ECR Today – Cardiac imaging in 2020: reaching new heights
Watch this session on ECR Live: Thursday, March 7, 16:00–17:30, Room D2
Over the past decade, technological improvements have led to the widespread use of imaging modalities in the prediction, diagnosis and follow-up of coronary disease. Radiologists now have the ability to obtain information on the structure of cardiac muscle with MRI and evaluate cardiac arteries with CT, while hybrid imaging will soon allow them to do both. Cardiac CT will also provide more functional information in the future, and its use will continue to grow. Experts will present the newest and upcoming possibilities of cardiac imaging today at the ECR.
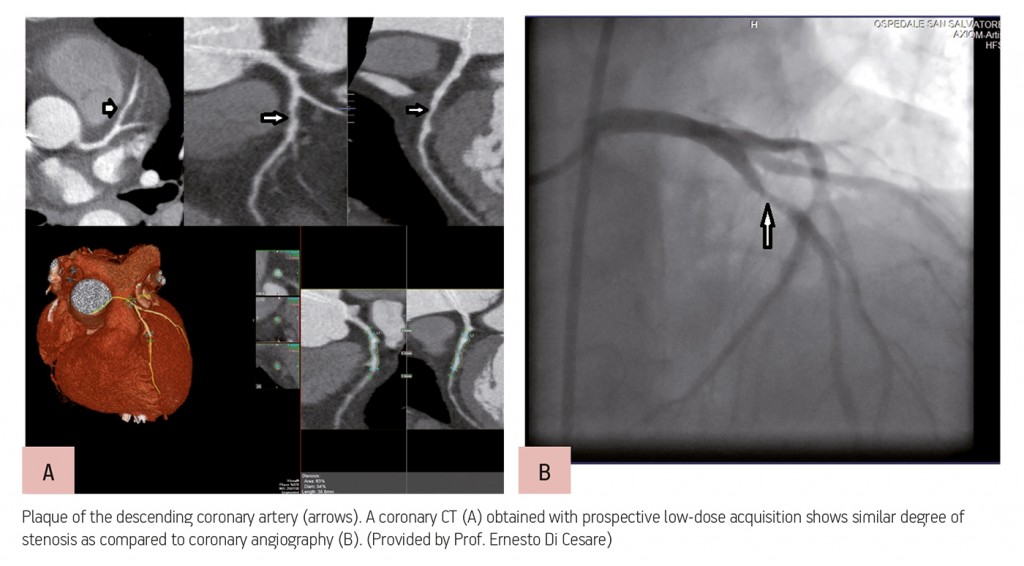
Advances in cardiac CT have brought its use in clinical routine to unprecedented levels. The main reason is that image acquisition optimisation strategies allow radiologists to assess blood vessels with the same efficiency as coronary angiography, non-invasively and almost instantaneously.
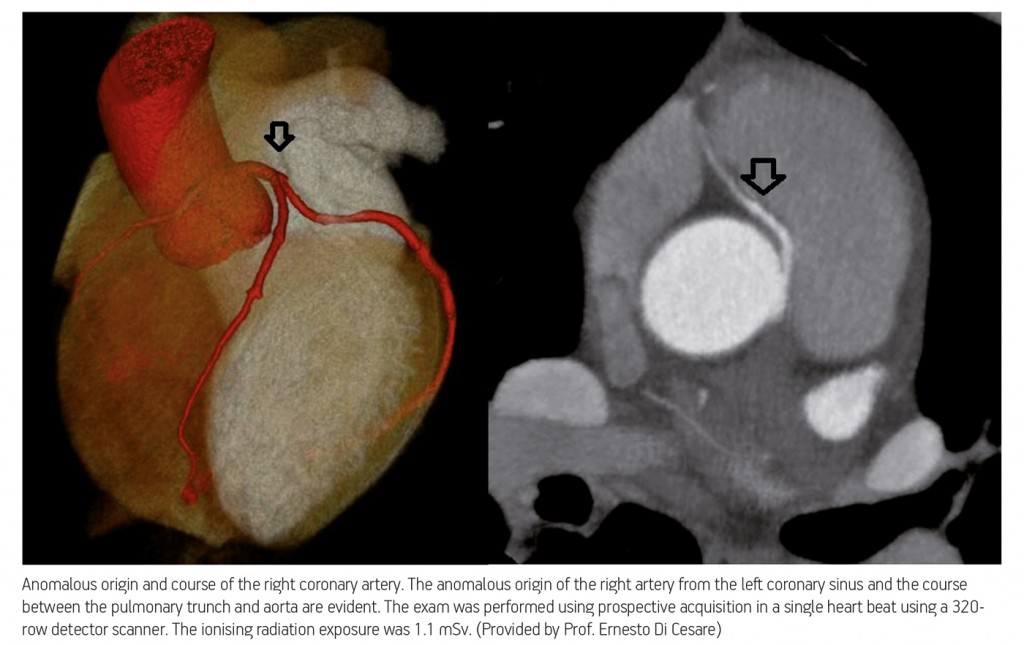
“CT is considered a wonderful technique for the evaluation of coronary arteries. It is really similar to coronary angiography, but without the risks. With new apparatus, we have the ability to produce imaging very fast, reduce artefact, but especially reduce the dose of radiation in each patient,” said course moderator Professor Ernesto Di Cesare, chairman of the radiology department at L’Aquila University Hospital in Italy.
