Dr. Pepe’s Diploma Casebook: Case 112 – The Wisdom of Dr. Pepe (Chapter 5) – SOLVED! (for real this time)

Dear Friends,
The fifth chapter of “The wisdom of Dr. Pepe” is the last presentation of this blog series and ends the present season.
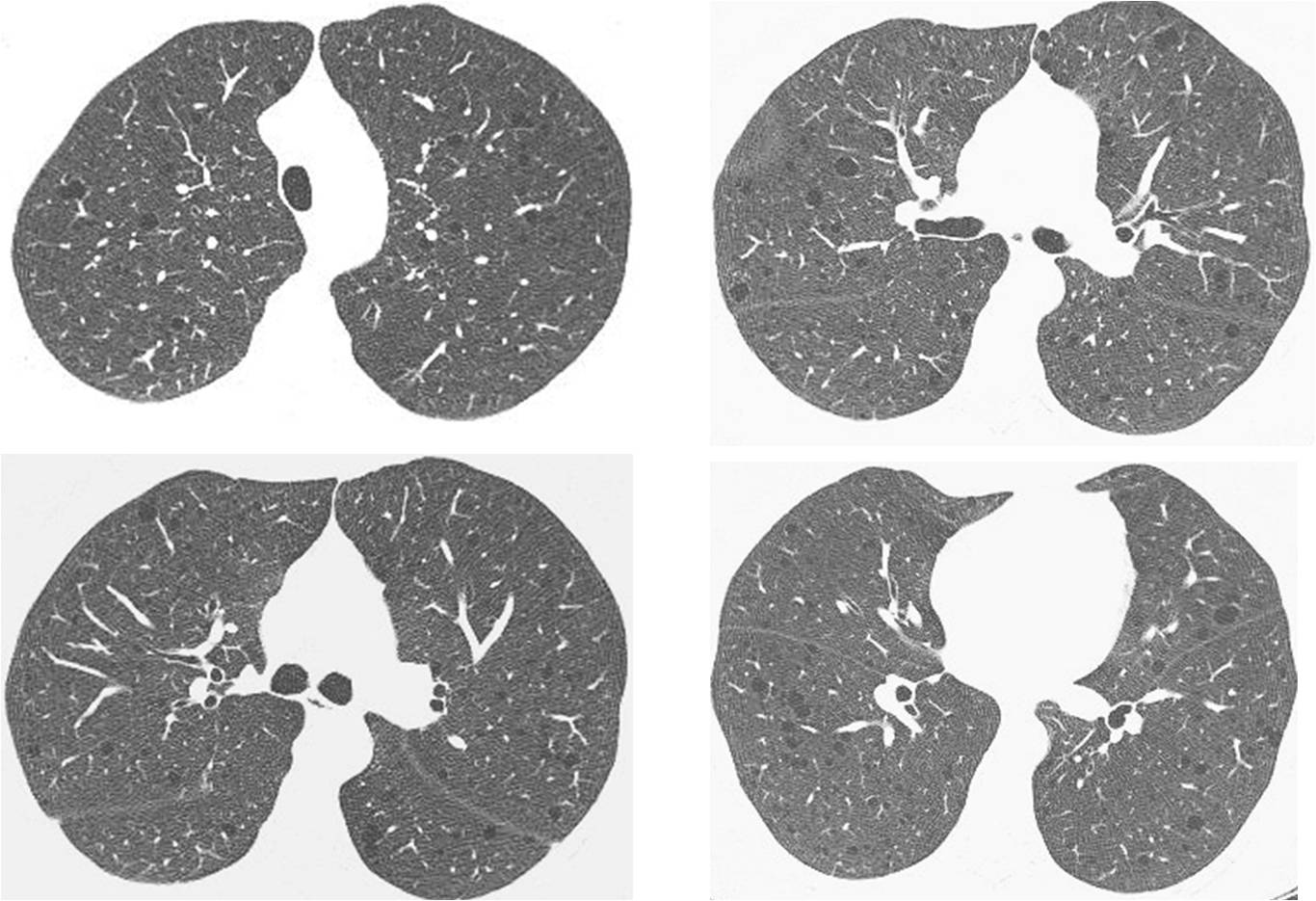
The axial CT images below belong to a 37-year-old woman, who was operated on five years ago for a retroperitoneal tumour. What do you see?
