Dr. Pepe’s Diploma Casebook: Case 15 – SOLVED!
Dear Friends,
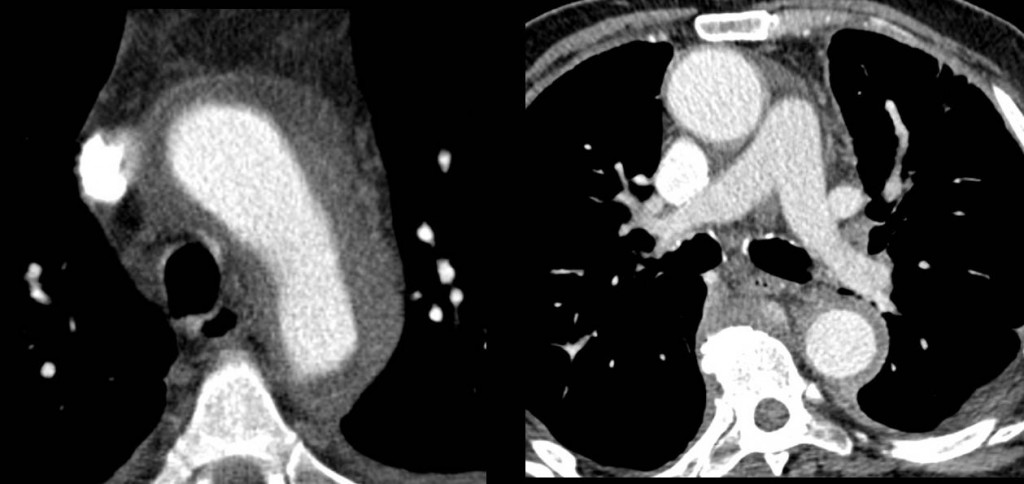
I have decided to show you a nice case before your Christmas holidays. Enhanced axial CT of a 69-year-old man with bone pain.
Diagnosis:
1. Aortic dissection
2 Intramural hematoma
3. Fibrosing mediastinitis
4. None of the above
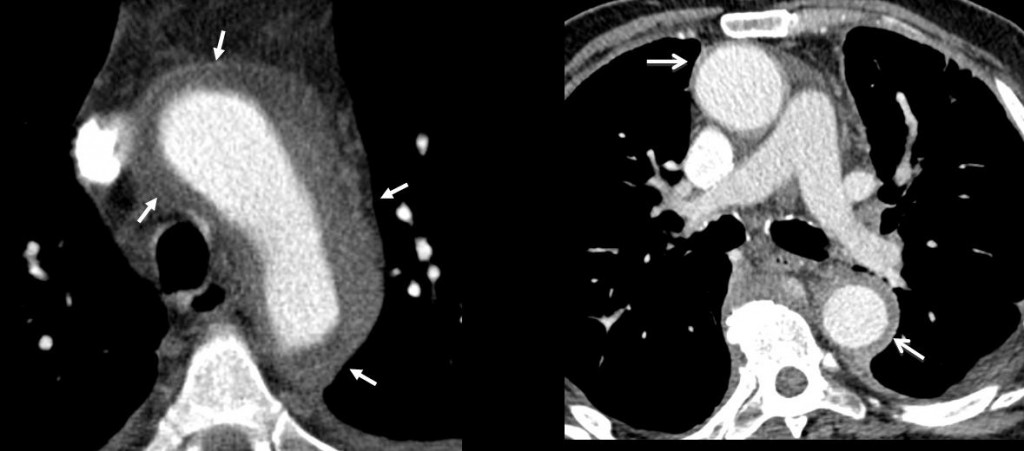
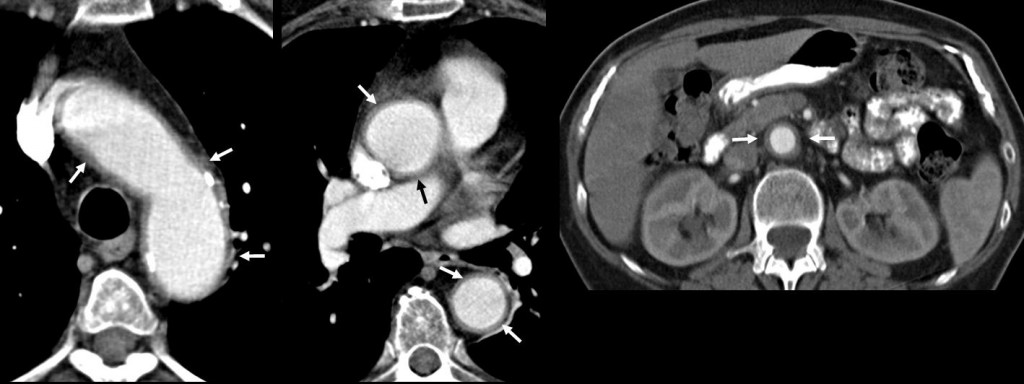
Findings: there is diffuse concentric thickening of the aortic wall (arrows), affecting the ascending and descending aorta. Of the proposed diagnoses, aortic dissection is characterised by an intimal flap separating the true and