
Watch this session on ECR Live: Thursday, March 2, 16:00–17:30, Room X
#ECR2017
Imaging data is key in multicentre clinical trials for cancer research but quality control is currently a major impediment, bringing the validity of the trials into question and potentially impacting on the quality of drugs put on the market, a panel of experts will argue today in a session held by the ESR and the European Organisation for Research and Treatment of Cancer (EORTC) at the ECR.
Imaging is increasingly contributing to cancer research thanks to the development of innovative techniques that depict functional and molecular processes. In most oncological clinical trials, imaging is now the primary criteria used to evaluate progression of disease or efficiency of the drug being tested.
The best way to obtain valuable imaging measurements is to involve the imagers who take part in these trials and educate the clinician investigators, experts will explain in the session.
When it comes to imaging in cancer research, a number of issues take centre stage. Difficulties associated with integrating imaging biomarkers into trials have been neglected compared with those relating to the inclusion of tissue and blood biomarkers, largely because of the complexity of imaging technologies, safety issues related to new contrast media, standardisation of image acquisition across multivendor platforms and various post-processing options available with advanced software, as reported recently in The Lancet by the EORTC and leading researchers.
Read more…

Watch this session on ECR Live: Wednesday, March 1, 16:00–17:30, Room F2
#ECR2017
There is hardly any area of hospital medicine where interventional radiology (IR) has not had some impact on patient management. The range of conditions that can be treated using interventional radiology techniques is continually expanding.
In today’s session, experts will provide an insight into image-guided interventions in oncology with a particular focus on illustrating the importance of quality assurance in image-guided oncological interventions and their effect on treatment outcomes.
In recent years, IR has played a vital role in the field of oncology, and alongside medical, surgical and radiation oncology it constitutes a key pillar in cancer care. Vascular and non-vascular procedures such as transarterial chemoembolisation, radiofrequency ablation (RFA), microwave ablation, radioembolisation, cryoablation and high-intensity focused ultrasound (HIFU) are delivered locally, minimise damage to nearby tissue and avoid the systemic side effects of chemotherapy.
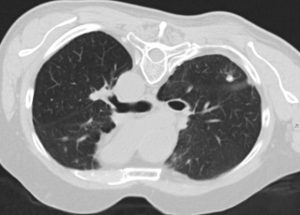
Colorectal lung metastasis before CT – guided microwave ablation.
For the interventional radiologist providing oncologic therapies it is essential to understand the rapidly changing field of oncology and to have a broad knowledge of oncologic diseases and available therapies to treat them. Radiologists providing image-guided interventions in oncology have an outstanding understanding of imaging as well as a diversity of interventional skills. However, they lack formal training in oncology and an understanding of chemotherapy and radiotherapy, according to Prof. Andy Adam from the Department of Radiology at Guy’s and St. Thomas’ Hospital in London. Read more…

Dear Friends,
This week, we have an oncologic patient with liver nodule detected on US examination. Below are the images from an MRI examination.
Possible diagnoses:
1. Liver hemangioma
2. Hepatocellular carcinoma (HCC)
3. Liver metastasis
4. Focal nodular hyperplasia (FNH)
Read more…