Check the images below, leave your thoughts in the comments section, and come back on Friday for the answer.
Findings: Axial CT images show numerous cystic spaces in both lungs (A and B, circles), several of which have a definite wall around them (A and B, arrows). Review of the clinical history discovered that the patient had undergone surgery for a perivascular epithelioid cell tumour (PEComa). This rare tumor is associated with lymphangioleiomyomatosis of the lung.
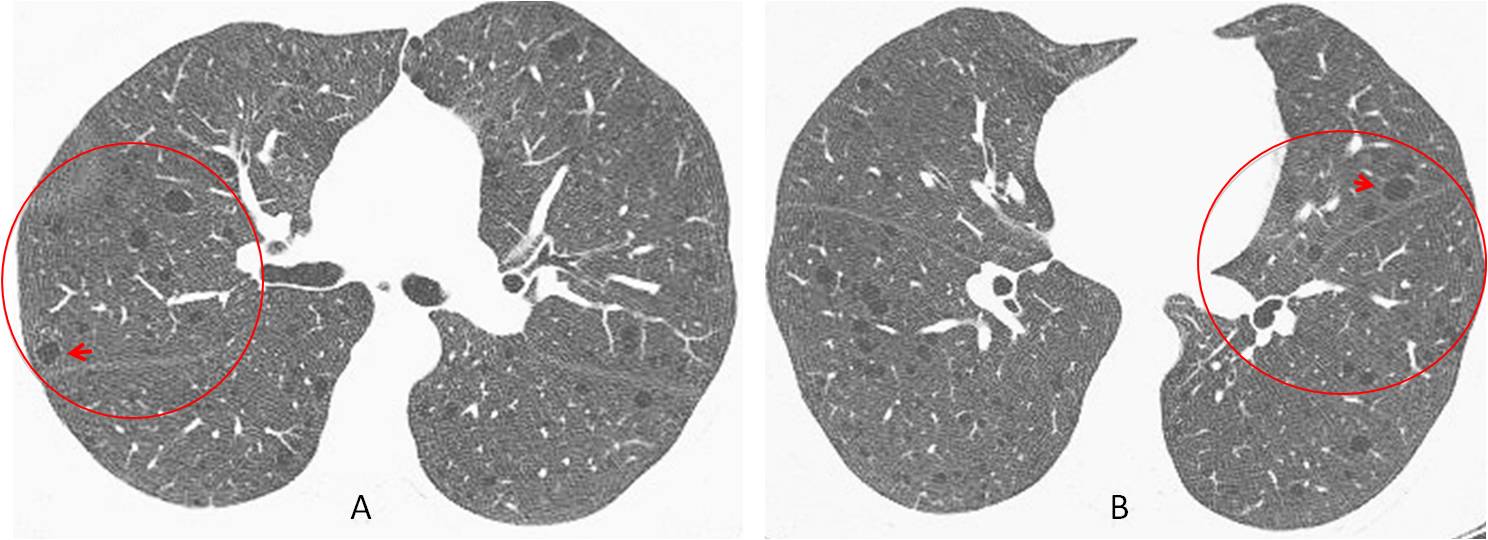
Final diagnosis: lymphangioleiomyomatosis of lung in a patient with PEComa
The case presented has a story behind it. This patient had previous CTs, and the findings were reported as emphysematous changes. The current CT was read by a dedicated radiologist who was not satisfied with the diagnosis of emphysema. He checked the clinical history, found out about the PEComa, and after searching on the Internet, discovered the association with lymphangioleiomyomatosis. As a result of his interest, he gained valuable knowledge and offered a better diagnosis.
In this final chapter of The Wisdom of Dr. Pepe, I intend to discuss enthusiasm (e), the fifth and last component of the equation, a factor that enhances the other four:
D = (bc + lv + ps + chl) e
I have used the word enthusiasm, but I might have chosen motivation or love of work well done. These concepts are basic components of our daily commitment. Without them, our work becomes dull and boring.
To emphasize the importance of enthusiasm I will present two representative cases already discussed in the blog, in which motivation played an important role in the final diagnosis.
