
Dear friends,
Here is an easy case to facilitate the transition into the new year.
Sixty-seven year old lady with dyspnea for about a month. Previous history of bronchiectasis.
Diagnosis:
1. Infected bronchiectasis
2. Pulmonary embolism
3. Bonchioloalveolar carcinoma
4. Pleural disease
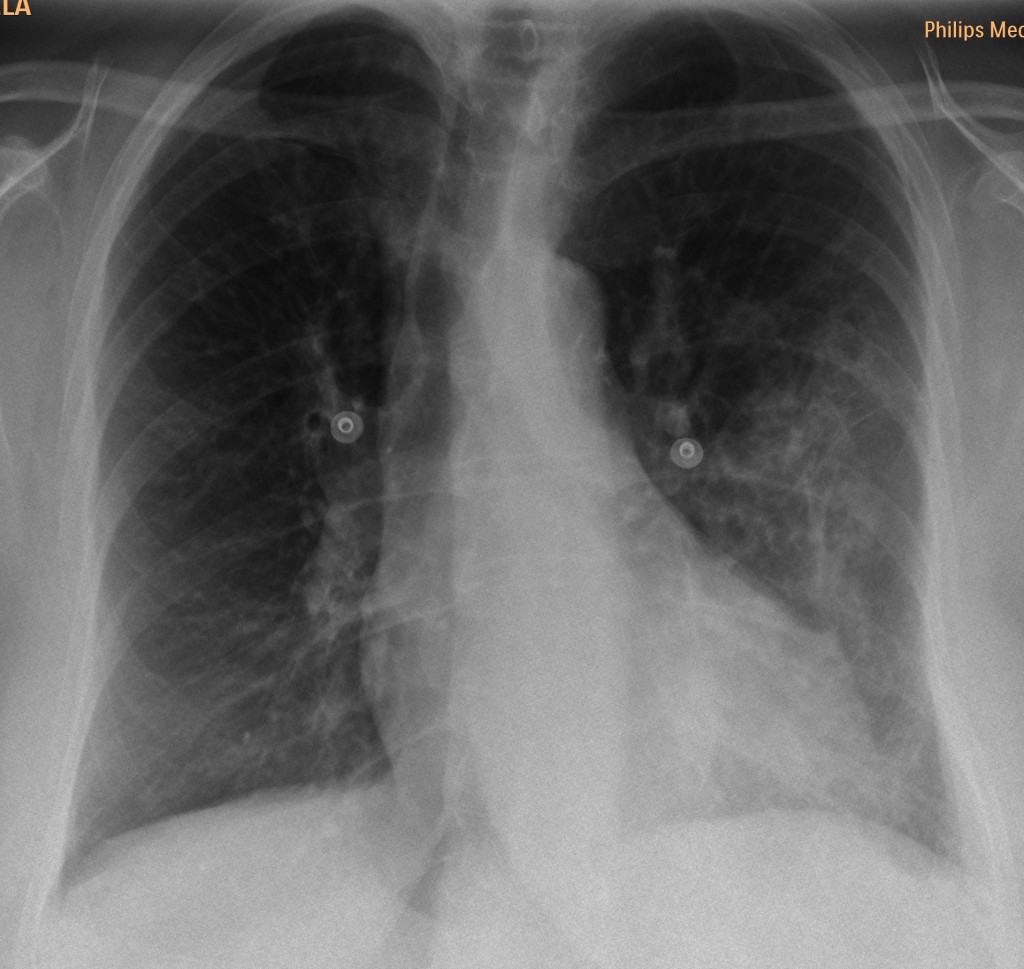
67 year old female, PA chest
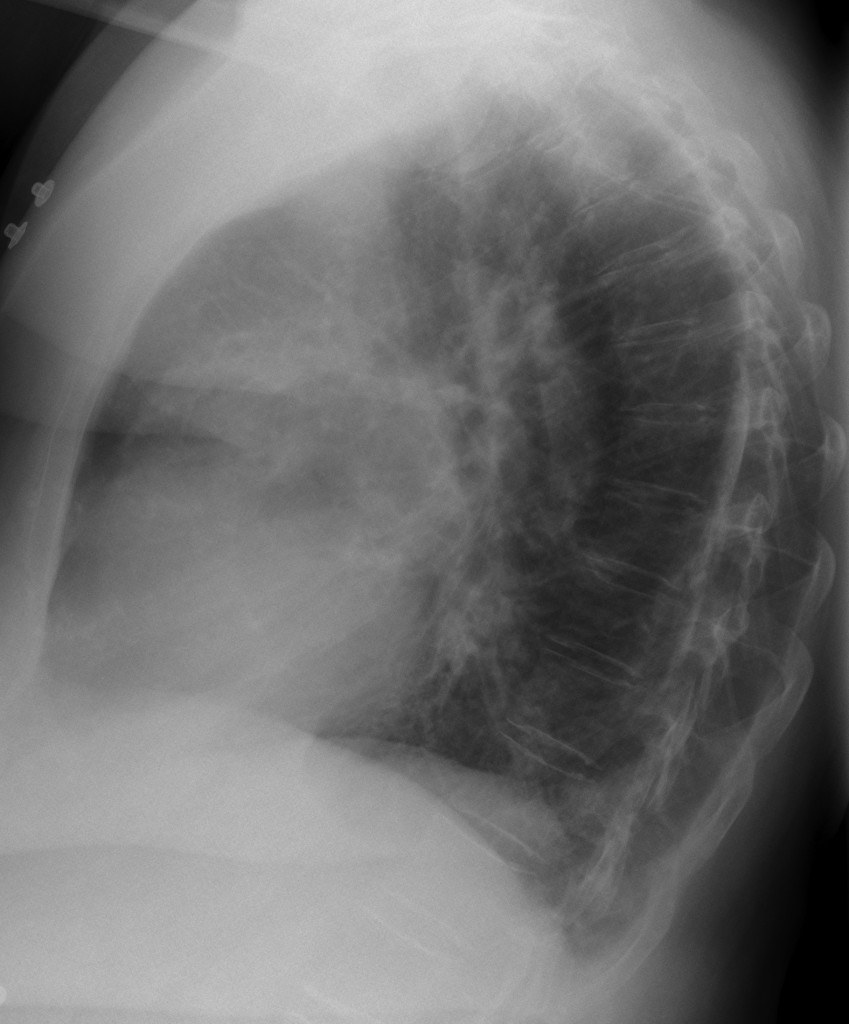
67 year old female, lateral chest
Click here for the answer to case #9
Of the four options offered, the first three cannot be diagnosed with confidence. However, obvious pleural calcification is visible on the lateral view, (arrows), which makes option 4 (pleural disease) the most likely diagnosis. This is a good example of calcified pleura seen on face on the PA view, simulating lung disease. CT confirms the diagnosis (arrows). Incidentally, no bronchiectasis was seen, which makes us wonder about the acumen of our clinical colleagues.
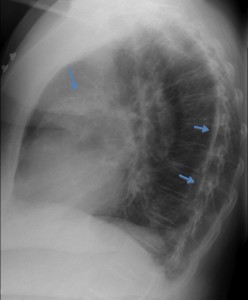
Answer case 9-1
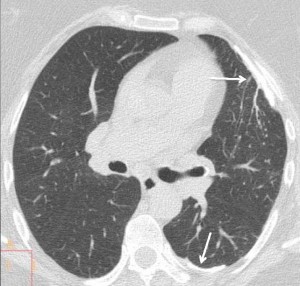
Answer case 9-2
Congratulations to all of you who made the diagnosis. It made Muppet very happy!
Teaching point: 1. Calcified pleural disease may have a bizarre appearance, which may be confused with lung disease unless one recognises it.
2. Always look at the lateral view. You never know when it’s going to help!







Is it “really” easy? Bronchiectasis are clearly visible on the left in the frontal view, along with a blunted left posterior CF angle in the lateral one. Acinar opacities and peribronchial cuffing coexist on the same side. No adenopathies. No visible bony mets. Tracheal deviation noted. Hyperlucency w/o obvious hilar abnormalities. I would choose the answer #1: acute on chronic inflammatory process (infected bronchiectasis).