false lumen, which is not seen in the images. Intramural aortic haematoma is characterised by a high-attenuation crescent-shaped thickening of the aortic wall (ie. only a part of the aortic wall is affected).
It would be highly unusual for fibrosing mediastinitis to affect the aorta without involving other mediastinal structures.
Concentric aortic wall thickening is highly suggestive of diffuse aortitis.
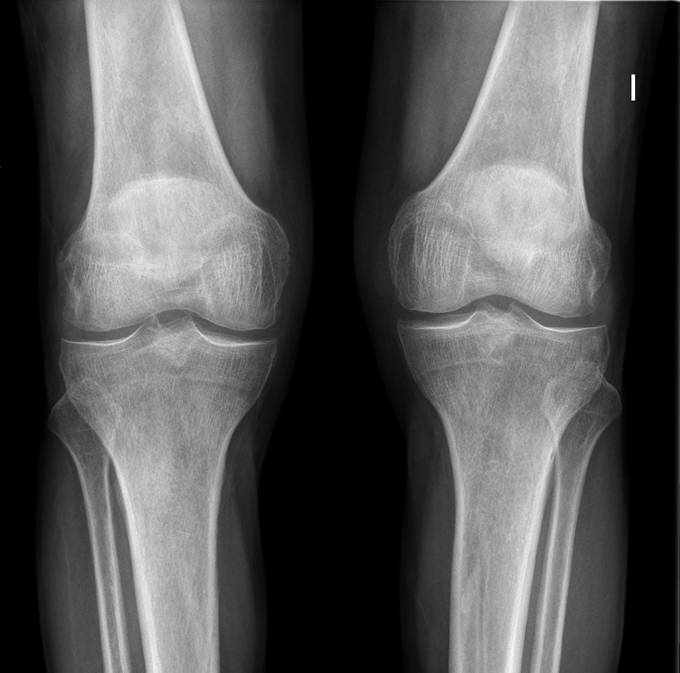
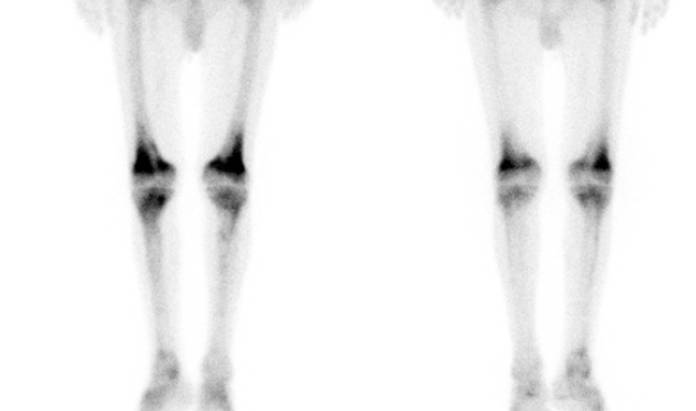
In this particular patient, radiographs of the knees shows heterogeneous osteosclerosis suggesting Erdheim-Chester disease (ECD) as the possible cause.
