Dr. Pepe’s Diploma Casebook: Case 115 – SOLVED!
Dear Friends,
Today I am presenting radiographs of a 60-year-old man with a cough and moderate fever.
Diagnosis:
1. Viral pneumonia
2. Non-cardiac pulmonary edema
3. Pulmonary hemorrhage
4. None of the above
Check the images below, leave your thoughts in the comments section, and come back on Friday for the answer.
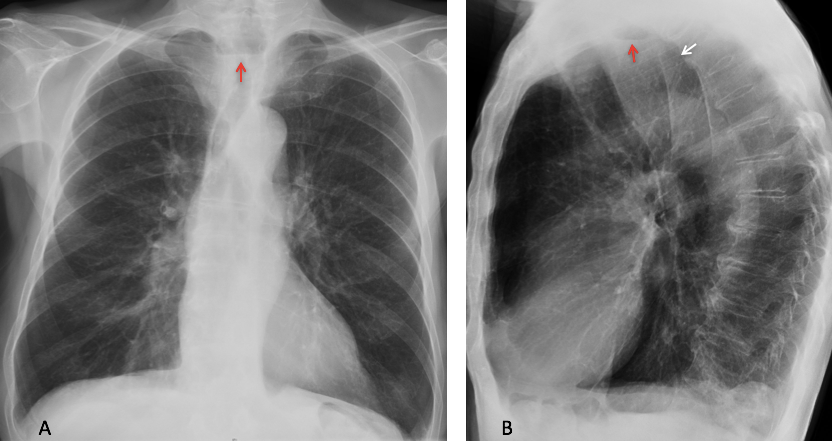
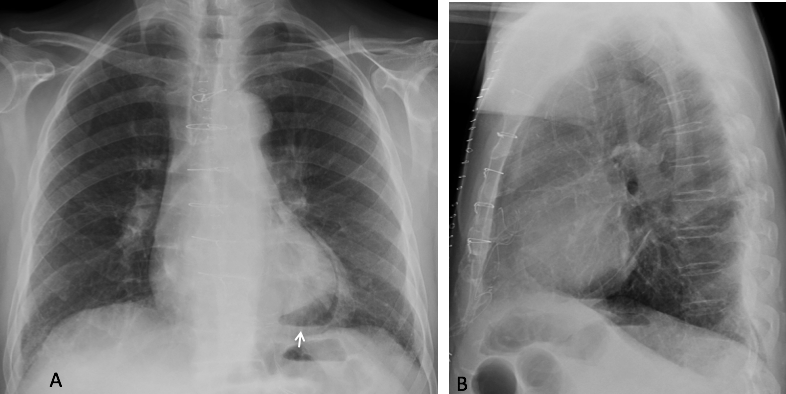
Findings: Chest radiographs shows bilateral airspace infiltrates. There is also dilatation of the upper esophagus in the PA view (A, white arrows) with an air-fluid level (A, red arrow). The lateral view shows a retrocardiac mass (B, white arrow), suggestive of a dilated lower esophagus. The trachea is displaced forward (B, red arrow).
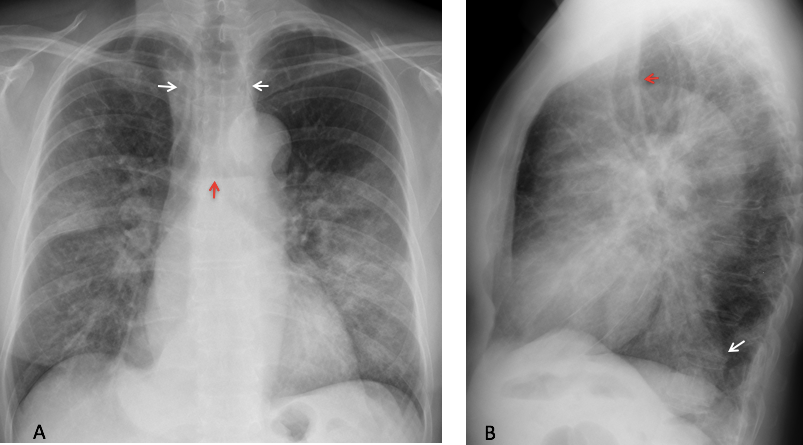
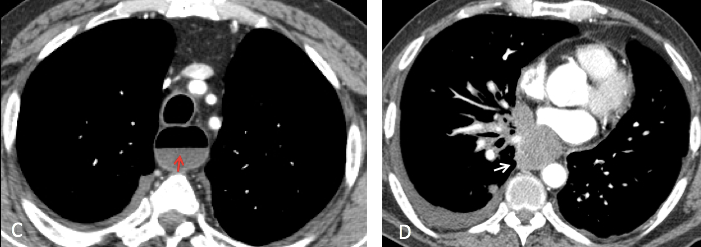
Coronal CT shows a dilated esophagus (C, arrow) and the air-space disease. Axial CT images confirm dilatation of the esophagus, which is full of residue (D and E, arrows).