CASE 1. In 2011 a chest radiograph in an asymptomatic 49-year-old man discovered an abnormal left lung, interpreted as chronic TB changes. The yearly control radiographs were read as “no change” (Fig. 1).
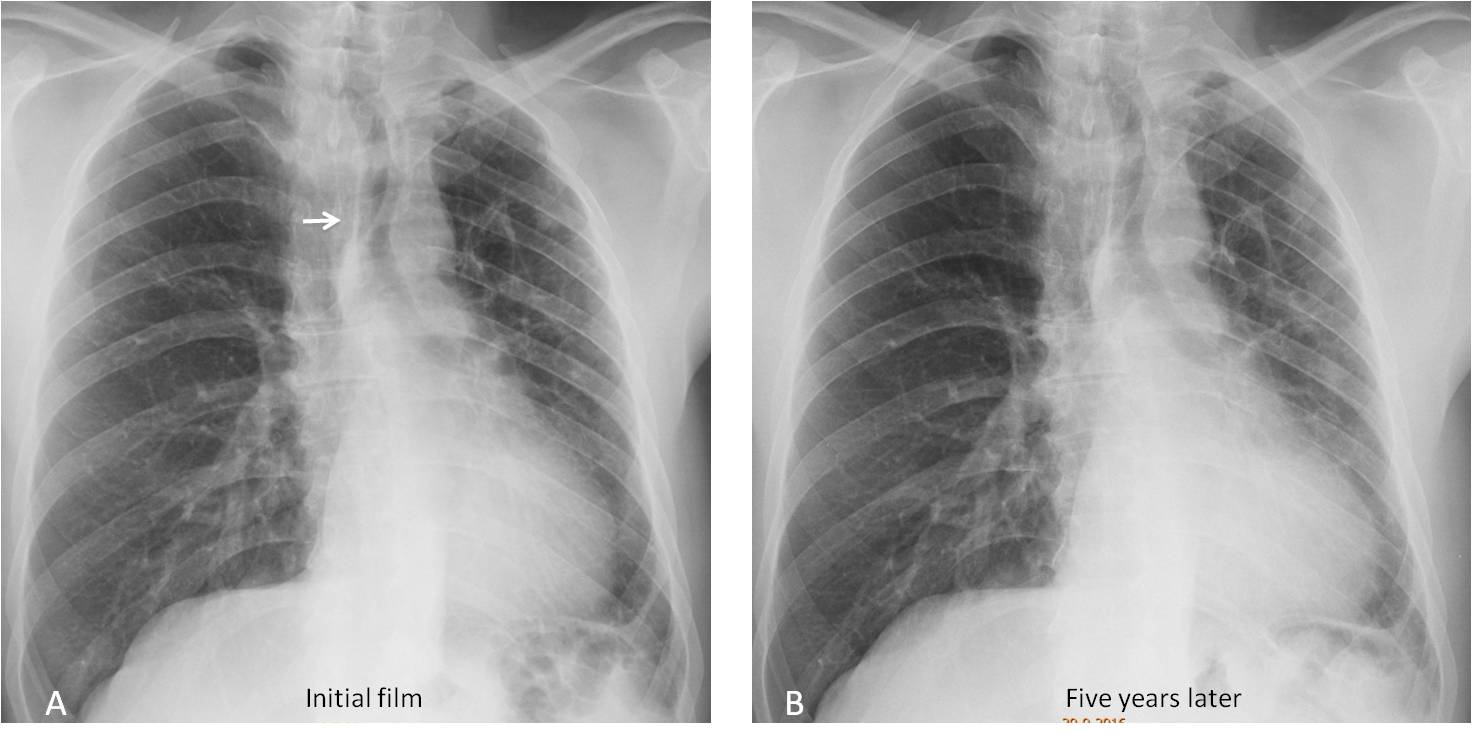
Fig. 1
Fig. 1. The initial PA radiograph shows a small left lung, with mediastinal shift (A, arrow). Five years later, the appearance of the chest has not changed (B).
In 2016 Dr. Carles Vilá, the same radiologist who discovered the PEComa case, was intrigued by the appearance. He spoke to the patient and found no history of previous TB. An expiration film did not show air trapping, excluding McLeod syndrome. Enhanced CT was done to investigate congenital arterial or venous hypoplasia (Fig. 2).