Final diagnosis: periaortitis in Erdheim-Chester disease.
Aortitis refers to an inflammatory condition of infectious or (more commonly) noninfectious origin involving the vessel wall.
Non-infectious aortitis (mainly affecting the medial layer) occurs in large-vessel vasculitides, such as Takayasu arteritis and giant cell arteritis (GCA). It is also seen in other collagen vascular disorders, such as rheumatoid arthritis, ankylosing spondylitis, and relapsing polychondritis. Other conditions mainly cause periaortic disease (affecting the adventitia and periadventitial spaces) such as chronic periaortitis (retroperitoneal fibrosis), immunoglobulin G4-related periaortitis, and Erdheim-Chester disease.
All the conditions mentioned above present with similar CT findings: concentric aortic wall thickening.
The age of the patient, the clinical setting, and in some of these diseases, possible systemic manifestations, are a key to the differential diagnosis.
Giant cell arteritis (GCA), the most common vasculitis of large and medium-sized arteries, occurs almost exclusively in individuals over 50 years of age.
The disease predominantly affects the extracranial carotid branches (causing headaches) and the aorta, and rarely, the central pulmonary arteries.
Fatigue, weight loss, low-grade fever, polymyalgia rheumatica, arthralgia, and tenosynovitis occur alone or in combination in more than half of patients with GCA.
GCA patients are more likely to develop aortic aneurysm and dissection; hence, aortitis must be investigated in this condition so that intensive treatment can be established to prevent long-term aortic complications.
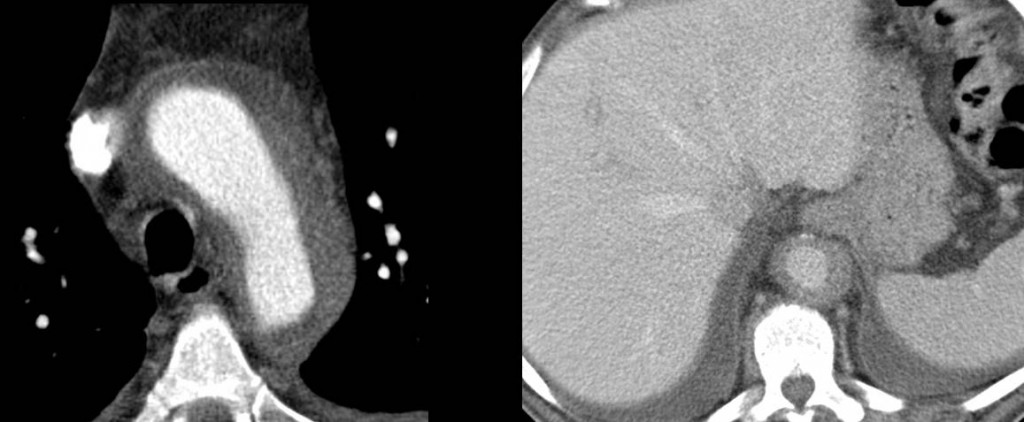
Fig. 5 (above) is a 68-year-old woman with GCA, presenting with severe headaches, fatigue, weight loss, and shoulder girdle pain. Note the concentric thickening of the wall of thoracic and abdominal aorta (arrows).
Takayasu arteritis (TA) is a chronic idiopathic arteritis resulting in large artery stenosis; it has a strong predilection for the aortic arch and its branches. TA is also known as ‘pulseless disease’ because of common involvement of the subclavian arteries with substantial stenosis and subsequently, decreased peripheral pulses. Although it is more common in Asia, the disease is found worldwide and usually affects young women.
