Dr. Pepe’s Diploma Casebook: Case 43 – SOLVED!
Dear Friends,
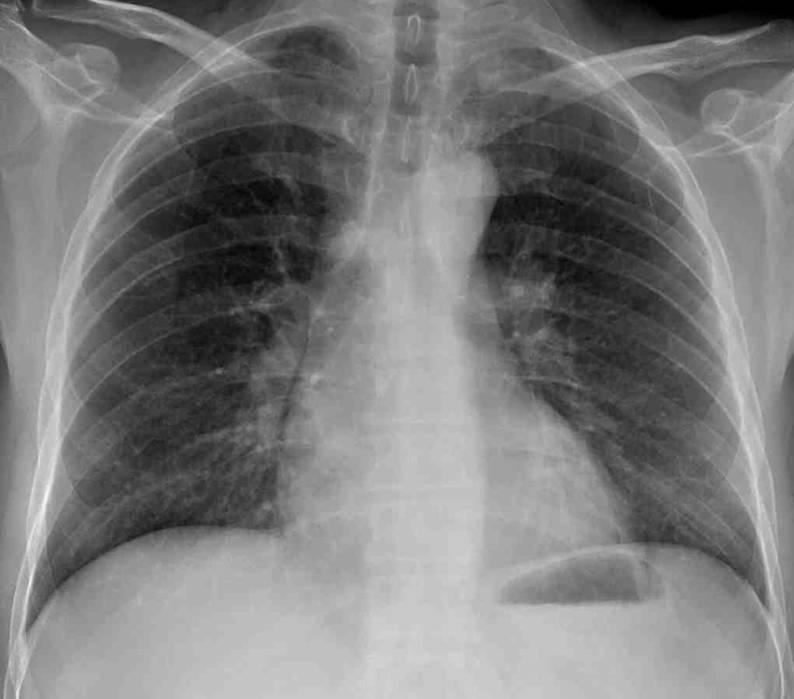
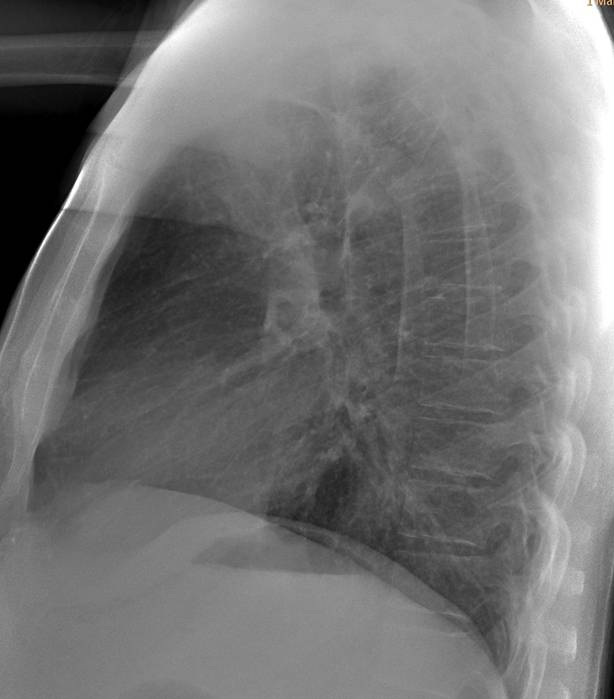
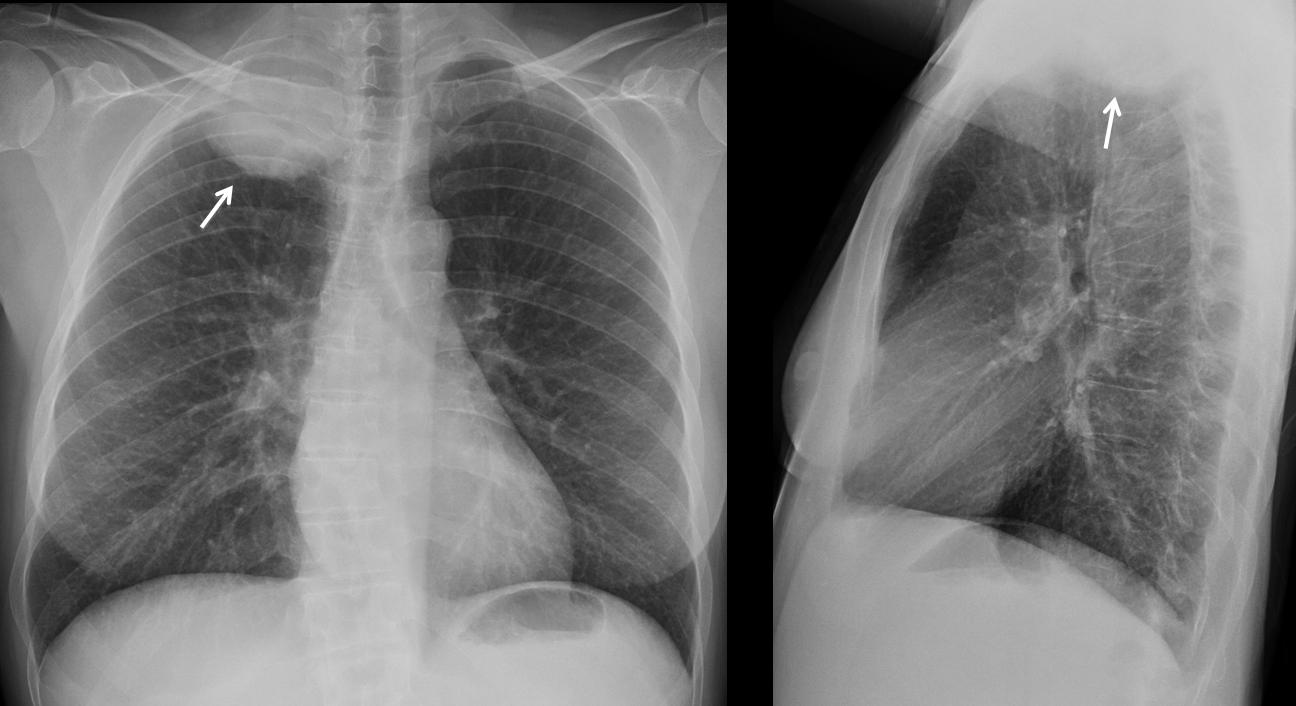
Today I’m presenting radiographs of a 54-year-old male with chest pain (below).