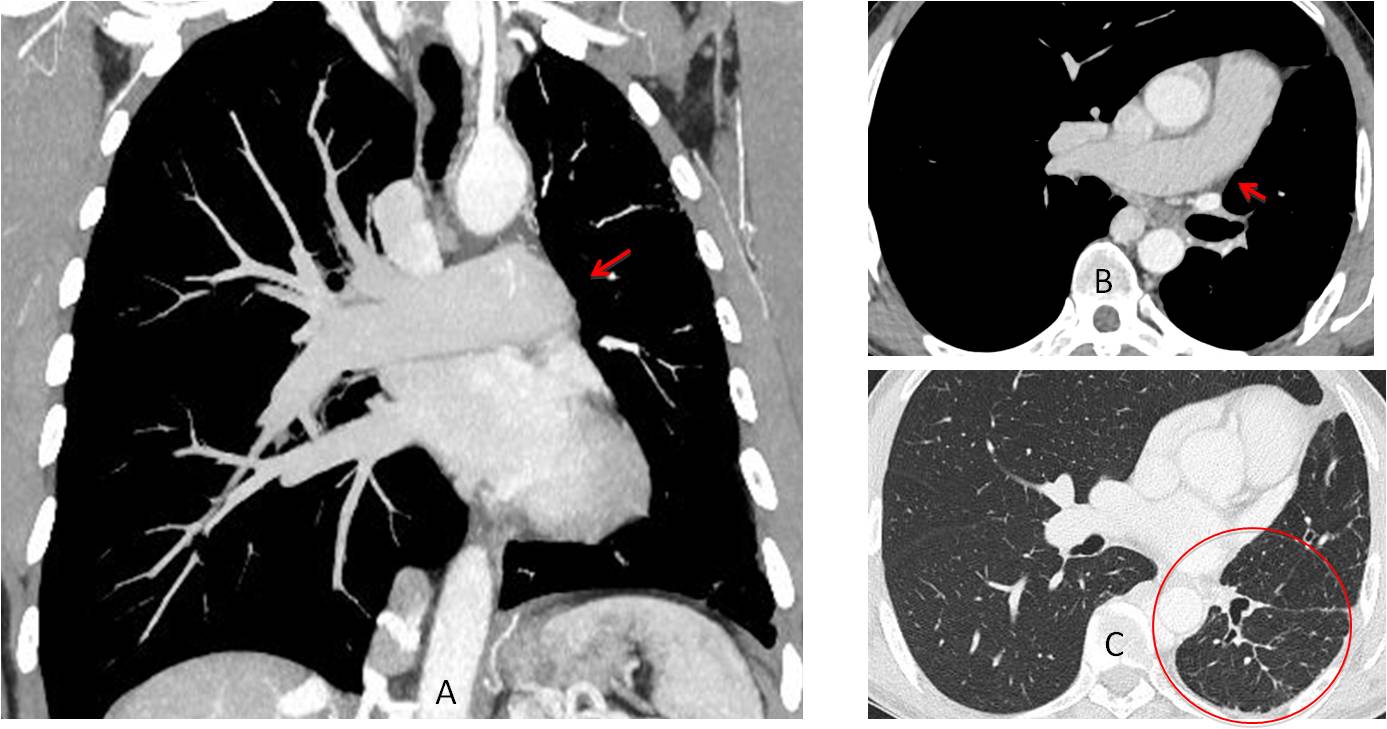
Fig. 2
Fig. 2. Enhanced coronal and axial CT images show that the left pulmonary artery is lacking (A and B, arrows). There is a reticular pattern in the left lung with pleural nodules (C, circle), which represents collateral circulation from pleural vessels.
Final diagnosis: congenital agenesis of left pulmonary artery. This rare condition (I have seen a handful of cases in my entire life) was diagnosed because a radiologist was intrigued about an unusual radiograph and made the effort to investigate it.
CASE 2. In this 41-year-old woman a pre-op radiograph discovered an extrapulmonary lesion. CT was recommended, but no lesion was seen and the study was interpreted as normal (Fig. 3).