Because the clinical and laboratory findings are typically non-specific, accurate diagnosis of TA virtually always depends on imaging studies. Both CT and MRI can provide information on vessel wall thickening in the early stages, and on luminal narrowing, aneurysmal dilation, and occlusion in advanced (fibrotic) stages.
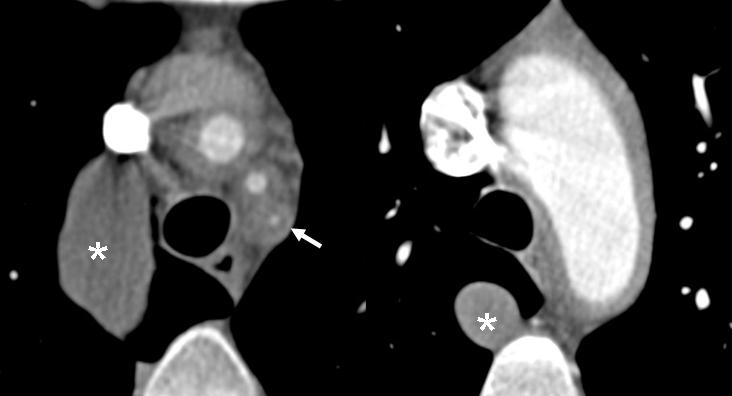
Fig. 6 (above) shows Takayasu arteritis in a 30-year-old woman presenting with decreased left arm pulse and left arm weakness. Contrast-enhanced CT. a) concentric wall thickening of the supra-aortic trunks with obliteration of left subclavian artery (arrows) and b) concentric wall thickening of the aortic arch. Unrelated enlarged azygous vein (asterisk) is due to congenital interruption of the inferior vena cava.
Erdheim-Chester disease (ECD) is a rare non-Langerhans cell histiocytosis, characterised by xanthomatous infiltration of the affected tissue by foamy histiocytes surrounded by fibrosis. It is a true systemic disease with bone involvement in almost all cases and extra-osseous involvement in 60% of patients, including retroperitoneal infiltration, cardiovascular abnormalities (‘coated’ aorta), central nervous system involvement, exophthalmos, xanthelasma palpebrarum, and interstitial lung disease.
CT images typically show periaortic tissue extending from the ascending to the abdominal aorta creating the ‘coated’ aorta appearance. ECD affects the adventitia and periadventitial spaces, and spares the media and intima. Nonetheless, the radiologic appearance is identical to aortic wall involvement because no demarcation line is seen between the periadventitial infiltration and the aortic parietal tissue.
Infectious aortitis is an inflammatory infectious process of the aortic wall induced by microorganisms. The aorta is normally very resistant to infection; however, an abnormal aortic wall, such as that associated with atherosclerotic disease, pre-existing aneurysm, cystic medial necrosis, diabetes, vascular malformation, medical devices or surgery, is more susceptible to infection.
Mechanisms of infection include hematogenous spread, contiguous seeding from adjacent infection, and traumatic or iatrogenic inoculation.
The CT manifestations of this condition are aortic wall thickening, periaortic fluid or soft-tissue accumulation, rapidly progressing saccular aneurysm or pseudoaneurysm, and occasionally, air in the aortic wall.
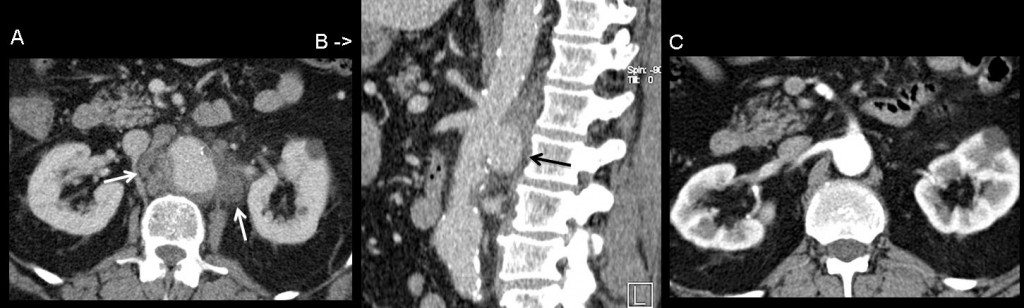
Fig. 8 (above) Infectious aortitis in a 60-year-old man with bacterial endocarditis. Contrast-enhanced CT a) depicts aneurysmal dilatation of the aorta and periaortic fluid accumulation (arrows). b) Sagittal reformatted image shows a rapidly progressing saccular pseudoaneurysm (arrow). Compare with image c) performed two weeks before.
