
Recent studies have raised the problem of dose optimisation imaging protocols in patients with renal colic. Some of them are written by emergency physicians, who seem to pay more attention to this problem than radiologists. We would like to hear what you think about this issue in the comments section below.
Renal colic is a common problem, which is increasing in incidence, affects 10%-15% of people over during their lives, and has a tendency to recur. The ability to rapidly identify kidney stones, as well as their position along the ureter and their dimensions, with high sensitivity and specificity using unenhanced CT, has made this technique the first-line approach to the condition. Since CT involves ionising radiation and there is growing concern about its possible carcinogenic effects, low-dose CT protocols for urolithiasis have been developed to minimise radiation risk.
However, low-dose images and often considered as low-quality images and, although these protocols have been shown to be accurate for stone detection, there are concerns about their use due to fears of missing other diagnoses that may clinically mimic stone disease, such as appendicitis, diverticulitis, and cholecystitis. A possible solution could be to use different CT protocols according to the pre-test probability of stone disease. In patients with a previous history of urolithiasis, a low-dose CT examination would be sufficient.
Read more…

To select the right treatment at the right time for your patient is a common slogan used to describe personalised medicine (PM): a new vision of healthcare which is already becoming a reality today. Different “omics” approaches such as genomics, proteomics or metabolomics allow patients’ predispositions to certain diseases or treatment response to specific medication to be predicted.
What is the role of radiology and radiologists in PM?
In the recent white paper, published by the ESR Working Group on Personalised Medicine (Insights Imaging (2015) 6:141–155), the authors emphasise the key roles medical imaging plays in PM. The authors clearly specify all areas and give examples of the unique and personalised information provided with medical imaging technologies.
In a substantial number of diseases, the first step leading from clinical symptoms to a diagnosis relies on imaging. Imaging has played this role for decades: assessing the location and extent of a disease in individual patients and characterising structural abnormalities and physiological environment, thus providing crucial information for the choice of the right treatment.
Read more…
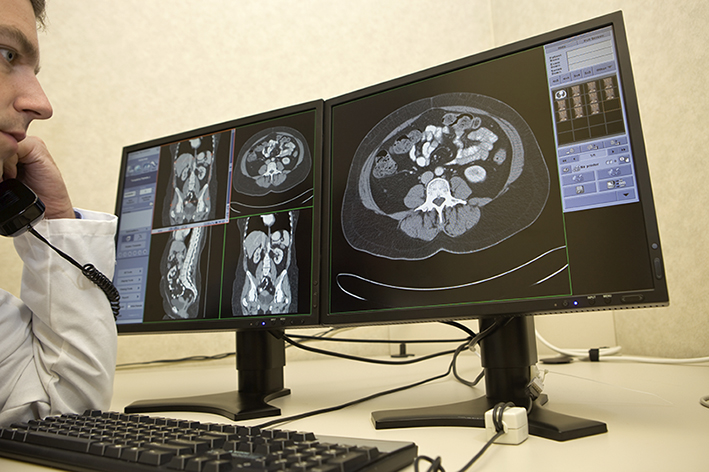
Survey results show that the radiologist’s availability to clinical colleagues is an important part of the imaging service. So how do you balance that availability and your regular workflow? We want to hear your thoughts below.
In 2011, Lindsay et al. published the results of a survey aimed at assessing what factors affected satisfaction with radiology services amongst referring clinicians (1). The survey was conducted shortly after implementation of a PACS system across three hospitals, and focused mainly on the changes created by improved communication between radiology and other hospital departments. Overall, respondents had a positive opinion of the impact of PACS installation, with the majority feeling it decreased the reporting times and ameliorated the working pattern for medical staff. Furthermore, there were a number of indicators showing that direct access to the radiological images did not decrease the importance of the radiology reports. On the contrary, the higher the experience of the referring clinicians, the higher the perceived value of this part of the radiologists’ work.
Read more…
A recent article in the New England Journal of Medicine raises some very interesting questions about the future of imaging service provision. Who are we as radiologists, and where do we want to go? Are we running “imaging factories” or “clinical imaging services”? We would like to hear what you think in the comments section at the bottom of this article.

Are modern radiologists just cogs in an image production machine?
Dr. Saurabh Jha is a radiologist working in the Department of Radiology at the Hospital of the University of Pennsylvania, Philadelphia. Before that, he had a professional life as a surgical trainee on this side of the pond, in England. In a paper entitled From imaging gatekeeper to service provider – a transatlantic journey
(N Engl J Med 2013:369:5-7) he underlines the differences between the way he perceived radiologists when he worked in Europe as a surgeon and the way he practices radiology in the USA. English radiologists were gatekeepers: that is, they provided imaging studies only when they were really appropriate and necessary according to their clinical judgement. American radiologists are service providers; that is they perform and read the examinations requested according to the referring physicians’s clinical judgement.
“Evaluation of radiological services in the USA is based on the volume of examinations and turnaround time; the higher the number of studies, the better it is for the department.”
Dr. Jha explains that this difference is mostly related to the fact that imaging was a scarce commodity when he was working for the British National Health Service while, on the contrary, there is abundance of CT scanners, MRI machines, and technologists in the United States. Another explanation is that evaluation of radiological services in the USA is based on the volume of examinations and turnaround time. In such a case, the higher the number of studies, the better it is for the department.
Read more…