Cardiac CT use in clinical routine will continue to rise in the near future. A paper published by the British Cardiovascular Society predicts that the number of cardiac CT examinations carried out will increase by up to 40 times by 2020. “The use of cardiac CT is bound to increase and, by the next decade, it could penetrate everyday work, in both specialised and non-specialised centres,” said Konstantin Nikolaou, professor of radiology and vice-chair of the department of clinical radiology at Munich University Hospital in Germany.
These projections mean that CT will also replace catheter angiography in some cases. Experts agree that CT could replace invasive angiography to rule out coronary artery disease (CAD) in selected patients with chest pain, in whom suspicion of coronary artery disease is not so strong.
“I think that CT will be used on an individual basis in patients less likely to suffer from CAD, to diagnose and characterise the atherosclerosis before the symptoms occur. At the moment, CT seems the most reliable tool for this evaluation,” predicted Di Cesare.
To become a clinical standard, CT must be backed up by solid scientific evidence, available only after randomised prospective multicentric studies. “Radiology and cardiology have to prove with large clinical trials that cardiac CT is effective and efficient, meaning it can provide the right results while remaining economically reasonable as compared to currently used diagnostic work-up,” Nikolaou said.
Cardiologists and radiologists are currently waiting for the results of two large studies in particular. The Rule Out Myocardial Infarction/Ischemia Using Computer Assisted Tomography (ROMICAT II) trial aims to show that cardiac CT can be used in patients with acute chest pain, while the PROMISE trial looks at patients with stable chest pain. For the latter, 64-slice CT was tested against the conventional standard of care (ECG, lab tests, etc.), to show if a single CT examination can spare patients further tests.
By 2020, cardiac CT will have undergone further technical developments. Major advances have been made over the past five years to optimise image acquisition and reduce dose; specialised centres can now operate cardiac CT using one mSv. This dosage will become standard practice as demand for CT examinations grows, Nikolaou believes. “I would expect that, by 2020, we will be in the range of two mSv or even less in most diagnostic cardiac CT studies. We can say it’s an optimistic way of seeing the future, but at least we should hope that, as soon as cardiac CT is used more and more frequently, any dose reduction algorithms available should be known and used by the radiologist performing the examination.”
This knowledge will be supported by increased automatic selection of technical parameters to reduce dose, Nikolaou believes. For example, automated selection of tube voltage has been introduced recently, and it already helps radiologists decide which tube voltage should be chosen in each patient, minimising radiation dose as much as possible.