Would you call these radiographs normal?
If not, where is the abnormality?
Leave me your answers in the comments section and look out for the answer on Friday.
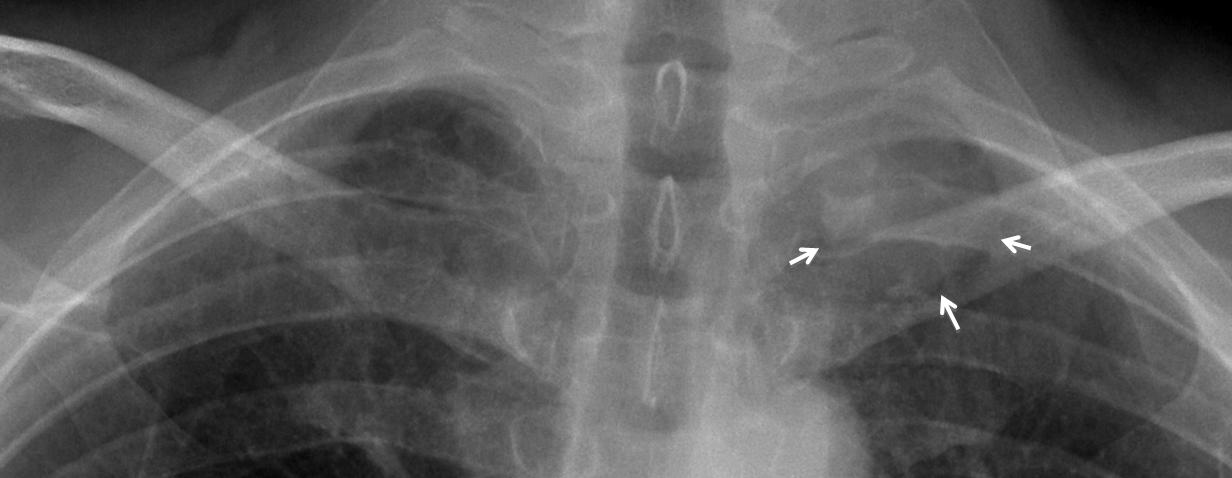
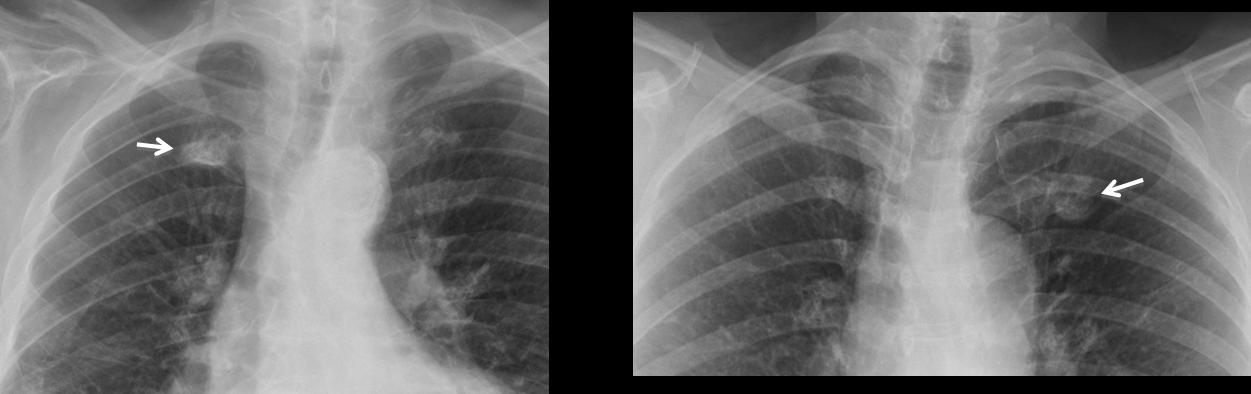
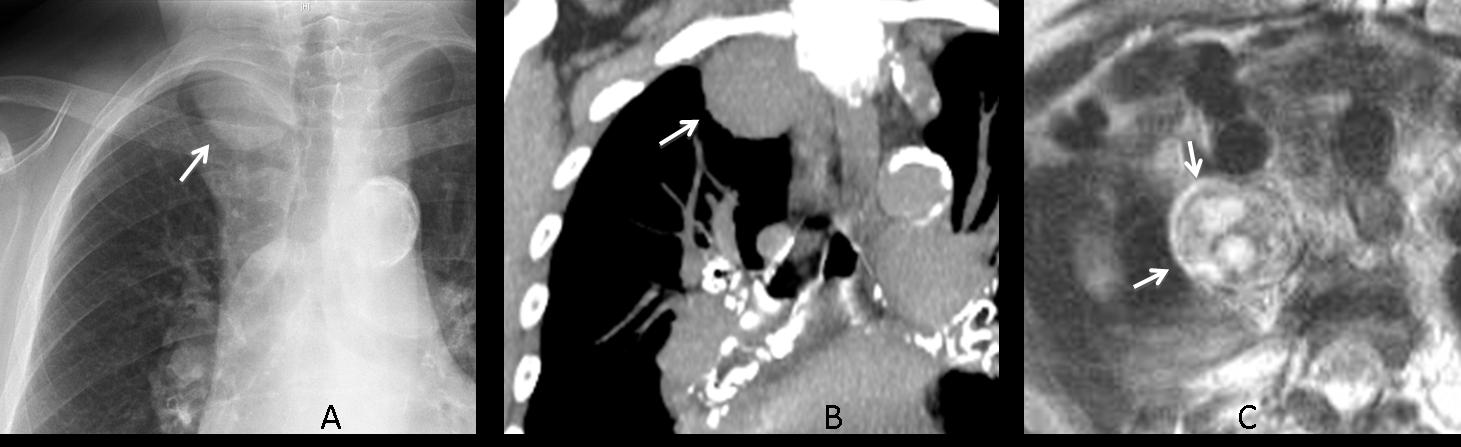
Findings: In the PA view, there is round mass in the left apex (arrows), partially obscured by the overlying bone structures. The mass was missed, and the chest radiograph was reported as normal.
