
Dear Friends,
Over the last couple of years, one of the last sessions at the ECR has always covered 20 interesting cases from various subspecialties, which the audience is asked to solve in an interactive way to broaden and update their knowledge.
In between, the very best submissions from the global radiological community have been presented in an interlude lecture. The best submission has always been awarded with a prize and a certificate.
Due to time limits, not all submitted cases can actually be shown onsite, but the session’s rising popularity has resulted in increasing numbers of submissions of excellent quality. This is why we would like to give our submitters the opportunity to reach a broader audience by posting the best cases here on the ESR Blog.
Read more…

RC 1910 – The hand and wrist, A-585 C- Tumours and tumour-like lesions
A short preview of lecture A-585 ‘C. Tumours and tumour-like lesions’, from the session RC 1910 ‘The hand and wrist’ at ECR 2014, given by E. Llopis from Valencia, Spain.
Watch the whole lecture and many more at http://ipp.myESR.org
Direct link: http://bit.ly/The_hand_and_wrist
Monday, March 10, 16:00 – 17:30 / Room E1
Abstract:
Radiological study of the wrist and hand is challenging due to its complex anatomy with many small structures and the number of normal bone and soft tissue variants that might mimic injuries. Moreover, many findings can be asymptomatic. Their knowledge is important to avoid misdiagnosis. During this lecture we will also review the role of the different imaging modalities, such as plain films for wrist alignment and bone structures as well as the important role of US and MR in differentiating tumour from tumour-like conditions. We will become familiar with some specific radiological findings that allow us to make accurate diagnoses of soft tissue and bone lesions.

E³ 920a – The treated spine and joints, A-246 A. Imaging of the postoperative spine (P.N.M. Tyrrell)
A short preview of lecture E³ 920a’ The treated spine and joints’, from the session A-246 ‘A. Imaging of the postoperative spine’ at ECR 2014, given by P.N.M. Tyrrell from Oswestry, United Kingdom.
Watch the whole lecture and many more at http://ipp.myESR.org
Direct link: http://bit.ly/The_treated_spine_and_joints
Saturday, March 8, 10:30 – 12:00 / Room A
Abstract:
Spinal surgery is most frequently performed to decompress (disc herniation, stenosis, malignant infiltration), fuse and stabilise (particularly following trauma or infiltrative destructive processes) and correct deformity. Often, there may be a combination of these procedures at one operation. Surgical instrumentation or bone graft is sometimes employed. Patients may present themselves with symptoms early or late following the procedure. This interactive session seeks to address the variety of surgical procedures undertaken and subsequently imaged post-operatively because of symptoms. The session aims to help one to understand and become familiar with the expected post-operative imaging appearances related to the surgical procedure, learn about abnormal pathological features as a cause of symptoms in the acute and more chronic situation and explore the diagnosis and differential diagnosis. This may include post-operative fibrosis versus recurrent disc herniation versus post-operative infection. Failure of fusion due to failure of instrumentation or inadequate take of bone graft can give rise to pseudoarthrosis. Recurrent stenotic symptoms may relate to an inadequate decompression, recurrent disc herniation, post-operative haematoma, extension of a malignant process or ischaemic damage.

Watch this session on ECR Live: Monday, March 10, 08:30–10:00, Room B
Tweet #ECR2014B #SF16a
Shoulder imaging and intervention are becoming more important in clinical practice as ageing populations and patient expectations have increased demand. The shoulder is also one of the joints in the human body that can suffer from a number of pathologic conditions, in both young and elderly patients, such as rotator cuff tears and tendinosis, subacromial-subdeltoid bursitis, calcific tendinopathy, and degenerative conditions.
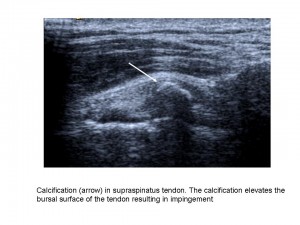
Shoulder imaging and surgery have developed in parallel over the last 20 years, and the introduction of minimally invasive surgical techniques has revolutionised shoulder interventions, which have been facilitated by accurate pre-operative diagnosis. The shoulder is an anatomic area that is very commonly evaluated with musculoskeletal ultrasound as it is accurate, quick, cheap, easily performed, well-tolerated by patients and can be combined with a dynamic examination and interventional procedures.
“MRI provides more general information about the shoulder, but many patients find the examination unpleasant due to noise and pain. Others are excluded from MRI because of claustrophobia or having an embedded electronic device such as a pacemaker. Also MRI cannot be performed as a dynamic examination, it often misses rotator cuff calcification, and the equipment is very expensive. As in many other fields, both techniques rely on high-quality equipment and are operator or interpreter dependent”, said Dr. Ian Beggs, musculoskeletal radiologist at the Royal Infirmary of Edinburgh.
Read more…

