Dr. Pepe’s Diploma Casebook: Case 33 – SOLVED!
Dear Friends,
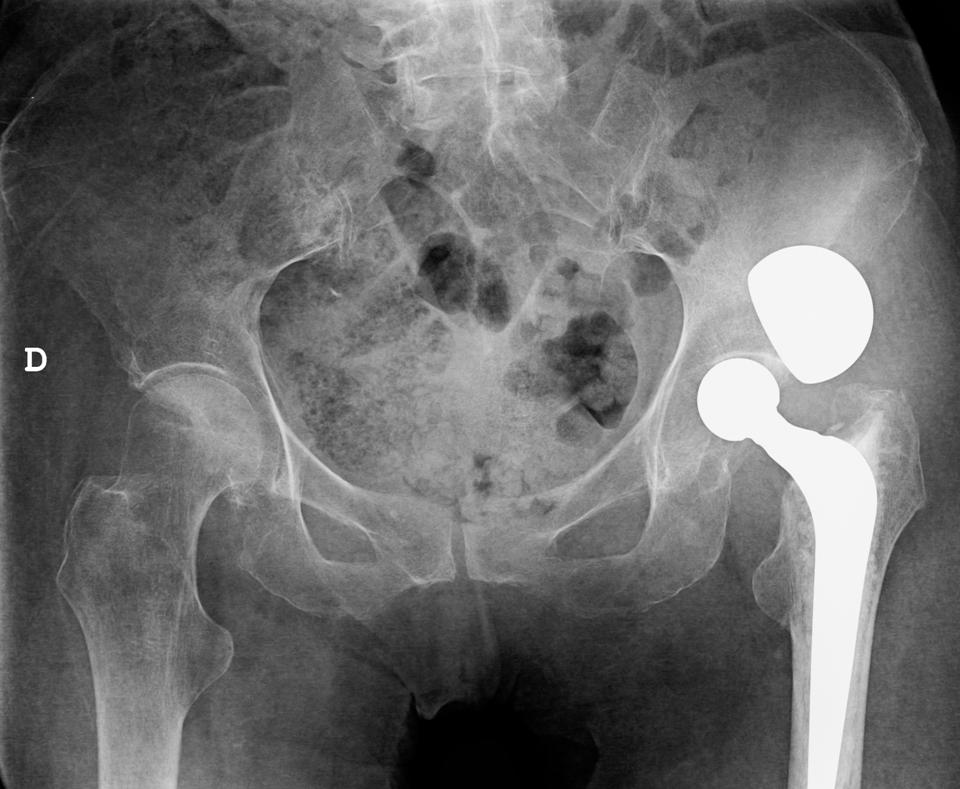
This week’s case features a 78-year-old woman after close reduction of a dislocated hip prosthesis.
Diagnosis:
1. Acetabular cup fracture.
2. Dissociation of bipolar hemiarthroplasty
3. Postoperative foreign body.
4. None of the above
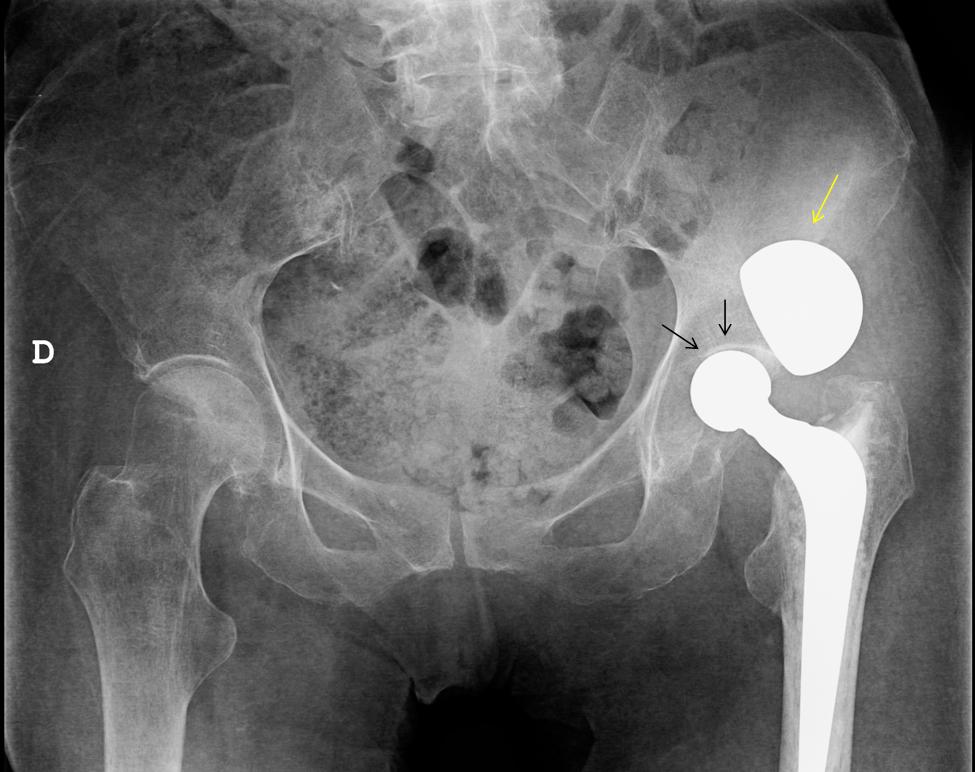
Findings: The head of the femoral component lies within the native acetabulum, which has a normal appearance without reaming (arrows). An “acetabular cup like” component lies outside the hip (yellow arrow). These findings suggest dissociation of a bipolar hemiarthroplasty as the most likely diagnosis.
To better understand these findings we should review the different types of hip arthroplasty:
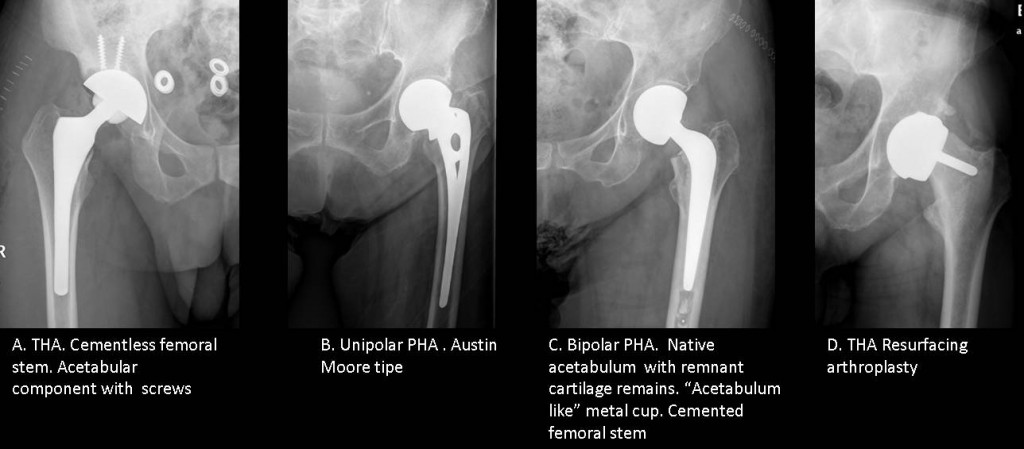
Total Hip Arthroplasty (THA): the femoral head and the acetabulum are replaced by prosthetic components (Fig 2a). The most common indication is osteoarthritis.
Partial Hip Arthroplasty (PHA): only the femoral head and neck are replaced. The most common indication is femoral neck fracture. There are two types:
a) Unipolar Hip Prostheses: femoral stem with a head that articulates with the native acetabulum (Fig 2b)
b) Bipolar Hip Prostheses: polyethylene lined metal cup with a small femoral head (Fig 2c)
Resurfacing arthroplasty: Only the articular surfaces are replaced. May be total or partial (Fig 2d)
Dislocations are more common in total hip replacement than in hemiarthroplasty and they typically occur between the femoral component and the acetabular component (Fig. 3).
Factors predisposing to dislocation include:
Patient factors: age, sex, weak hip musculature, excessive alcohol intake
Surgical factors: surgical approach, positioning of implant, previous hip surgery
Implant factors: femoral neck length, offset, head diameter
Dislocation is much more likely in the firsts 3 month following surgery. More common and more likely to be recurrent after a second total hip replacement. The usual treatment is closed reduction, particularly in early luxation. In late luxation, surgery is mainly used.