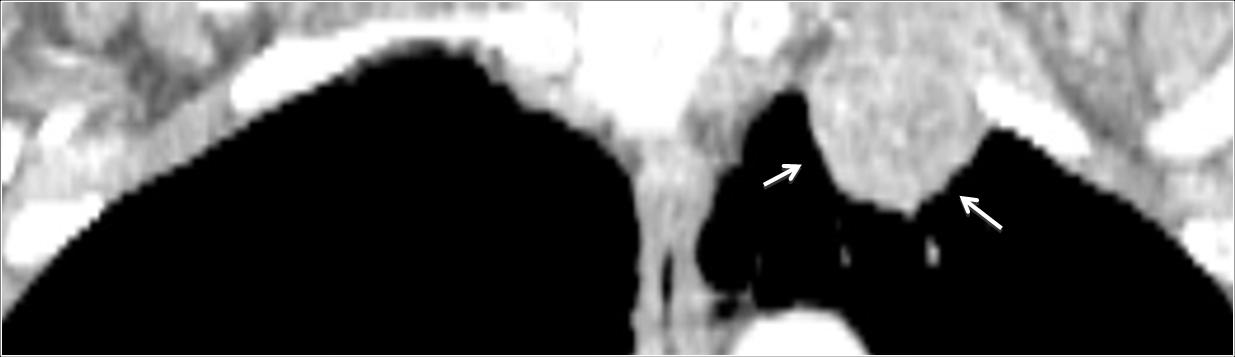
CT, performed to investigate myasthenia, shows the mass in the left apex (arrows). Needle biopsy returned the diagnosis of adenocarcinoma.
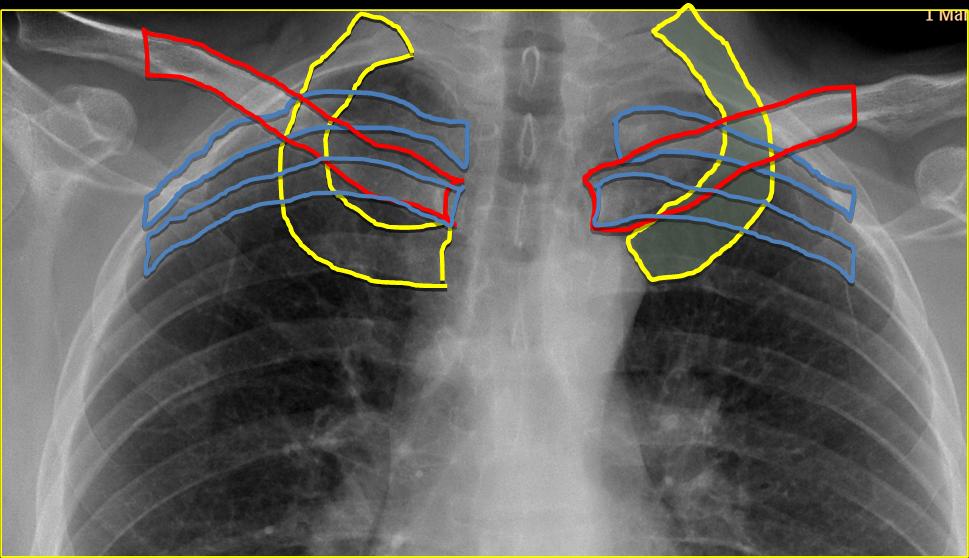
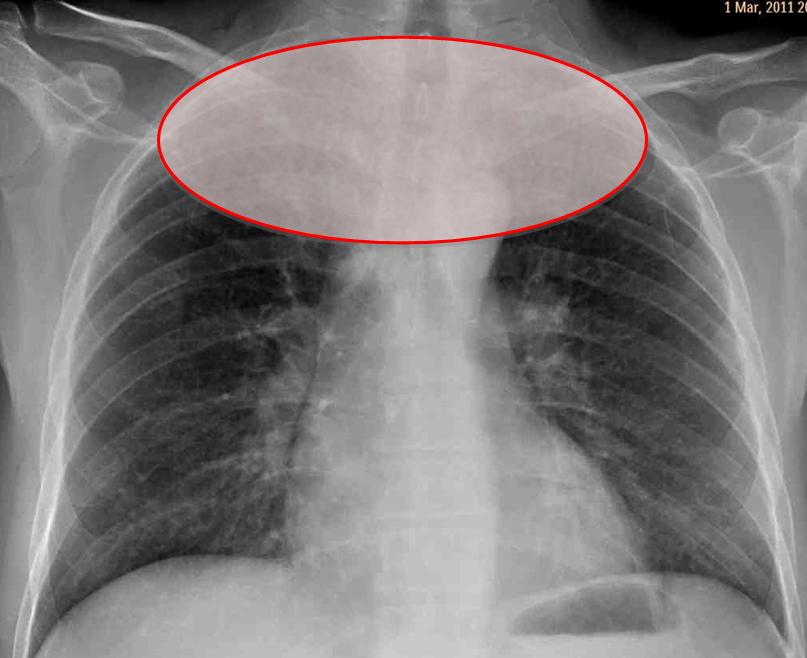
Missed lesions in the lung apices are not uncommon, because the numerous bone structures in this region (Fig. 3, below) obscure the lung parenchyma and impede visualisation of underlying disease. For this reason, the apices should be given special attention in the chest radiograph. Moreover, the apices are poorly visualised in the lateral view, leaving the PA view as the main source of information.
The upper apical area is limited by the first ribs. I have arbitrarily placed the lower limit at the superior cortex of the second ribs (Fig. 4, shaded area). Before the CT era, lordotic views were employed to better visualise the apices, but in my experience, the lordotic view can be confusing. Thus, if apical disease is suspected, CT is the technique of choice.
