Radiologists must be thorough when investigating malignant primary bone tumours
Watch this session on ECR Live: Thursday, 16:00–17:30, Room E2
Tweet #ECR2014E2 #MS3
Malignant primary bone tumours like osteosarcoma and Ewing’s sarcoma are very serious diseases mainly affecting children and teenagers. General radiologists are not likely to see these patients every day at their practice, but when they do, they must know what they have to do to optimise patient care and improve outcomes. Experts will give instructions and share useful advice during the dedicated Multidisciplinary Session today at the ECR.
Malignant primary bone tumours are very rare and affect less than five or six patients per million a year, according to Koenraad Verstraete, professor of radiology and chair of the radiology department at Ghent University Hospital, Belgium. The average radiologist may only seldom encounter this disease, but he or she is often the first one to discover it. The imaging strategy chosen by the radiologist will, therefore, considerably influence patient management, said Verstraete, who will chair the session
“You can discover it by accident, for instance when examining patients with pain in the knee or a limp. It is the burden of the radiologist who makes the first x-ray or first MRI to interpret the image correctly and refer the patient to the appropriate centre. It can also occur that you will be responsible for local follow-up of the patient after surgery,” said Verstraete, who will speak about osteosarcoma and Ewing sarcoma, two major malignant bone tumours usually found in children. He will also briefly present attendees with images of other malignant bone tumours, such as chondrosarcoma and adamantinoma, to complete his presentation.
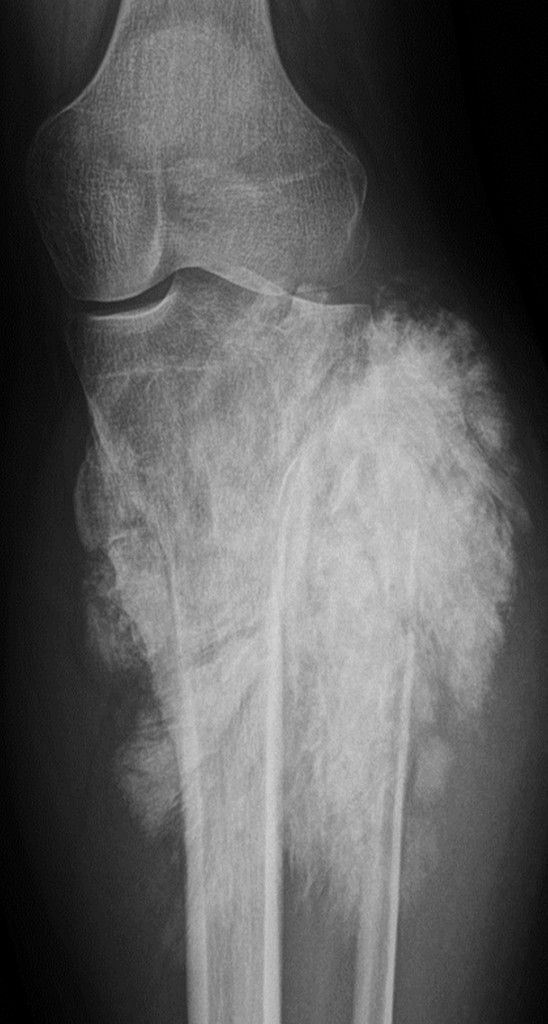
The first task of the radiologist is to make the right diagnosis, usually with conventional x-ray. Ewing’s sarcoma may look like an infection, Verstraete said. The session will teach attendees how to differentiate a tumour from an infection by searching for fat cells in the bone marrow – which are typically present in the case of an infection and absent in the case of a tumour.
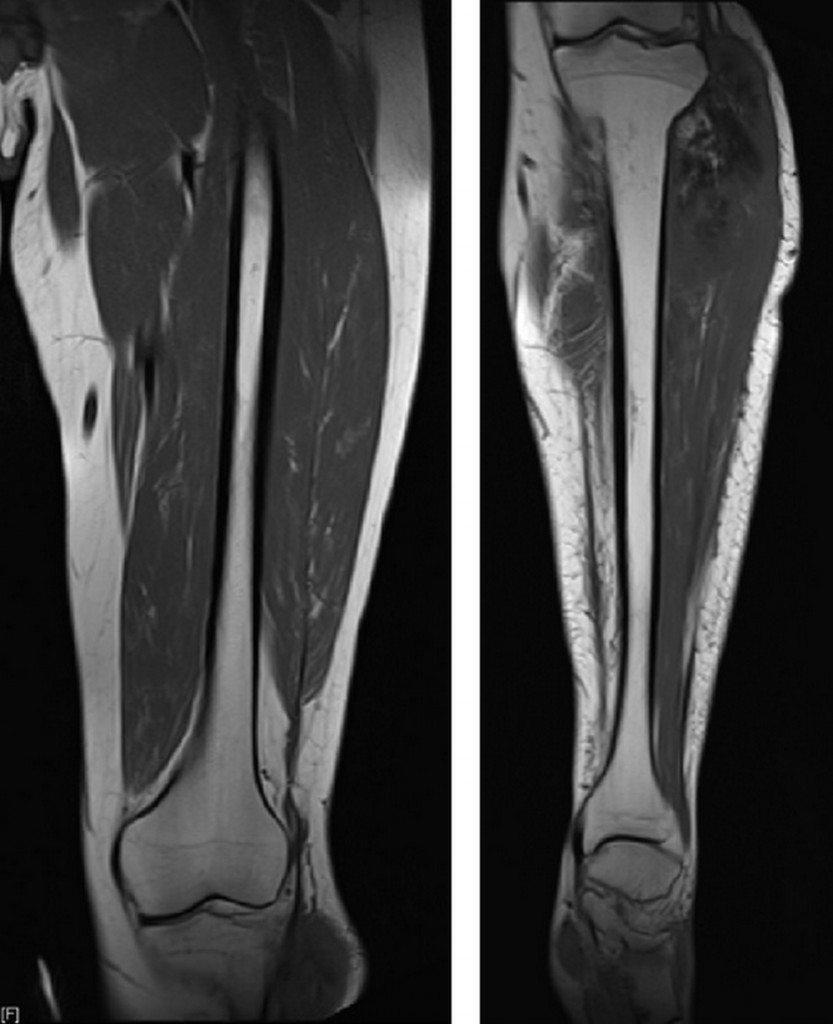
The second task is to perform local staging of the tumour, to let the surgeon know where the tumour is invading the joint, muscle, nerves or vessels. MRI is the modality of choice, and radiologists should not only image the knee, but also the whole upper or lower leg for skip lesions, according to Verstraete.