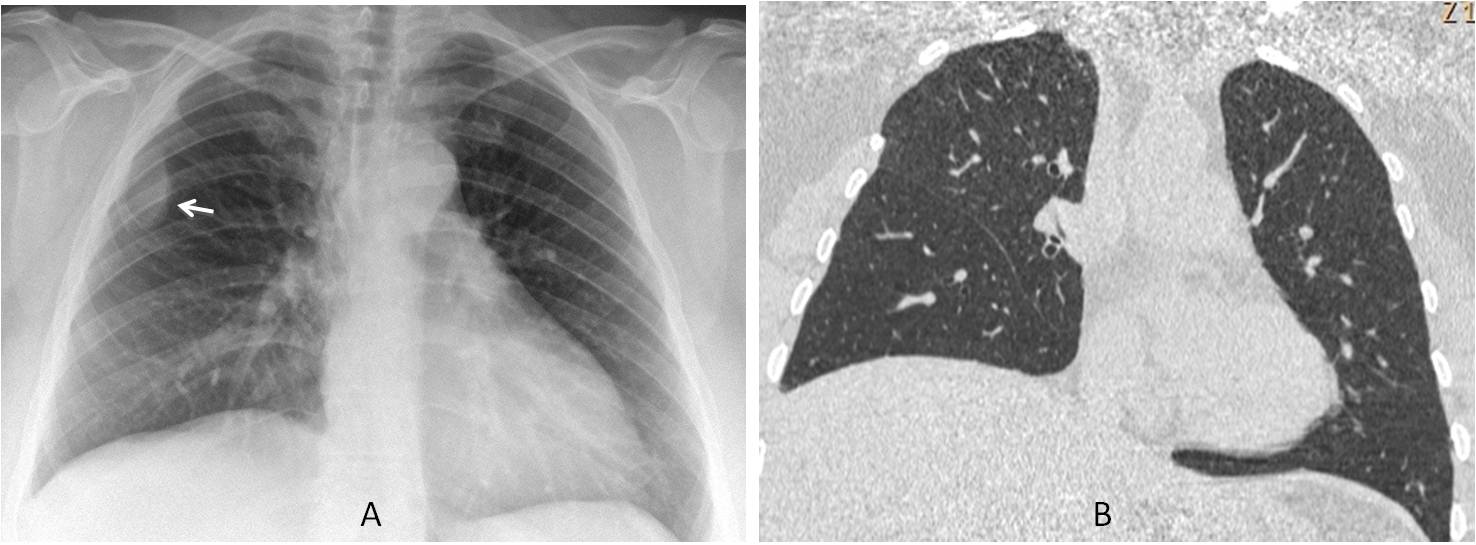
Fig. 3
Fig. 3. Preoperative radiograph shows an extrapleural lesion in the left hemithorax (A, arrow). The lesion is not visible in the CT image (B).
The disparity between the radiography and CT findings prompted us to repeat the chest radiograph, which again showed a lesion (Fig. 4 ). We reviewed the CT and found that the lesion was visible in the scout film but not in the axial view. A careful review of the images showed an intercostal gap with atrophy of the intercostal muscle at the same level.