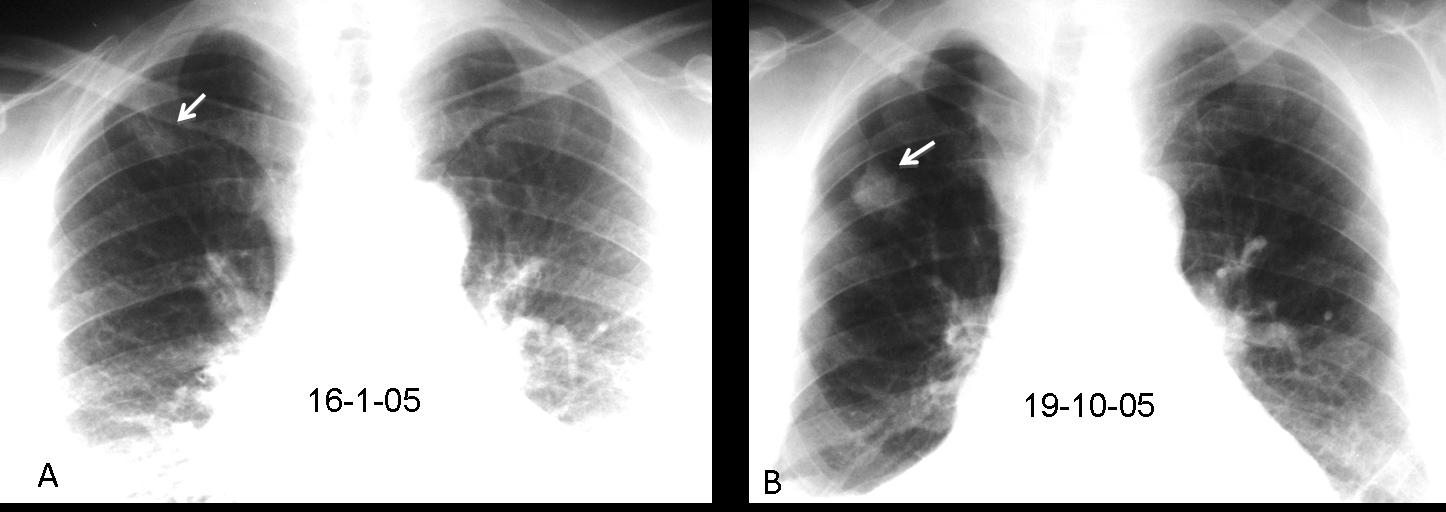
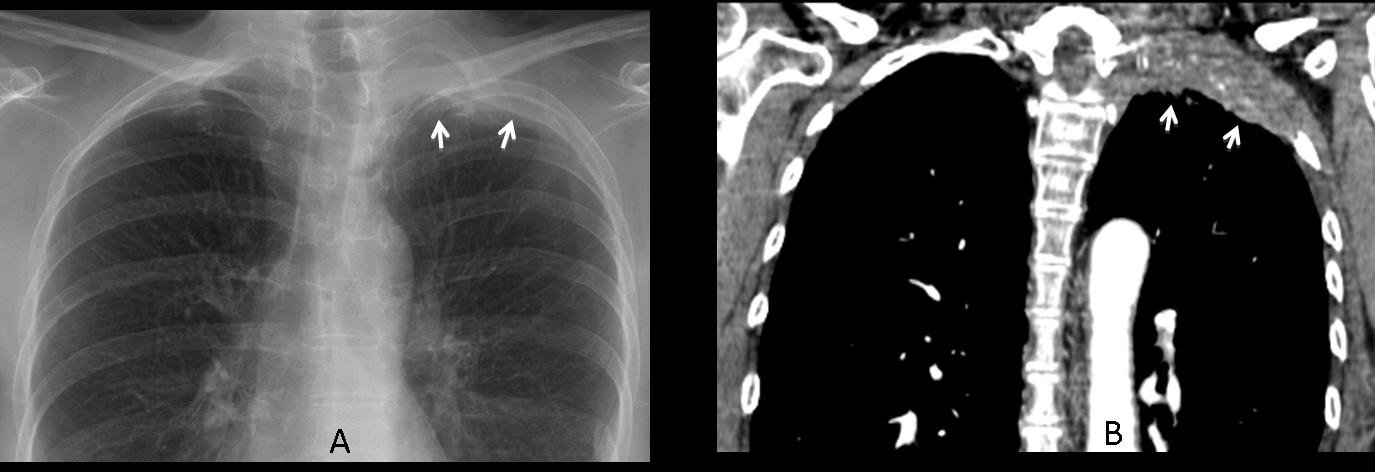
Pulmonary nodules are a common presentation of carcinoma, and most occur in the upper lobes. It should not come as a surprise that they are often missed in the initial chest radiograph. The reported miss rate reaches 60%. Below is a representative case: 59-year-old male with a right apical nodule that was not seen in January 2005 (A, arrow). The nodule was discovered nine months later when a postoperative pneumothorax made it obvious (B, arrow).
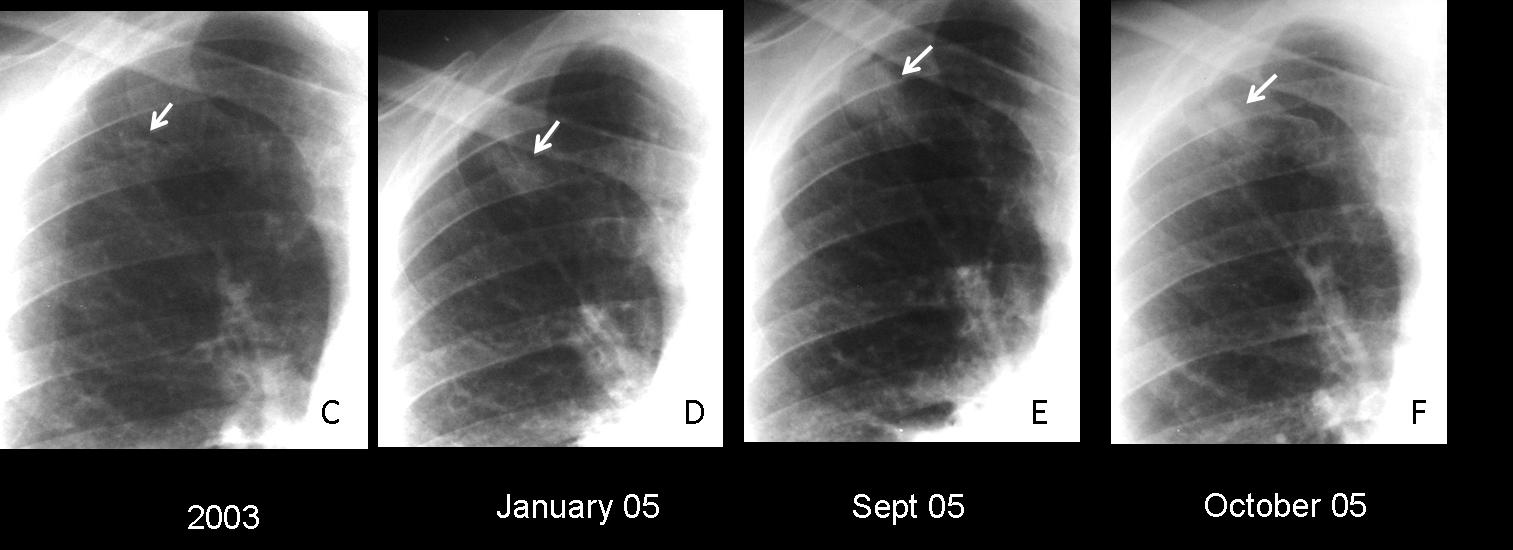
A series of films in the same patient shows that the nodule was missed repeatedly. It was probably present in 2003 (C, arrow), and was obvious in January 2005 (D, arrow), September 2005 (E, arrow), and early October 2005 (F, arrow). Final diagnosis: carcinoma.