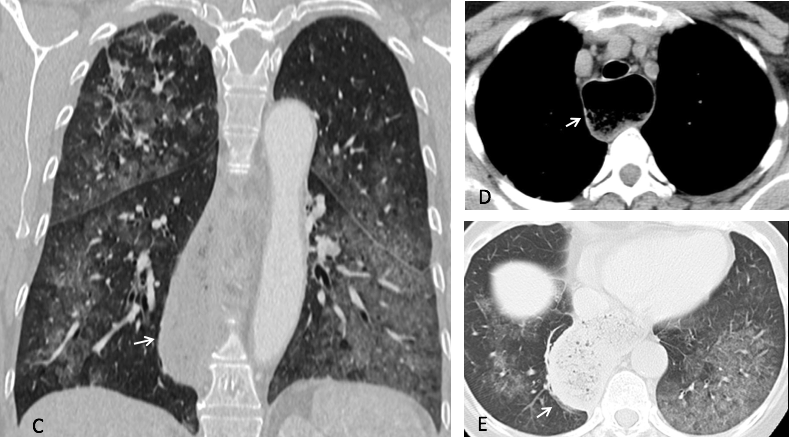
Final diagnosis: esophageal achalasia with secondary aspiration pneumonia
In case 114, I described air-fluid levels in lung and pleura. In this presentation I intend to discuss the appearance and differential diagnosis of air-fluid levels in the mediastinum, chest wall, and subdiaphragmatic area.
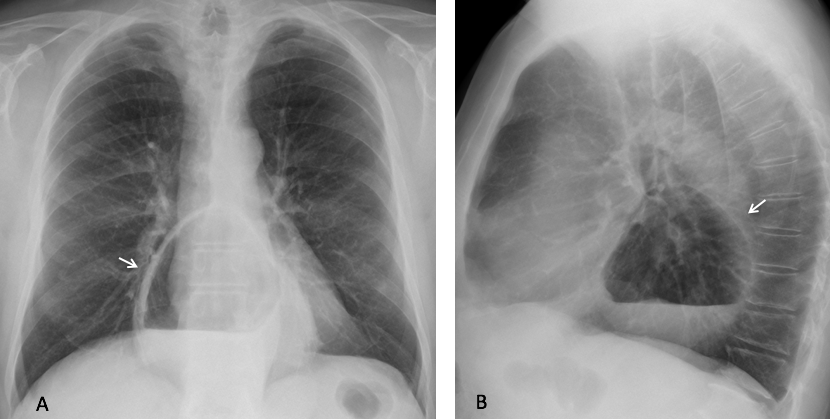
By far, hiatal hernia is the most frequent cause of air-fluid level in the middle lower mediastinum. It has a typical appearance (Fig. 1) and is very common in the elderly.
Fig. 1. 72-year-old. woman with a large hiatal hernia with an air-fluid level in the lower middle mediastinum (A and B, arrows).
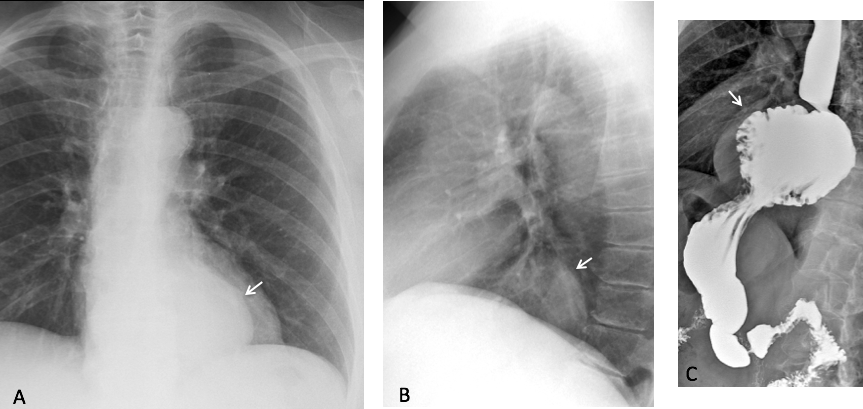
A small percentage of hiatal hernias do not have air, raising the possibility of a solid mediastinal mass. The uncertainty is easily clarified by performing an esophagogram (Fig. 2). Remember that any mass in the lower middle mediastinum is a hiatal hernia until proven otherwise.