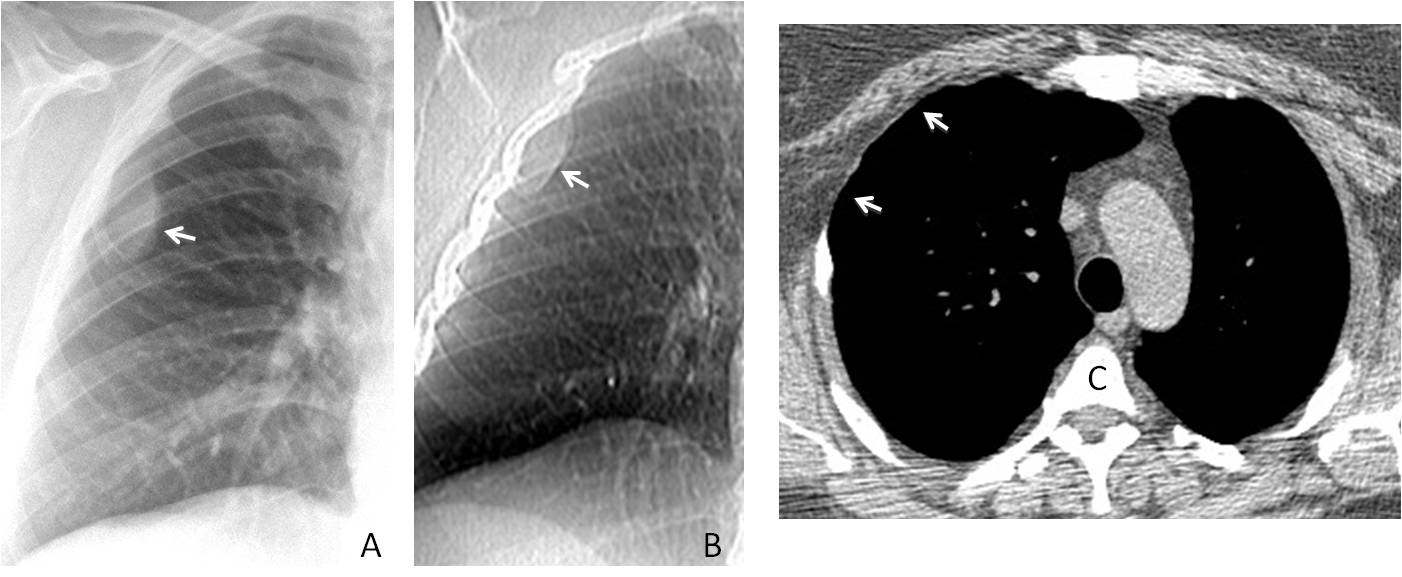
Fig. 4
Fig. 4. Repeat radiograph after CT again shows the extrapulmonary lesion (A, arrow). The CT scout view demonstrates the lesion (B, arrow), but it is not visible in the axial view (C). However, in the same view, marked atrophy of the intercostal muscle is seen (C, arrows).
Considering the atrophic intercostal muscles, a good explanation for the findings is that chest wall fat was intermittently herniating into the chest cavity. This theory was proven by placing the patient in the left decubitus position, which confirmed the fat herniation (Fig. 5). The patient had undergone surgery in this area during childhood to treat complications of a pneumothorax.
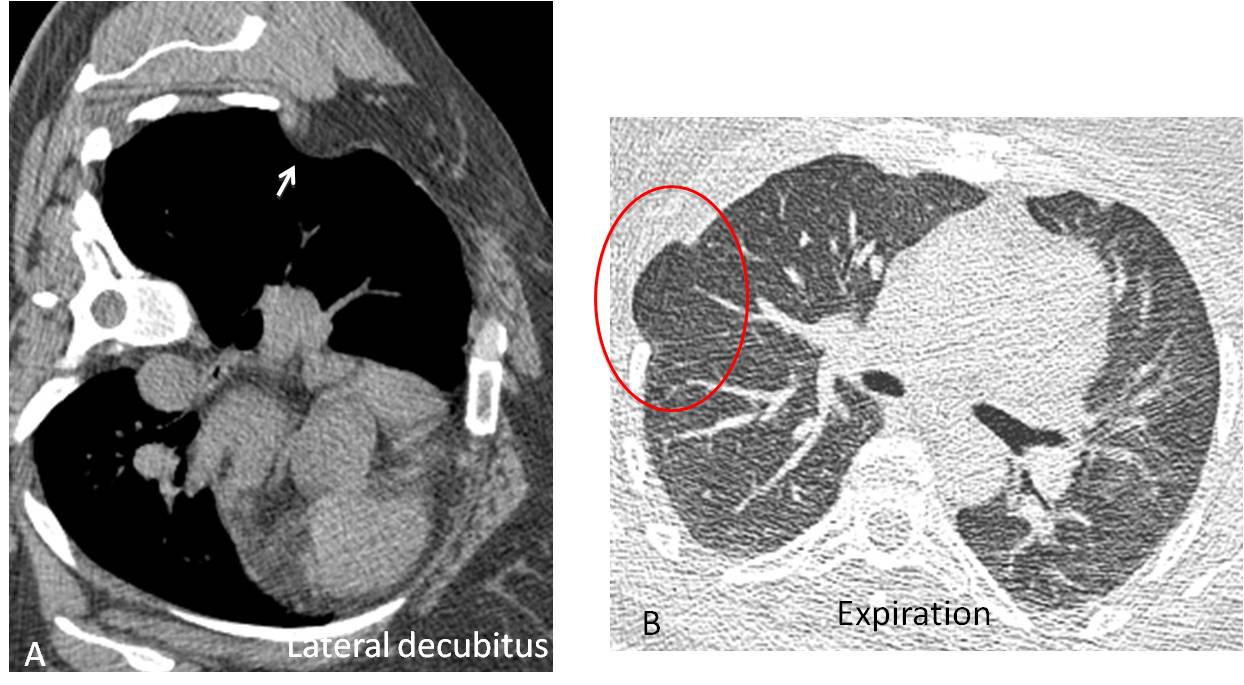
Fig. 5
Fig. 5. With the patient in the lateral decubitus position, the extrapleural fat herniates into the lung (A, arrow). Expiratory CT showed lung herniation in the same weak spot (B, circle).