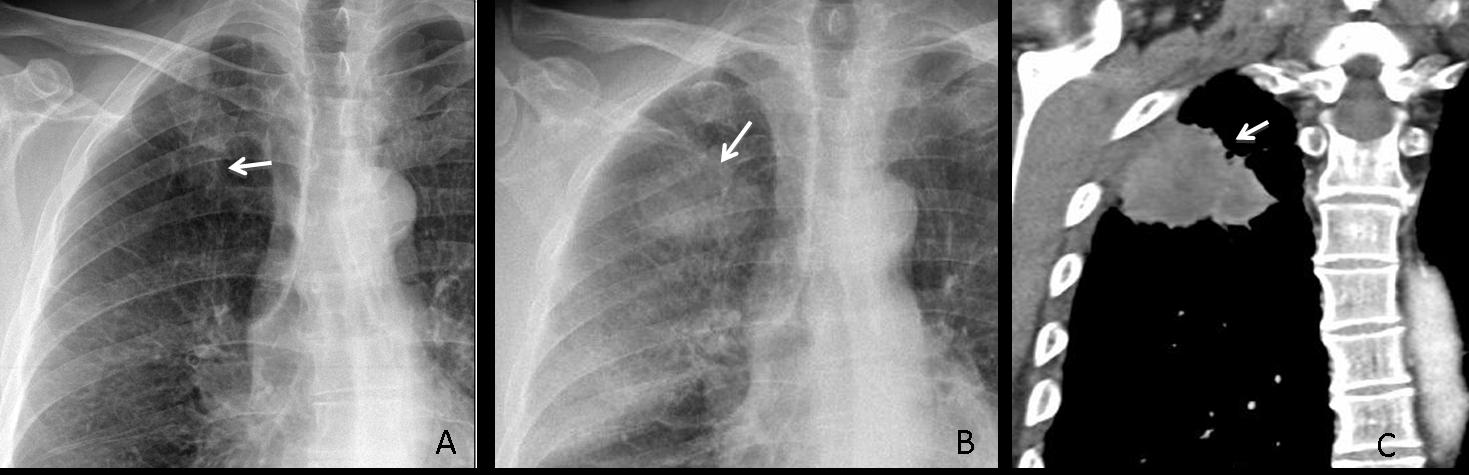
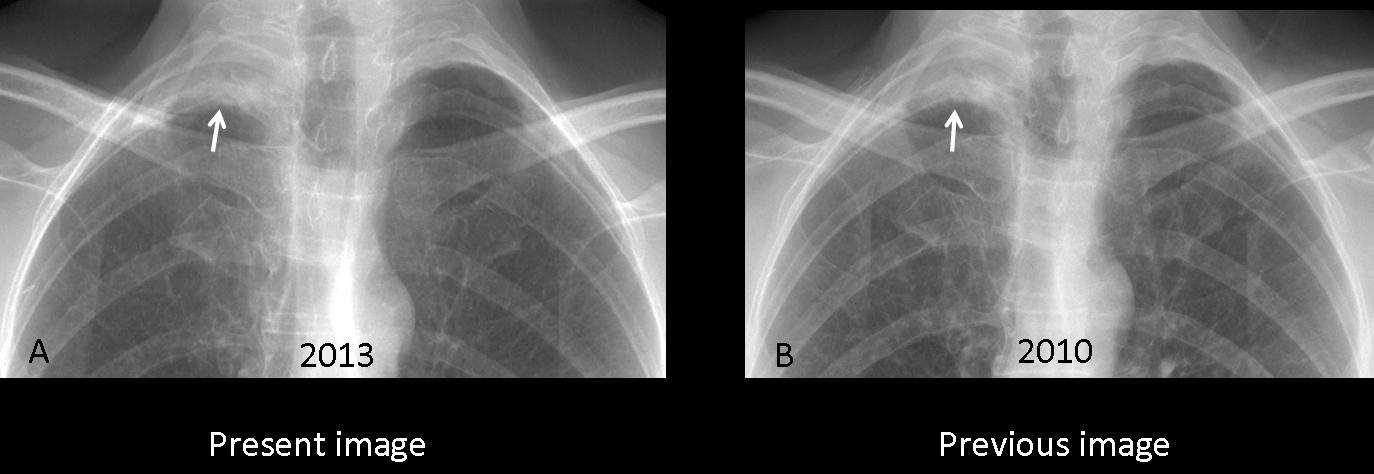
Missing a malignant nodule can have dire consequences. Below are images of a 63-year-old man, in whom a right apical nodule was not seen in 2009 (A, arrow). Radiographs made two years later show that the nodule has increased markedly in size (B, arrow). CT confirms the findings (C, arrow). Diagnosis: carcinoma with chest wall invasion.