Fig. 2. Rounded retrocardiac mass (A, arrow), located in the lower middle mediastinum in the lateral view (B, arrow). Esophagogram demonstrates an airless hiatal hernia (C, arrow).
Excluding hiatal hernia, an air-fluid level in the mediastinum is usually located in the esophagus. It is seen as a straight line in the middle mediastinum. It is usually related to esophageal obstruction of any cause, the most common being achalasia (Figs. 3 and 4) and neoplasm (Fig. 5). Occasionally, a diverticulum may show an air-fluid level (Fig. 6).
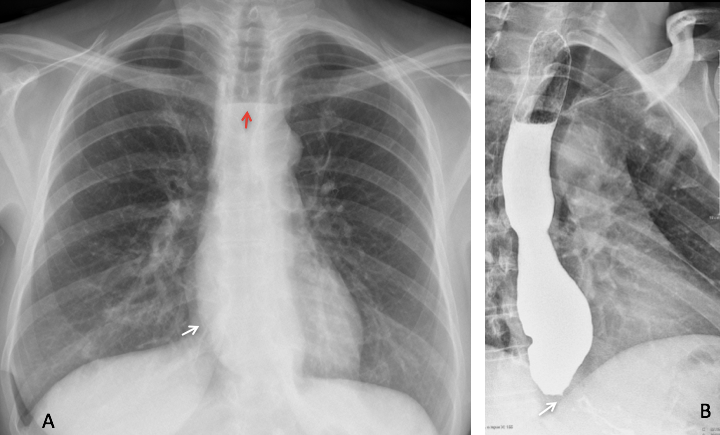
Fig. 3. 47-year-old woman with dysphagia. PA radiograph shows bulging of the paraesophageal line (A, white arrow) with a mediastinal air-fluid level (A, red arrow). Esophagogram shows distal esophageal stenosis (B, arrow) with dilatation and air-fluid level. Diagnosis: achalasia
Fig. 4. 47 year-old man with dysphagia. PA radiograph shows a dilated lower esophagus (A, white arrows). In the lateral view, an air-fluid level is seen in mid-esophagus B, white arrow) and there is thickening of the retrosternal stripe (B, red arrow). CT confirms the dilated esophagus, containing air and fluid (C, arrow). Diagnosis: esophageal achalasia
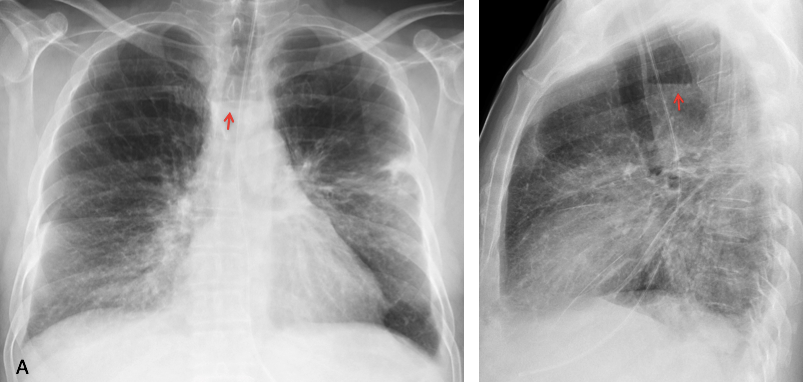
Fig. 5. 52-year-old man with diffuse lung disease and an air-fluid level in the upper mediastinum (A and B, arrows).
Enhanced axial CT shows dilatation of the upper esophagus with an air-fluid level (C, arrow). A caudal CT slice shows a middle mediastinal mass (D, arrow). Diagnosis: small-cell lung carcinoma infiltrating the middle third of the esophagus.