This is a nice example of how with imagination and persistence (the final CT was taken six months after the initial radiograph), we can explain apparently contradicting findings and arrive at a satisfactory diagnosis.

Dr. Pepe’s fifth commandment:
Thou shalt remember the components of the diagnostic formula:
D = (bc + lv + ps + chl) e
basic concepts, lateral view, previous studies, and checklists.
And particularly remember that they may all be useless without enhancement by the fifth element: enthusiasm.


LAM
Lymphangioleiomyomatosis (LAM). Would speculate that the retroperitoneal tumour could have been in the kidneys (Angiomyolipoma).
Tumor was in the retroperitoneum nad was a PEComa.
Young woman with multiple bilateral pulmonary cysts lesions, with diffuse and aleatory widespread. Lymphangioleiomiomatosis is a good option.
Thanks!!
LAM
LAM
LAM
in young woman LAM is best diagnosis eith retroperitoneal another lymphatic mass or renal angiomyolipoma
Istiocitosi X
Lymphangioleiomiomatosis VS lymphoid intersticial pneunomia
Birt-Hogg-Dubé
Birt-Hogg-dube
Primary pattern of cyst (air image without inner vessel) with Round regular shape disseminated throughout both lungs. No nodule, no fibrosing pattern.
Young woman
Lymphyngioleiomyomatosis. Most likely renal tumors such as angiomyolipomas.
If bilateral angiomyolipomas, consider syndromic tuberous sclerosis.
LAM
Birt-Hogg-Dubé
LAM
I made a comment about the histology of the tumor and nobody paid any attention
Perivascular epitheloid cells tumors (PEComa) are a group of tumours that include angiomyolipomas, lymphangioleiomiomatosis, sugar cell tumors… and is in association with sclerosis tuberous
Lymphangioleiomiomatosis
LAM
Since lymphangioleiomyomatosis, an otherwise benign condition, belongs to the family of perivascular epitheloid cell tumours, it cannot be excluded that the lung lesions in this case in fact represent metastases from the retroperitoneal perivascular epitheloid cell tumour rather than independent neoplasms.
J Med Case Reports. 2009; 3: 62.
Good thinking,but it is not the case. CT was stable for more than two years. But I like your idea!
PECOMA E LAM appartengono alla stessa categoria di tumori mesenchimali…..quindi pecoma retroperitoneale e lam polmonare….
LAM
At this stage of the game I imagine that everybody knows that the patient has LAM associated to a PEComa. Congratulations to all of you who gave the right answer, lead by Murzin, who was the first.
Have a nice summer vacation!
Sorry to be the one to complain, but the article repeated lesson chapter 4, about the checklists. I suspect it was accidental. can you please put chapter 5, which represents letter ‘e’ in formula D = (bc + lv + ps + chl) e.
You’re right, it was accidental. We’re sorry about ths mistake. The real solution is now in place!
Dr. Pepe – probably the best mathematician between radiologist:)
Great thanks for sharing Your knowledge and enthusiasm with others.
Have a nice holiday!
Thank you very much, my friend. I am touched by your comment.
where is the professor?
Sorry, I was on vacation.
Next case will be posted on Monday, September 4.
Glad to be missed!
both lung cystic lesion
Lymphangioleiomiomatosis is a good option.