IMO trachea is not deviated . its due to asymetry,,,
I agree. Patient is slightly rotated towards the right
Happy New Year!
Bonchioloalveolar carcinoma.
Bonchioloalveolar carcinoma
Infected Bronchiectasis
in addition to the bronchiectesis on the left there are signs of pleural disease and thickening
-on frontal veiw :
left lateral thick plura with some longitudinally oriented lines with a degree of over all decrease translucency on the lower 1/2 of left thorax
doubling of the left cardiac shadow (mediastinal pleura)with possibil adherence to pericardium
– on lateral veiw :
posterior longitudinal line
obliteration of posterior costodiafragmatic angle .
but still thinking of some signs of fibrosis and pulmonary volume loss in the left pulmonary base which may be secundary to br. alv. cancer
so my choise is between 3 and 4 .
happy new yr
Hi all,
Ok let me attempt…
67 year old lady with complaint of dyspnea since 1 month.
Infected bronchiectasis is ruled out by history as infected bronchiectasis has to have presence of fever and cough with expectoration (since the bronchiectasis is in the lower lobe) also.
Coming to next option of Pulmonary embolism – dyspnea in absence of chest pain, less likely but possible. Especially when pleural disease is present as many a times the only presentation is minimal pleural effusion which on tapping is hemorrhagic.
Bronchoalveolar carcinoma, the only favouring feature is her old age. The trachea seems to be shifted to the right but also there is right posterior oblique rotation of the patient. So commenting on mediastinal adenopathy seems to be difficult however apparent mediastinal widening is not present nor any sign of malignancy like rib destruction.
Next option, pleural disease is definitely present. I can appreciate the blunting of posterior cp angle.
So my answer would be option 4(pleural disease) followed by option 2(pulmonary embolism).
Happy new year ! Here’s what i see: left sided bronchiectasis; small left pleural effusion; mediastinal shift to the right; no gastric air bubble; some lucent bands (air tracks) in the mediastinum -paratracheal (mostly left side), retrosternal and doubling the left inferior arc; retrotracheal air band (air stasis in oesophagus?). Can’t figure out a linear band oblique in the middle left pulmonary area descending toward the heart (might mess the whole diagnosis, might just be a parenchymal band in superior lingula). Does the patient has a history of dysphagia? Fever ? Fistula (eso-pleural) maybe secondary to esophageal neoplasm is one dx. Lingular lucency is highly inhomogenous; plus the air trapping (shifting the mediastinum) – those i can’t figure (yet) but awaiting more clues (at list if she has dysphagia / fever).
Needs CT Thorax-superior abdomen + oral positive contrast media.
? 1 & 4
Translucent esophagus in uperr two thirds/presbioesophagus or substenosis distal,extramural compression.
Compressed and narowed left tracheal wall/precarinal part.
On lateral chest,i see lobular calciphication in sumation with heart and aorta ascedens…pathology of midlle part of mediastinum i sugest,maybe pericard cist dif.dg. mediastinal pleura or pleuropericard pathology,stigmata TBC maybe,few athesions locoregional…
Anyway,happy new year and wish you all good eye!!! 🙂
-small cystic an reticular opacities involving left mid and lower zones.
-pleural thickening/effusion on left side suggested by blunting of CP angle and the adjacent opacity.
left pulmonary process appears chronic;may represent superinfection if clinical/lab values correlate.
pleural effusion can also result in new onset dyspnoea.
HRCT chest for furthur evaluation.
*happy new year to everybody(including the muppet!!)
Bonchioloalveolar carcinoma
Left sided bronchiectasis with ipsilateral pleural effusion:: Infected bronchiectasis.
Answer to this case will be posted shortly. Some of you already made the right diagnosis. Final comment: of the four answers there is one which cannot be challenged. Which one?
ii suppose it to be infective bronchoectasis…