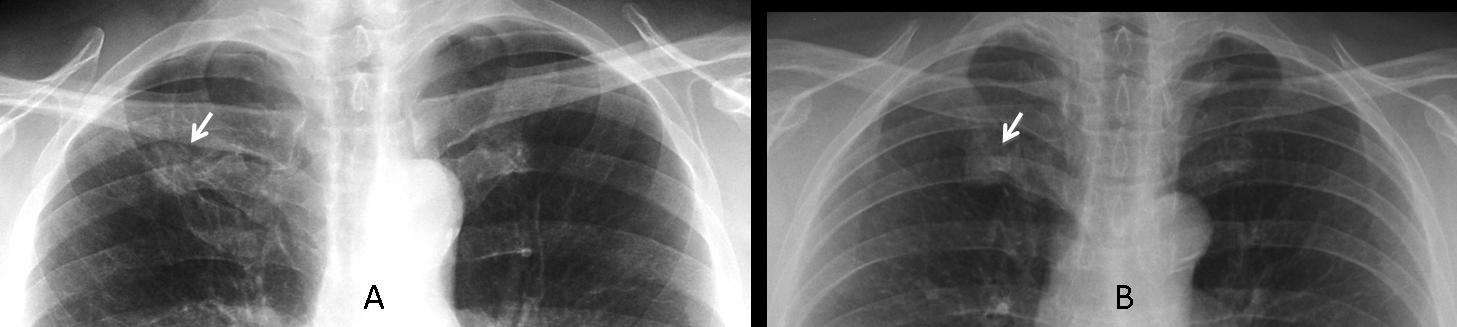
Nodules near the first chondrocostal cartilage should not be confused with exuberant ossification of the cartilage. Below are radiographs of two patients with nodular shadows in the apical area. Which one would you call a tumour and which one a normal variant?
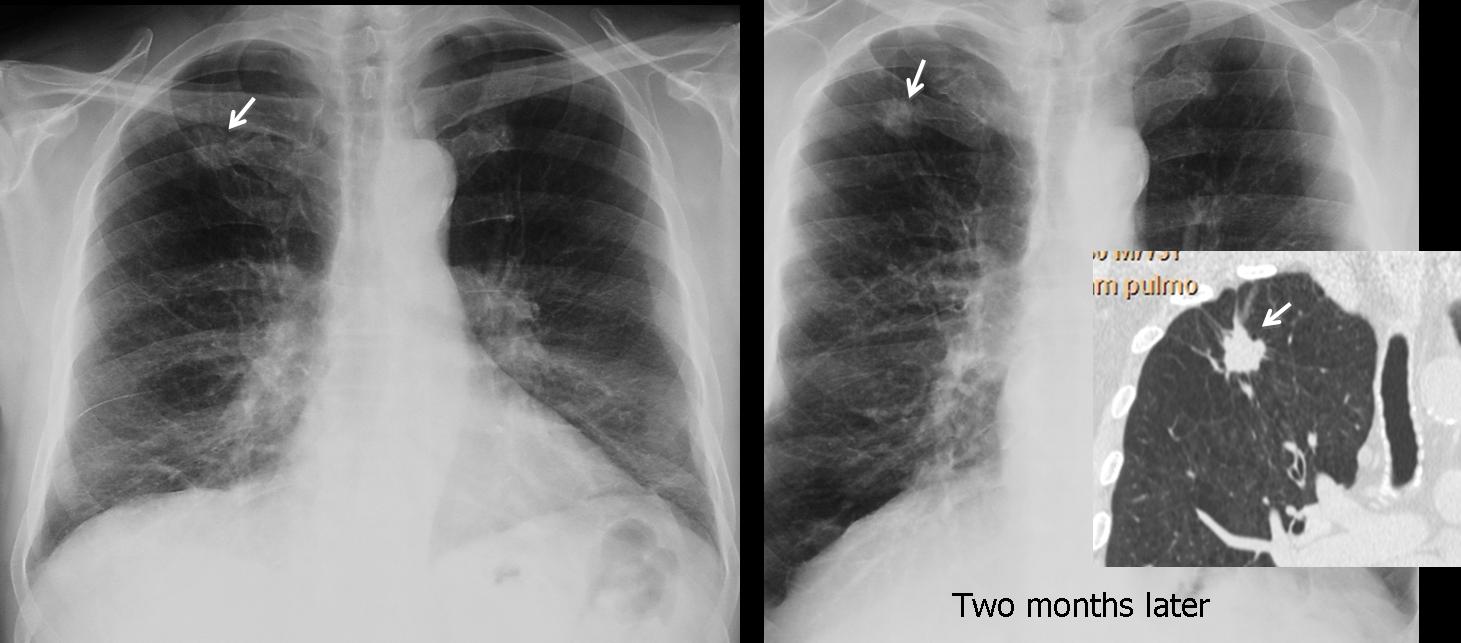
These radiographs correspond to case A, a 56-year-old male smoker. The nodule is real. It was overlooked initially and discovered in a second examination two months later when the patient took a deeper inspiration for the radiograph. CT (insert) confirms the findings. Diagnosis: adenocarcinoma.
Case B corresponds to a false nodule due to calcified hypertrophic cartilage at the first costochondral union. They are fairly common in elderly people and can be recognised by their increased opacity and proximity to the costochondral area.
Below are two more examples of costochondral cartilage simulating nodules (arrows).
The radiographs below belong to 49-year-old man with chest pain. Would you call them normal?
If not, where would you place the abnormality?
The PA radiograph shows asymmetric pleural thickening at the left apex (A, arrows). This finding, when combined with shoulder pain, should prompt additional examinations to exclude a superior sulcus tumour (Pancoast tumour). Coronal CT shows the tumour (B, arrows) invading the chest wall and encasing the left subclavian artery.