Fig. 6. 62-year-old man with trouble swallowing. PA radiograph shows an upper mediastinal air-fluid level (A, arrow). Lateral view shows an opacity occupying Raider’s triangle (B, white arrow) with an air-fluid level (B, red arrow). Esophagogram showed a Zenker diverticulum, confirmed at surgery.
Last, but not least, do not forget to investigate previous esophageal surgery as a cause of mediastinal air-fluid levels.
Fig. 7. Patient after resection of the lower esophagus and pulling-up of the stomach (C, arrow), giving the air fluid levels apparent on chest radiographs (A and B, arrows).
Pneumopericardium is very uncommon and usually related to previous surgery (Fig. 8). If there is no history of a previous intervention, think of a large hiatal hernia mimicking pericardial air (Fig. 9).
Fig. 8. 47-year-old man with pneumopericardium and an air-fluid level after heart surgery visible in the PA view (A, arrow).
Fig. 9. 84-year-old man with metastatic lung disease and a large hiatal hernia simulating pneumopericardium in the supine radiograph (A, arrows). Enhanced coronal CT confirms the massive hernia (B, arrows).
Subdiaphragmatic air-fluid levels are better seen in the RUQ. They are usually secondary to subphrenic or liver abscesses (Fig. 10). Occasionally, dilated bowel loops may simulate an abscess, easily excluded with barium studies or CT scan (Fig. 11).
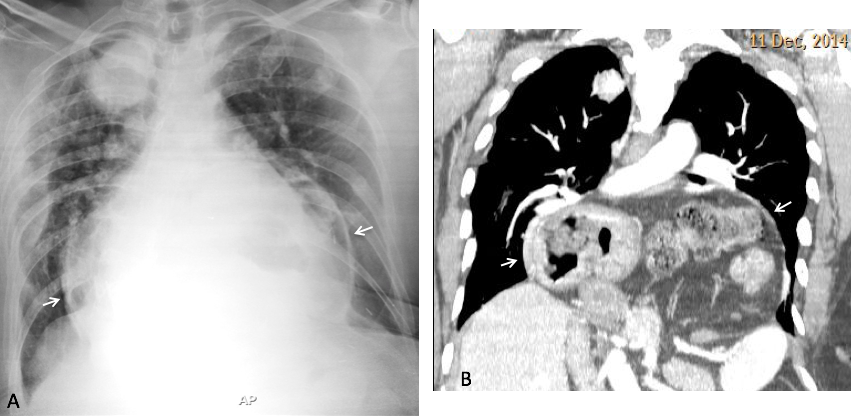
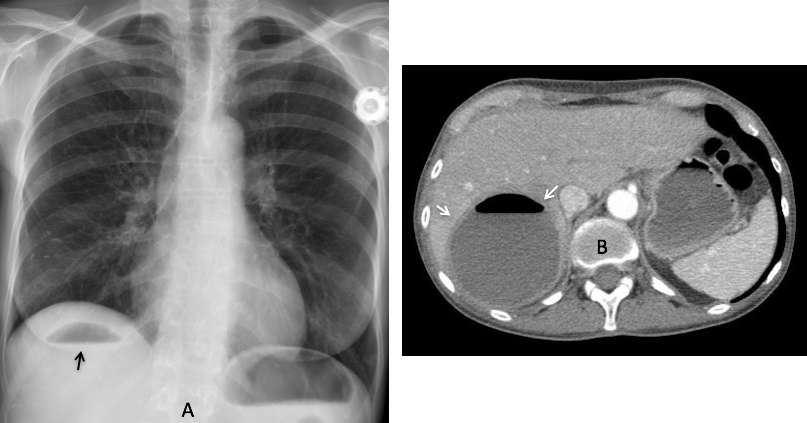
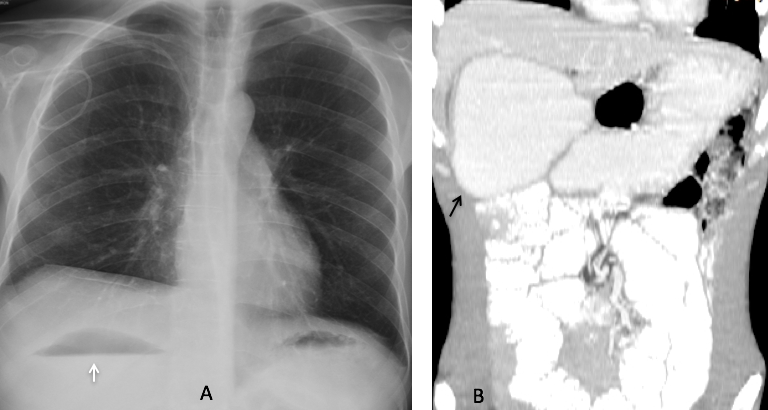
Fig. 10. 47 year-old woman with carcinoma of the breast and a liver abscess seen as an air-fluid level in the RUQ of the abdomen (A, arrow). Enhanced axial CT confirms the intrahepatic location of the abscess (B, arrows) (Case courtesy of Dr. Matthias Meissnitzer).