Watch this session on ECR Live: Thursday, 16:00–17:30, Room E2
Tweet #ECR2014E2 #MS3
Malignant primary bone tumours like osteosarcoma and Ewing’s sarcoma are very serious diseases mainly affecting children and teenagers. General radiologists are not likely to see these patients every day at their practice, but when they do, they must know what they have to do to optimise patient care and improve outcomes. Experts will give instructions and share useful advice during the dedicated Multidisciplinary Session today at the ECR.
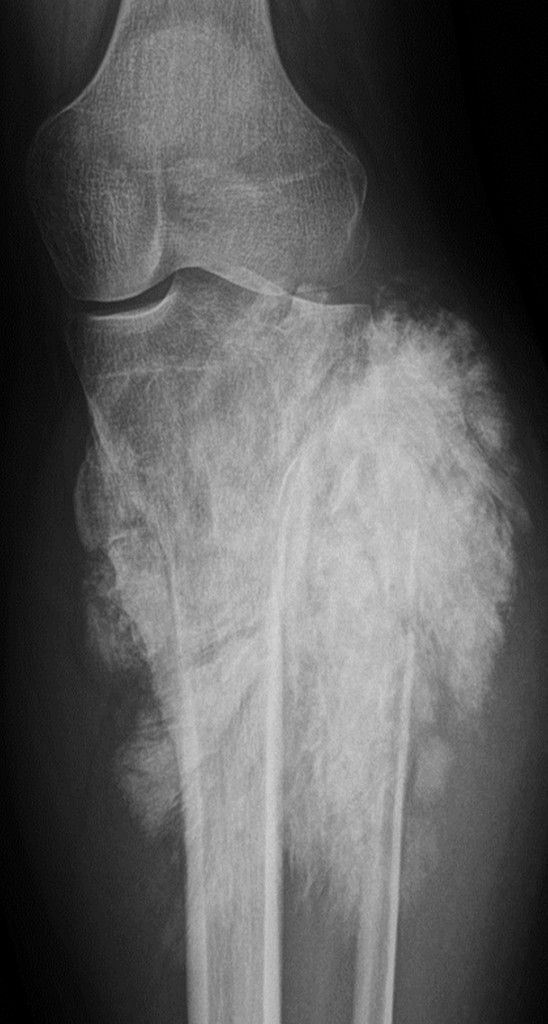
Conventional x-ray of a tumour in the knee
(Image provided by Prof. Koenraad Verstraete)
Read more…

A-585 B. Peripheral skeleton
V.N. Cassar-Pullicino | Monday, March 11, 10:30 – 12:00 / Room A
In this interactive session focussing on peripheral musculoskeletal lesions presenting to the Accident and Emergency Department, we will review the strengths and weaknesses of the imaging modalities applied to chosen bone, joint and soft tissue lesions. The imaging-based approach will strengthen the understanding of the different pathological entities which vary from trauma to infection in both the paediatric and adult age groups.

B-0931 Dynamic contrast-enhanced imaging for detection of complications after double-bundle reconstruction of the anterior cruciate ligament
Y.-C. Lin, Y.-H. Juan, Y.-C. Cheung, W.-L. Yeh, C.-H. Chiu, C.-F. Tan, C.-M. Kuo | Monday, March 11, 14:00 – 15:30 / Room E1
Purpose: Double-bundle reconstruction with stump preservation has revolutionized the surgical treatment for anterior cruciate ligament (ACL) injury. However, poor revascularization at the osteoligamentous interface (OI) of the tibia tunnel remains a major cause of graft complications. In this study, we applied dynamic contrast-enhanced (CE) magnetic resonance imaging (MRI) to quantify the OI enhancement values of the tibia tunnels and ACL stump. We aimed to determine the relationship between graft complications and OI and stump enhancements.
Methods and Materials: From October 2011 to April 2012, 34 patients were enrolled in our study (mean postoperative duration, 7.3 months). All patients underwent one 1.5-T MRI study with the imaging pulse-sequence protocol of proton density-weighted imaging (WI), T2WI, pre-enhanced and post-enhanced T1WI, and dynamic CE MRI. Graft complications, including cystic degeneration and tear, were evaluated using pre-enhanced MRI, and peak enhancement (ePeak) values were acquired from a dynamic CE study. The receiver operating characteristic (ROC) analysis was used to obtain optimal cut-off values for complicated grafts.
Results: Our study included 28 patients (mean age, 25.5 years). Nine patients (32.1%) had cystic degeneration and 1 (3.6%) had complete posterolateral (PL) bundle tear. Mean ePeak percentages for graft with or without complications were 84.19%/127.69% for anterior–medial (AM) bundle, 107.54%/128.21% for PL bundle, and 171%/151.06% for stump, respectively. ROC analysis yielded the optimal ePeak cut-off values of 126 %, 104 %, and 35 % for AM bundle, PL bundle, and stump, respectively.
Conclusion: Graft complications were directly associated with higher tibial OI values but inversely associated with higher stump values.