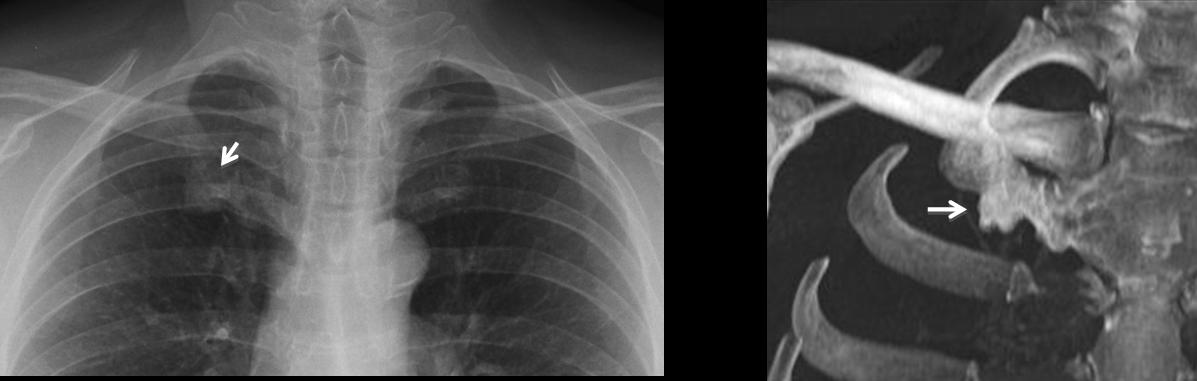
Pancoast tumour is characterised by the typical triad of shoulder pain, rib destruction and Horner syndrome. In many cases all three factors are not present, and the term superior sulcus tumour is preferred. The current criteria recommend that any patient with upper chest pain and asymmetrical apical pleural thickening greater than 5 mm should undergo further study. In my experience, rib destruction is difficult to identify on plain films, unless it is obvious, as in the case below, where there is marked pleural thickening and destruction of the second left rib (A,B, arrows). CT is the method of choice to evaluate bone invasion, and MRI is better for demonstrating brachial plexus involvement.
Since inflammatory/ischaemic apical pleural thickening (apical cap) is a common occurrence, how should we proceed in individual cases? When in doubt, comparison with previous films is of tremendous help by demonstrating that the thickening was present previously and unchanged, ruling out a neoplastic origin.
See the case below in which an apical cap remains stable for three years (A, B, arrows).
If no previous films are available, CT is decisive in differentiating an apical cap from a superior sulcus tumour. In the case of tumour, CT demonstrates a soft-tissue mass in the apical area, whereas in apical cap, there is extrapleural fat expansion and a mainly fat density lesion.
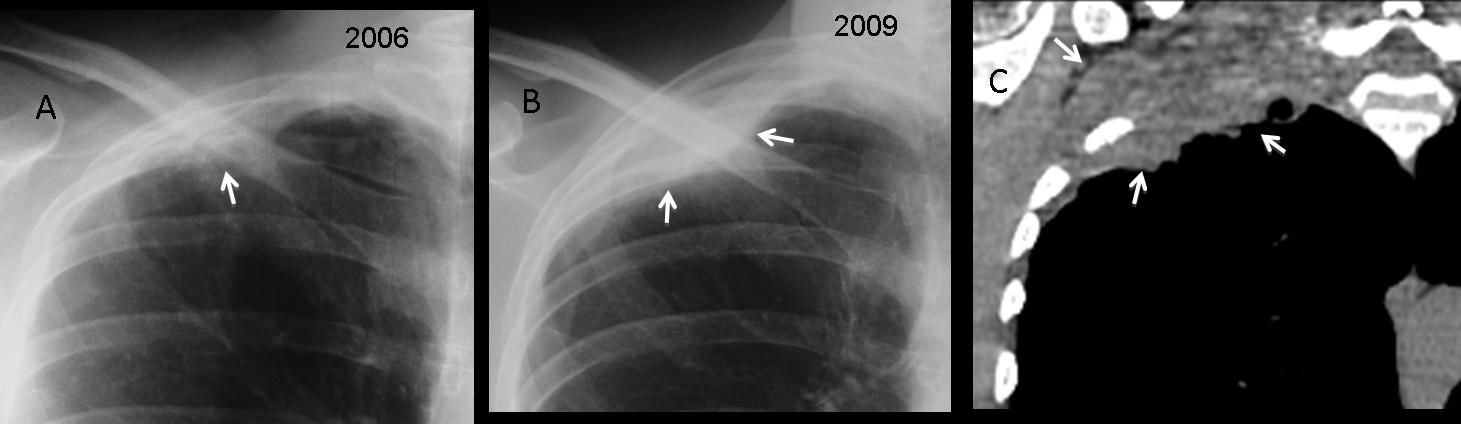
In the case below, there was discrete pleural thickening in 2006 (A, arrow) that was not considered significant. Three years later, the pleural thickening has increased markedly (B, arrow). CT shows an apical soft tissue mass with chest wall invasion (C, arrows), confirming the diagnosis of superior sulcus tumour.
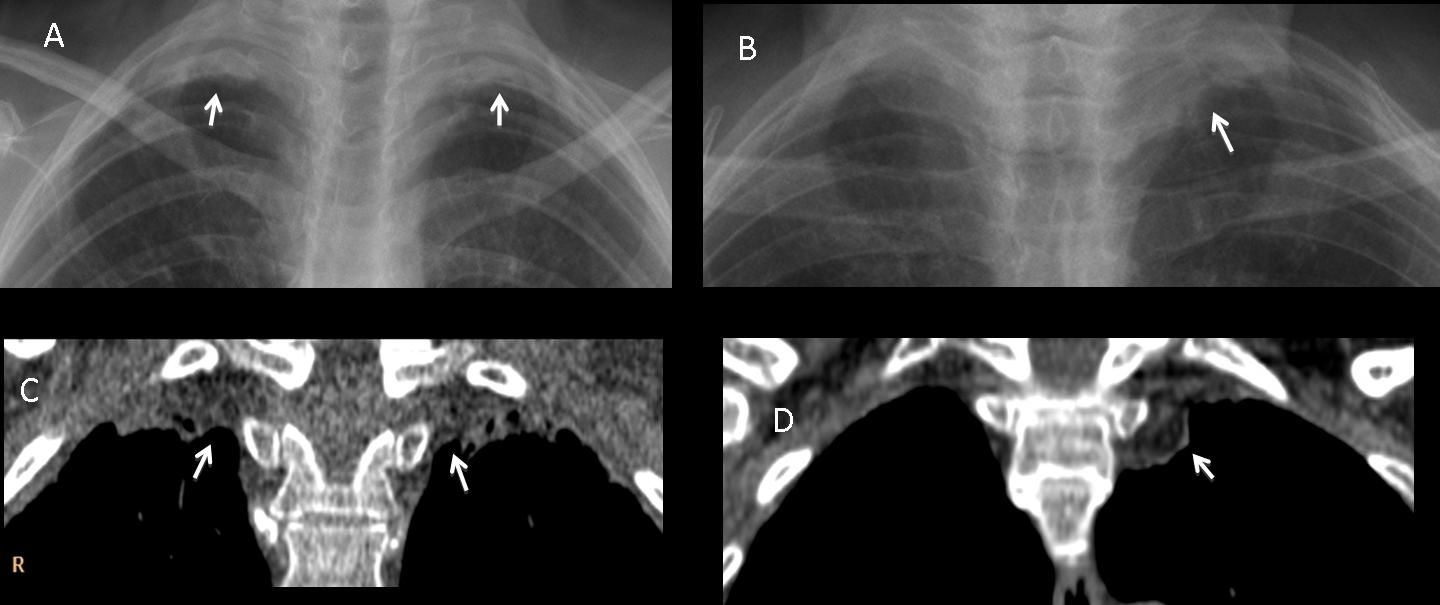
Inflammatory/ischaemic apical caps may be unilateral or bilateral (A,B arrows). In the cases below, CT shows the typical appearance of fat mixed with vessels and extrapleural tissue (C,D, arrows).
