresia gives finger-like lessions, but ABPA too, doesn´t it?
Vascular malformation.
There is hyperlucency with minimal atelectatic changes as well as prominent vascular markings in the left upper zone, I think it is sort of vascular malformation.
4. Bronchial atresia
Correct. It is a matter of putting together the information that the radiograph offers.
Muppet happy!
We already knew it! In fact, it is very prevalent in our planet, Tatooine…
Sent from my i-Millenium Falcon
Muppet belongs to a different generation and honors Admiral Adama.
And Sheldon.
Buzinga!
Broncoceli da Atresia di un bronco con iperventialzione del territorio polmonare corrispondente ( air-trapping ) attraverso i canali di Kohn.
Tuberculosis
ABPA or bronchial atresia
buy burberry outlet to take huge discount