A-149 Chairman’s introduction
V.N. Cassar-Pullicino | Friday, March 8, 16:00 – 17:30 / Room C
In this New Horizon session dedicated to cartilage imaging, the audience will learn of new advances in imaging the normal and abnormal cartilage matrix and understand the basic techniques used in this assessment. It is hoped that these new techniques which are currently in the research field would very soon be translated into clinical application. Early detection of cartilage disease may lead to novel therapies which can help reverse and repair the degenerative process.

B-0188 Dynamic contrast-enhanced MRI can assess vascularity within pseudarthrotic clefts and predicts good clinical outcome
M.-A. Weber, K. Bloess, I. Burkholder, D. Bender, G. Schmidmaier, H.-U. Kauczor, O. Schoierer | Thursday, March 7, 14:00 – 15:30 / Room E1
Purpose: To prospectively evaluate whether dynamic contrast-enhanced (DCE) MRI can assess vascularity within pseudarthrotic clefts and predicts clinical outcome better than the clinical non-union scoring system (NUSS).
Methods and Materials: Sixty-four patients (mean age, 49.3 years) with non-union of an extremity fracture in computed-tomography received 3-Tesla MRI including DCE (coronal T1-weighted fat-saturated VIBE, TR/TE=3.76/1.35ms, 17 measurements, 2 mm slice thickness) after 0.1mmol/kg body-weight of gadoterat. We assessed vascularity within the pseudarthrotic cleft using a region-of-interest analysis. Signal intensity curves were subdivided into those with more intense contrast-agent uptake in the pseudarthrotic cleft than in normal adjacent muscle tissue (vascularised non-union) and those with similar or less uptake. The pharmacokinetic parameters of the Tofts model (Ktrans, Kep, iAUC, Ve) were correlated to the clinical outcome at one-year follow-up (n=37).
Results: Despite inserted osteosynthesis material, DCE parameters could be evaluated in n=60 at first visit. Sensitivity/specificity of vascularised non-unions as indicator of good clinical outcome was 77.3%/46.7% compared to 95.5%/26.7% using NUSS. Logistic regression revealed non-significant impact of NUSS on clinical outcome (p=0.27, odds ratio=0.97). At first examination, median iAUC (initial area under the enhancement curve) was 24.13 in patients with good outcome compared with 10.96 in non-responders (p=0.032), while Ktrans, Kep, and Ve were not significantly different. Using a receiver operating characteristic analysis, sensitivity/specificity of iAUC at the optimal cut-off value of 17.5 to predict outcome was 68.2%/76.9%. All pharmacokinetic parameters did not change significantly at the one-year control (n=18).
Conclusion: DCE MRI can assess vascularity in pseudarthrotic clefts. A vascularised non-union indicates good clinical outcome.

A-153 CEST (chemical exchange saturation transfer)
B. Schmitt | Friday, March 8, 16:00 – 17:30 / Room C
CEST imaging in principle relies on the chemical exchange of protons bound to solute molecules and surrounding bulk water molecules. The effect can be used for MRI because the magnetization of each solute proton, is also transferred to bulk water, and can thus be visualized via the MR signal. CEST effects can be evaluated for specific molecular groups due to their characteristic proton resonance frequencies, which provides the technique with a high intrinsic sensitivity to these groups. In healthy cartilage tissue, strong CEST effects from exchangeable protons of glycosaminoglycan (GAG) molecules can be observed. The magnitude of these effects decreases when concentration ratio between bulk water protons and GAG protons decreases, e.g. in the early stages of osteoarthritis (OA). Initial studies on patients after cartilage repair surgery with GAG-dependent CEST (gagCEST) imaging have demonstrated that it is feasible to visualize GAG loss in vivo at 7.0 Tesla. Initial reports also claim that the technique might be transitioned to the clinical field strength of 3 T. Although CEST imaging can be performed with standard clinical equipment and protocols can easily be implemented in a routine clinical workflow, the signal analysis in gagCEST imaging and the reading of gagCEST images are technically complex. For example, effects, which alter the T2 relaxation time of tissue such as high relative water concentration, can affect the magnitude of gagCEST effects although the absolute concentration of GAG is unchanged. Unless confounding effects are automatically corrected, careful analysis of images is necessary for proper interpretation of results.