Some masses in the apices are easily seen, as in the images below. In these cases, it is important to determine where the mass originates to make an accurate differential diagnosis. Would you care to guess the origin of this lesion?
- Lung
- Mediastinum
- Pleura
- Can’t tell
The superior apical region is narrow, and large masses adapt to the available space, obscuring the characteristics that enable differentiation between intra- and extrapulmonary lesions. I find that it is complicated to determine the origin of a mass in chest plain films. CT or MRI must be performed to solve the problem. In this case, MRI shows that it is a lung carcinoma with chest wall invasion (A-C, arrows).
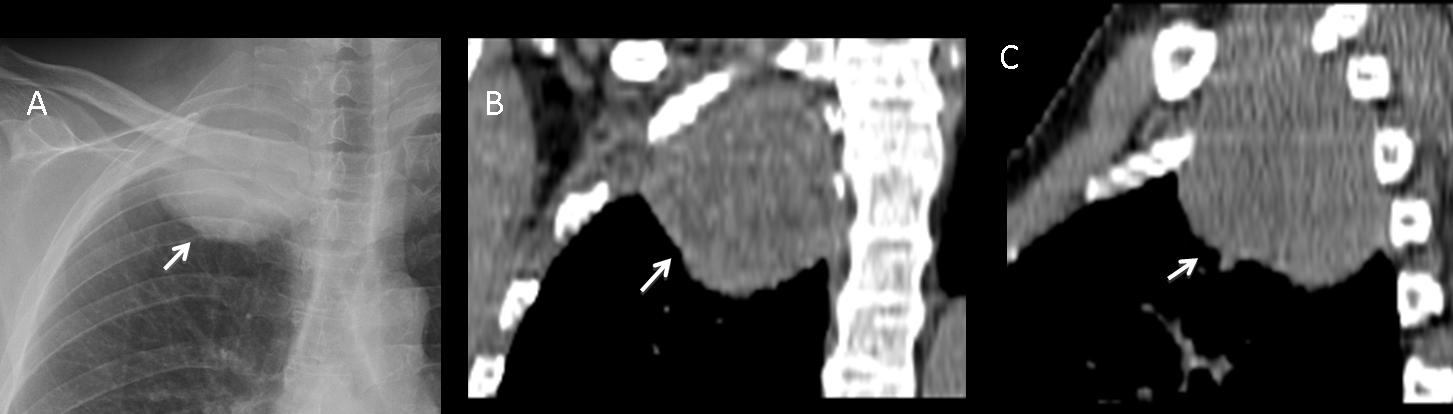
To illustrate the difficulty of determining the origin of an apical mass, I’m showing the following case of a 56-year-old woman with a rounded apical shadow. Chest radiograph and CT show features similar to those of the previous case (A,B arrows). MRI depicts the mass arising from the mediastinum (C, arrows). Final diagnosis: schwannoma.
Follow Dr. Pepe’s advice:
- The pulmonary apices are difficult to evaluate because of the overlying bone structures. About 60% of all missed pulmonary nodules are located in the apical region.
- To distinguish benign apical pleural thickening (apical cap) from a superior sulcus tumour, compare with previous films. If they are not available and the patient has symptoms, perform CT.
- It is very difficult to identify the origin of apical masses on plain films.





sarcoidosis
Donught sign
Tricky case Dr Pepe !!! The resolution of the Xrays doesn’t help much.
Nevertheless, I think that in the AP view there is an opacity projecting in the apex of the left lung and also destruction and sclerosis of the posterior end of the 3rd left rib.
No abnormalities in the profil view.
Pancoast tumor? Posterior thoracic wall tumor?
I am tricky, but just! I agree with your comment about the resolution. Will send you the original images.
There is no destruction or sclerosis of the third rib.
In PA view :There is an opacity at the right side of the carina I the lateral view :it is projecting anterior to the air filled airway ,and showing thick walled cavity that was not apparent in PA view .(DD:bronchogenic cyst_)
Pneumomediastinum
I also think that there is a small lesion in the apex of the left lung, though I do not think that it is the cause of pain. As always, cant wait till Friday 🙂
Patience, my son, patience.
i think professor gives as the answer.
is a phantom tumor.
accessory rib?
I agree with Katerina, i think that there is a lesion in the apex of the left lung. Neurinoma? Pancoast tumor?
molto tenue opacità rotodeggiante a limiti netti all’apice del polmone sx, che in LL non si riesce bene a definire.
Left upper nodular mass, lateral ,medial and inferior borders can be defined, it seens they are kindy irregular, but superior marging are barely visible. Could correspond with san intrapulmonary nodule.
Since tomorrow you will know the answer, I can advance that the patient has a 3 cm rounded mass in the left apex. This case is shown to emphasize the importance of looking at the apices. More to come!
hazy densities noted in the apical portion of the left lung which could be fatty tissues. Can we call this as apical cap sign?