Fig. 11. 34 year-old man with severe intestinal malabsorption syndrome. An air-fluid level in the dilated duodenum simulates an intrahepatic abscess (A, arrow). The dilated duodenum is obvious in the coronal CT image (B, arrow).
Air-fluid level in the thoracic tissues is usually secondary to previous surgery. The appearance is similar to air in the pleura, lacking an upper wall and with asymmetrical length of the levels (Fig. 12).
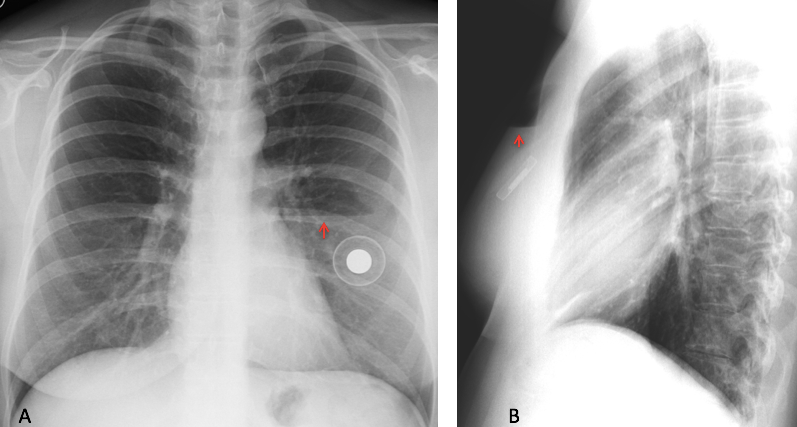
Fig. 12. Air-fluid level in the PA radiograph after placement of a breast implant (A, arrow).
Lateral view confirms the location in the anterior chest wall (B, arrow). Note the asymmetry in length of the levels in the two views.
Follow Dr. Pepe’s advice:
1. Most common cause of air-fluid level in the lower middle mediastinum is hiatal hernia.
2. Most air-fluid levels in the mediastinum are due to esophageal obstruction.
3. Subdiaphragmatic air-fluid levels are due to abdominal abscess or dilated bowel loops.

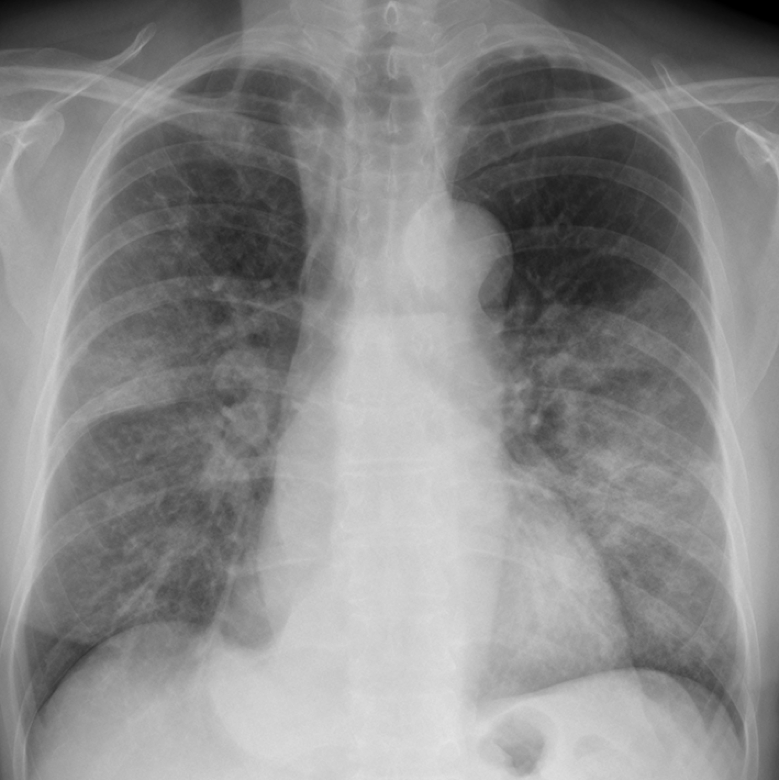
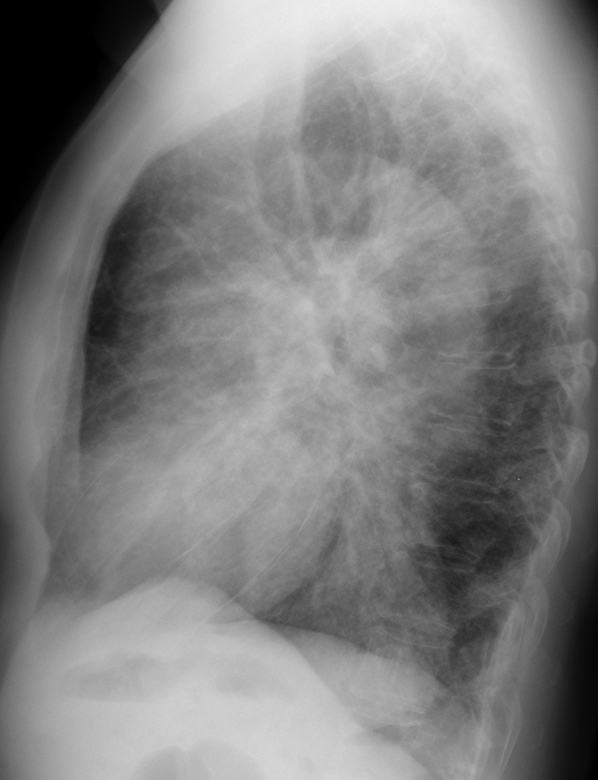





Good morning. There are billateral reticulonodular opacities located in the lower two thirds of both lungs. I can also see a small triangular opacity at the region of the right cardiophrenic angle. I think there could also be thickening of the right paratracheal line, with apparent occupation of the anterior clear space. Maybe the answer is number 4: lymphangitic carcinomatosis.
Hello!
Superior esophageal dilatation (in lateral view there is anterior tracheal displacement). Bilateral alveolar opacities in inferiors hemithorax, so I think in aspirative pneumonie.
There is an increased density in the right cardiophrenic angle and obliteration of the retrocardiac space.
So 4. Any of the above: Aspirative pneumonie because of esophaeal pathology
There are reticulonodular and patchy opacity in bilateral mid and lower lung zones, could be due to infection, inflammation or malignancy