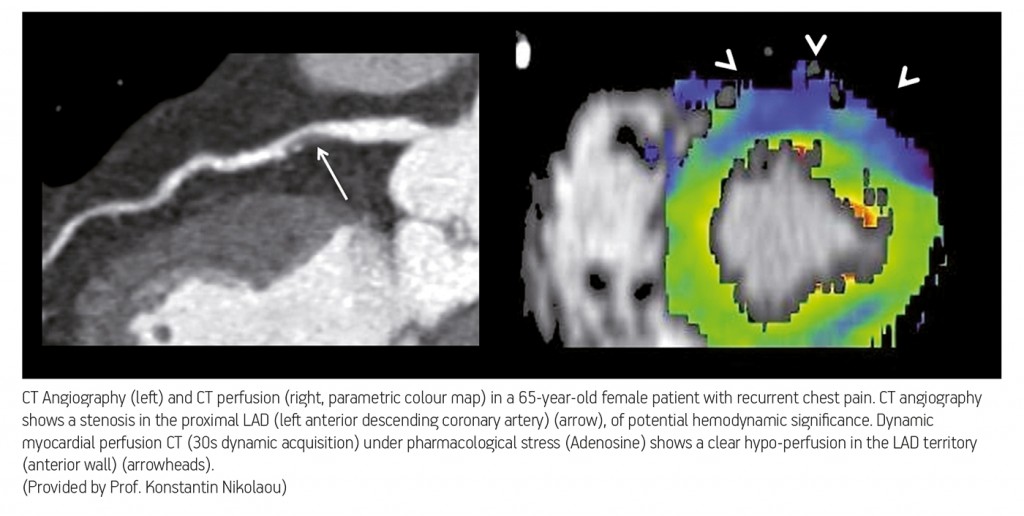
CT scanners will also provide more and more functional information on the myocardium, by enabling radiologists to evaluate whether a stenosis is reducing blood flow to the myocardium or not. “Today you would normally perform an angiographic CT scan to look at the coronaries and see if there is morphological stenosis, but soon we might perform an additional type of CT scan, to assess whether this stenosis will lead to ischaemia, so whether it is reducing blood flow to the myocardium or not. This is very important information for cardiologists,” Nikolaou said.
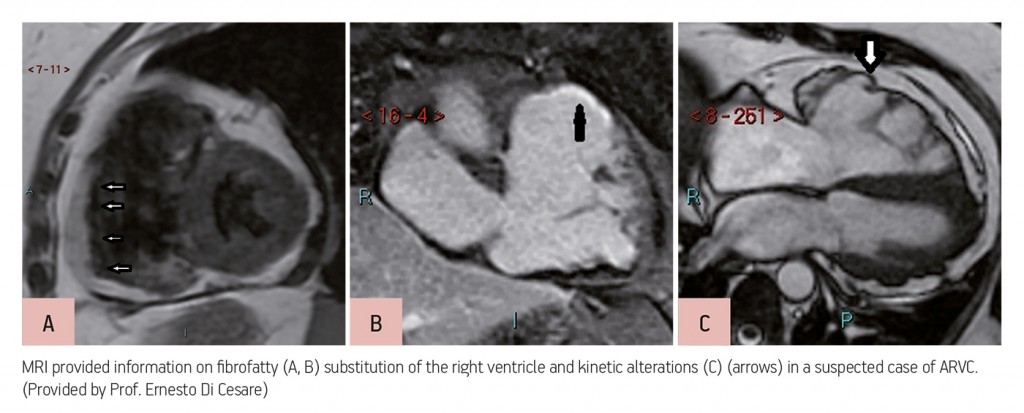
Hybrid imaging, in particular PET-CT and the recently introduced MR-PET, should also offer information on both the myocardium and coronary arteries by 2020. Heart MRI, the golden standard for imaging the myocardium, will undergo several transformations, but this is further down the road, according to Di Cesare. Researchers are currently testing the possibility of evaluating the myocardium with magnetic field strengths higher than 1.5T. “So far they haven’t been very enthusiastic about the results, but things could change soon. Heart MRI is a very fast evolving modality. In the beginning we used low field, right now we are using medium field, and I think that in the far future we could improve the evaluation with fields beyond 3T, helped by the development of new sequences, and provide new information about the heart structure,” he said.
Refresher Course: Cardiac
Thursday, March 7, 16:00–17:30, Room D2
RC 303: Cardiac imaging: the cutting edge
Moderator: E. Di Cesare; L’Aquila/IT
A. Cardiac MRI: do we need more than 1.5T?
B.J. Wintersperger; Toronto, ON/CA
B. Cardiac CT: technique in 2020; where to next?
K. Nikolaou; Munich/DE
C. Cardiac hybrid imaging: ‘One-Stop-Shop’
P.A. Kaufmann; Zurich/CH



“A recent paper published by the British Cardiovascular Society predicts that the number of cardiac CT examinations carried out will increase by up to 40 times by 2020.”
Does the author have a reference for the paper mentioned here? I would like to read it.
Of course, you can find the source here:
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC1861505/
(Table 1)
All the best.