Follow Dr. Pepe’s advice:
- Extensive concentric aortic wall thickening suggests abnormal inflammation of the aortic wall (aortitis).
- The age of the patient, the clinical setting, and in some conditions, the potential systemic manifestations are a key to the differential diagnosis.
- Giant-cell aortitis is the most common type of aortitis in patients over 50 years of age.
Suggested reading:
- Aortitis: Imaging spectrum of the infectious and inflammatory conditions of the aorta. RadioGraphics 2011; 31:435–451
- Insights into imaging for aortitis. Insights in imaging 2012;3:545-560.
Case prepared by Eva Castañer, MD




Confluent regular high attenuation mural thickening involving the aorta, without surrounding peri-aortic fat stranding. The thickening seems to be eccentric at the arch, and more concentric at the descending thoracic aorta.
No intimal flap is seen.
This does not appear to enhance (although we have to see the pre-contrast sequence to confirm this).
The features are mostly suggestive of aortic intramural haematoma, as opposed to aortitis (the latter usually shows peri-aortic fat stranding, and is usually more segmental).
Fibrosing mediastinitis
2.Intramural hematoma.
Fibrosting mediate its
Periaortitis
It goes with systemic simphoms.
Vi è una prima osservazione di tipo clinico:la dissecazione aortica, insieme all’ematoma intramurale, fanno parte conl’ulcera aterosclerotica della SAA( Sindrome Aortica Acuta) che non è riportato nel soggetto che invece si lamenta di un dolore osseo!.In secondo luogo è l’imaging che esclude queste due patologie, non dimostrando il”flap” intimale nella dissezione ed i segni( es.placche calcifiche…) dell’amatoma intramurale, di cui non si dimostra l’esame precontrasto.Si dimostra invece una presenza di T.solido iperintenso, “localizzato”in sede medio-posteriore ove si osserva un lume eofageo pervio, cranialmente e che poi si riduce a 2 piccole bolle aeree in un esofago a pareti ispessite.In vicinanza dell’esofago, si intravede un tramite ipointenso, probabilmente fistoloso; adenopatia all’angolo di divisione della polmonare. CD Tumore esofageo, fistolizzato, con mediatinite localizzata e metastatizzato all’osso(dolore osseo!).
Nothing of the above. There is a perivertebral mass that I believe is assosiated to the imaging finding of aorta (aortitis?).
Erdheim-Chester disease
Bone pain is the most frequent symptom.
Soft tissue infiltration of the aortic arch.
Infiltration may occur around the pulmonary arteries, superior vena cava, pericardium.
it is possible pericardial effusion and pulmonary oedema.
OK?
OK
Dove sono le alterazioni “ossee”., della Erdheim-Chester?.Non sono state allegate nella TC!
Post-contrast CT angiogram of the thoracic aorta.
There is haemorrhage within the aortic wall with no intimal tear (a pre-contrast scan is necessary to confirm this). It maintains a circumferential relationship with the aortic lumen. The aortic lumen is not compressed. No aortic calcifications are present.
Appearance is in keeping with an aortic intramural haematoma. Pre-contrast CT is required for confirmation of this finding and exclusion of aortic dissection (intramural haematoma is thought to be a precursor of this entity).
Wonderful discussion and differential diagnosis. Many thanks.