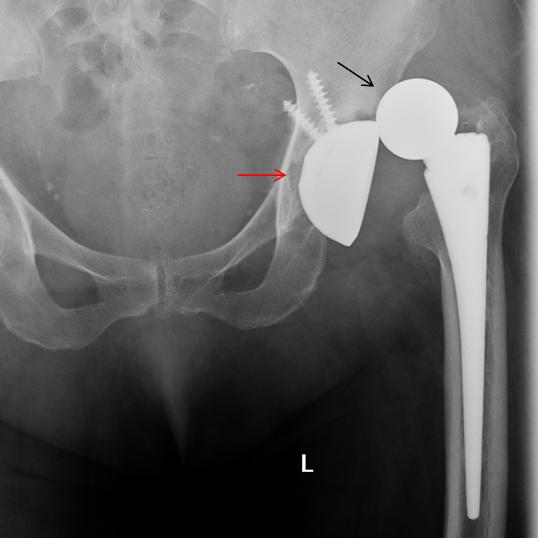
Fig 3 (above): femoral head dislocation (arrow) in a total hip prosthesis. The acetabular component (red arrow) remains in place.
Bipolar hip hemiarthroplasty have two components: a femoral stem with a small diameter head (red arrow) and a separate polyethylene-lined metal cup (yellow arrow). This system is designed to spare the cartilage in the hip socket because it moves on two ‘poles’. A theoretical advantage over unipolar components is a greater range of movement.
Dissociation of a bipolar prosthesis consists in a separation of the components usually the femoral head and the metal cup. Dissociations are quite uncommon. Sometimes they are produced during luxation itself, but they occur more commonly following closed reduction. For this reason, any attempt at reduction should be done under general anesthesia and fluoroscopic guidancel. During reduction, care should be taken to avoid twisting forces.
Always take a post- reduction radiograph to confirm proper placement. When there is dissociation, open reduction is mandatory (Fig. 5).
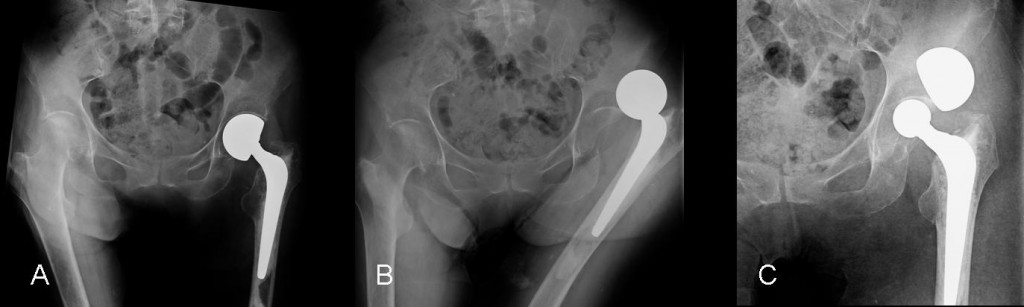
Fig. 5 (above): time sequence of dissociation of a bipolar prosthesis. A. Prosthesis is normally placed. B. There is dislocation of the prosthesis. C. After attempted closed reduction, there is dissociation of the prosthesis.
Follow Dr. Pepe’s advice:
- The radiologist should be familiar with the different types of hip prosthesis and with the most common general and type-specific complications associated with these devices
- The radiologists should be aware of the distinction between dislocation of a prosthesis and dissociation of its bipolar components.
Recommended reading: Current concepts of hip arthroplasty for radiologists. Part 1. Features and radiographic assessment. AJR 2012; 199:559–569
Current concepts of hip arthroplasty for radiologists. Part 2, Revisions and Complications. AJR 2012; 199:570–580
Case prepared by Carmen Torrents MD
diagnosis, hip, joint, musculoskeletal, prosthesis, radiography





Vi è una evidente dislocazione supero-esterna della coppa acetabolare, mentre la testa dell’artroprotesi rimane sul fondo acetabolare. Cioè è stata “ridotta ” la dislocazione della testa ma la coppa acebolare è lussata!
mi pare che la mia descrizione sia giusta o no !
Although you use the word “dislocation” instead of “dissociation”, I think your interpretation is correct