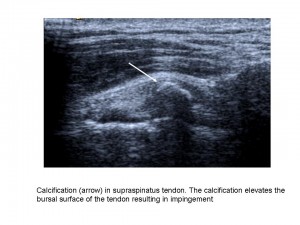
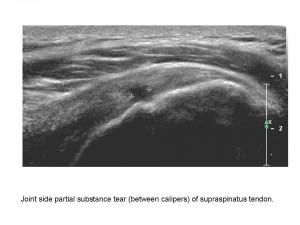
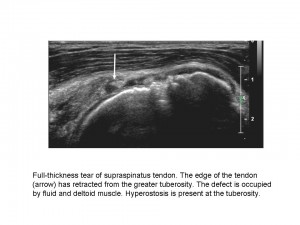
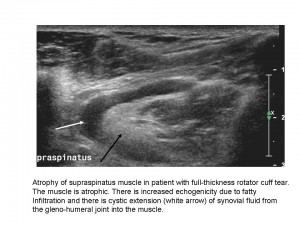
Shoulder imaging and intervention
Watch this session on ECR Live: Monday, March 10, 08:30–10:00, Room B
Tweet #ECR2014B #SF16a
Shoulder imaging and intervention are becoming more important in clinical practice as ageing populations and patient expectations have increased demand. The shoulder is also one of the joints in the human body that can suffer from a number of pathologic conditions, in both young and elderly patients, such as rotator cuff tears and tendinosis, subacromial-subdeltoid bursitis, calcific tendinopathy, and degenerative conditions.
Shoulder imaging and surgery have developed in parallel over the last 20 years, and the introduction of minimally invasive surgical techniques has revolutionised shoulder interventions, which have been facilitated by accurate pre-operative diagnosis. The shoulder is an anatomic area that is very commonly evaluated with musculoskeletal ultrasound as it is accurate, quick, cheap, easily performed, well-tolerated by patients and can be combined with a dynamic examination and interventional procedures.
“MRI provides more general information about the shoulder, but many patients find the examination unpleasant due to noise and pain. Others are excluded from MRI because of claustrophobia or having an embedded electronic device such as a pacemaker. Also MRI cannot be performed as a dynamic examination, it often misses rotator cuff calcification, and the equipment is very expensive. As in many other fields, both techniques rely on high-quality equipment and are operator or interpreter dependent”, said Dr. Ian Beggs, musculoskeletal radiologist at the Royal Infirmary of Edinburgh.
Several studies have shown US and MRI to be equally accurate in the detection of rotator cuff tears and tendinosis. The accuracy in full-thickness tears is above 90%, but is substantially lower for partial thickness tears. MR arthrography improves diagnostic accuracy by a few percentage points for full-thickness rotator cuff tears and by a substantially larger margin in partial-thickness tears but is invasive and carries a risk of causing joint infection. MR arthrography is also the best imaging method for assessing shoulder instability. Ultrasound is superior in assessing rotator cuff calcification and can be used for dynamic examinations and for interventions. When it comes to the importance of performing dynamic manoeuvers in the diagnosis of rotator cuff impingement, experts seem to be divided on the issue.
“Some people believe that a dynamic US examination is essential in identifying and diagnosing impingement. Others believe that impingement is a clinical diagnosis or best confirmed by injecting local anaesthetic (often under ultrasound guidance) to see if this abolishes the impingement symptoms,” Dr. Beggs explained.
Being inexpensive, readily available, and radiation-free, ultrasound is the imaging modality of choice for guiding interventional procedures around the shoulder. Thanks to its high resolution and multiplanar capabilities, ultrasound can be used to guide needles precisely in the tendons of the rotator cuff, the bursa or the gleno-humeral and acromio-clavicular joints.
“Different kinds of procedures can be performed around the shoulder. Except for simple intra-articular or intra-bursal steroid injections, I think that the most interesting procedures are the treatment of tendinopathies. Calcific tendinopathy is a very common condition that can be very painful and disabling. After local anaesthesia, intra-tendinous calcifications can be dissolved and re-aspirated using simple saline solution under US guidance. This procedure is very quick and easy, and it allows excellent results to be obtained. More recently, injection of platelet-rich plasma within rotator cuff tendons has been demonstrated to be effective in improving degenerative tendinopathy. Although these procedures are very minimally invasive, they should be regarded as surgical procedures. However, the risk of adverse events is extremely low and could be considered negligible,” said Dr. Luca Sconfienza, radiologist at the Policlinico San Donato in Milan/Italy, on the wide range of US-guided interventions in the shoulder.
The main disadvantage of this modality is that the ultrasound beam cannot correctly visualise abnormalities of the subcortical bone, and therefore it cannot be used to guide procedures aimed at treating those lesions. Experience is of the greatest importance when performing ultrasound-guided interventions in the shoulder. The operator should not only be experienced in manually performing the procedure but also in evaluating and following up patients from the clinical point of view, and appropriate training is essential.
Finally, when asked about future developments and hot topics, Dr. Beggs had this to say: “Developing themes include the realisation that there is a high prevalence of asymptomatic rotator cuff tears in older patients and that not all tears require surgery; the importance of assessing fatty atrophy and infiltration of the rotator cuff muscles in patients with rotator cuff tears, as fatty atrophy indicates a poor functional prognosis as the muscle damage is irreversible; and the apparent efficacy of US-guided interventions, although this last point is controversial. Several studies have shown the advantage of US-guided injections, but one well-known study showed that blind injections of steroids into the buttocks were as effective as US-guided shoulder injections in patients with impingement”.
Special Focus Session
Monday, March 10, 08:30–10:00, Room B
SF 16a: Shoulder imaging and intervention
» Chairman’s introduction
I. Beggs; Edinburgh/UK
» US of the rotator cuff
A. Plagou; Athens/GR
» MRI of the rotator cuff
S. Waldt; Munich/DE
» US-guided interventions of the shoulder
L.M. Sconfienza; San Donato Milanese/IT
» Panel discussion:
Controversies and confusion in shoulder imaging