There is proximal esophageal dilatation with air fluid level, suspected esophageal lesion.
There is soft tissue opacity at right cardiophrenic angle with bulging contour, possibly mass lesion or enlarged nodes.
There is suspected LA enlargement.
The answer: No 4. None of above
I see an air fluid level in the esophagus with bilateral pulmonary infiltrates in mid and lower lung zones most likely due to aspiration pneumonia. Irregular opacity in the right cardiophrenic angle – would consider an esophageal diverticulum and achalasia as a cause of the esophageal air fluid level.
Double density sign of the right heart border on PA and bulging of the posterior aspect of the cardiac silhouette on lateral suggests left atrial enlargement.
answer: 4 none of the above
Double contour of right heart border can also be due to dilated distal esophagus and is more probable in this case.
Wise decision ,-)
there are peribronchovascular changes, multiple ill-defined nodules in both lung, predominantly in upper lobes and the infiltration in the RUL on the level of IIId intercostal space – IVth rib
there is hyperlucency in the upper mediastinum and opacity in the posteriobasal origin – most likely corresponding to widened esophagus
4. none of above, DDX :
– esophageal tumor (GIST) with suprastenotic esophageal widening and aspiration pneumonia
– the esophageal diverticulum with further aspiration pneumonia
– postoperative condition (surgically treated achalasia oesophagogastroplasty?) and aspiration pneumonia
Or this I should write first:
– pseudoachalasia – barium is needed to check for bird beak sign
(This is the most suggesting diagnose)
A most complete differential diagnosis. Congratulations
Thursaday evening recap: achalasia with chronic aspiration. The key to the diagnosis is recognizing the dilated esophagus with an air-fluid level.
Gold medal to MK, who was the first to mention the diagnosis