“Local staging is often done by general radiologists, but they often forget to image the whole femur or tibia, because these tumours mostly occur in the knee. When a patient is referred to a tumour centre with an MRI of the knee, surgeons want to know if, for instance, the whole femur is also invaded and how far. So an important message to radiologists is to please also make images of the whole bone,” he explained.
Radiologists must also prevent the local orthopaedic surgeon from performing a biopsy at this stage. “This should be done in the referral centre by the oncologic surgeon who will perform the surgery. When the local orthopaedic surgeon does the biopsy, this can really go the wrong way and end with amputation. The radiologist should say to the local surgeon to not do anything and send the patient directly to referral centre,” he insisted.
The third task for radiologists is to determine the site of biopsy so they can show the oncologic surgeon where the most active part of the tumour is and which route they should take. At this stage, the patient is already in a specialised tumour centre where oncologists, pathologists, radiologists and surgeons are in charge of his/her management. Dynamic contrast-en¬hanced MRI is helpful for finding the best site of biopsy, by looking at the vascularity of the tumour and leading the surgeon towards its most malignant part.
After local staging, radiologists must also do distant staging, usually with a CT scan of the lungs, a com¬mon site of metastases with these tumours. Based on the results of the biopsy and staging, the medical team will decide what kind of therapy is needed. In the case of neoadjuvant chemotherapy, the patient will receive chemotherapy for three months prior to surgery. “The aim of the procedure is to kill the tumour and invisible micro-metastases, and make it shrink as much as possible before surgery. In this time, doctors also have the time to prepare a prosthesis, which will serve to replace the knee,” he said.
Assessment of treatment response before surgery is crucial and radiologists must perform another imaging study after three months. Once again, they will use dynamic contrast-enhanced MRI to see whether the tumour, and especially tumour vascularity, has decreased since the first MRI scan was carried out during local staging. The response rate is divided in two groups; the group with good response and the one with poor response. The cure rate can be as high as 70 to 75% for the group with good response and as low as 40 to 45% for the group with poor response.
Chemotherapy continues for about a year after surgery, and imaging also plays a key role in patient follow-up, detecting potential recurrence and complications after prosthesis placement or amputation. The most widely used imaging modalities to follow up patients with prostheses are x-ray and ultrasound, because prostheses can lead to metal artefacts in MRI. Radiologists also perform lung CT scans to see if there are any metastases. The usual frequency for follow-up is every three months after the first two years of surgery, and then every six months from the third to the fifth year.
Close cooperation with all the other physicians involved is key to patient management. “In all decision-making, we always use the multidisciplinary approach. We all sit together at the time of diagnosis, and before and after surgery. The multidisciplinary approach determines the whole diagnostic and therapeutic sequence,” said Verstraete, whose presentation will be followed by talks by the oncologist Dr. Catharina Dhooge and orthopaedic surgeon Dr. Gwen Sys from Ghent University Hospital.
The session will end with the case presentation of a patient who Verstraete and his colleagues treated for a year, and should serve as an example of teamwork by detailing the tasks of every physician involved in the case.
Multidisciplinary Session
Thursday, 16:00–17:30, Room E2
MS 3: Multidisciplinary approach for detection and treatment of malignant primary bone tumours
» Chairman’s introduction
K. Verstraete; Ghent/BE
» Imaging malignant primary bone tumours
K. Verstraete; Ghent/BE
» Oncologic approach to malignant primary bone tumours
C. Dhooge; Ghent/BE
» Surgical approach of malignant primary bone tumours
G. Sys; Ghent/BE
» Case presentation and discussion



Very usefull! Thanks 🙂