
B-0889 Improved image quality for higher diagnostic accuracy of cranial computed tomography using iterative image reconstruction
H. Haubenreisser, C. Fink, P. Apfaltrer, B. Schmidt, M. Sedlmair, S.O. Schönberg, T. Henzler | Monday, March 11, 14:00 – 15:30 / Room B
Purpose: To prospectively compare the image quality of cranial computed tomography (cCT) with thin slice widths using traditional filtered back projection (FBP) and sinogram-affirmed iterative image reconstruction (SAFIRE).
Materials and Methods: 40 consecutive studies (19 men; 71.6±16.6 years) referred for cCT were prospectively included. Each cranial CT raw data set was reconstructed with FBP and SAFIRE with decreasing slice widths (5 mm-1 mm). Objective image quality was assessed by measuring image noise in three predefined regions of the brain (white matter, thalamus, cerebellum) using identical regions of interest (ROIs). Subjective image quality was assessed by 2 experienced radiologists by ranking the reconstructed data sets with respect to overall image quality. The Mann-Whitney U-test and Cohen’s Kappa were used for statistical analysis.
Results: Image noise was statistically significantly reduced in all SAFIRE images at identical slice widths when compared to the images reconstructed with FBP (4.26±0.43 HU vs. 7.67±1.19 HU at 1 mm slice width) (p<0.001). Mean signal attenuation for each region and slice width remained constant between the two reconstruction methods (p>0.5). SNR was comparable between 1 mm SAFIRE images and 5 mm FBP images. Subjective image quality of SAFIRE images was rated consistently higher than that of the FBP images (p<0.001). Interobserver agreement was excellent between both radiologists (Cohen’s K = 0.79-0.86).
Conclusion: Iterative image reconstruction significantly reduces image noise, while increasing image quality. In cCT this may be used to decrease slice width and thus reduce partial volume effects, which may lead to increased diagnostic accuracy.

A-162 Upper limb nerve entrapment
D. Weishaupt | Friday, March 8, 16:00 – 17:30 / Room E1
The peripheral nerves of the upper limb are affected by a number of entrapment and compression neuropathies. These syndromes involve the brachial plexus as well as the musculocutaneous, axillary, suprascapular, ulnar, radial and median nerves. Clinical examination and electrophysiological studies are traditionally the mainstay of diagnostic work-up. However, ultrasonography and magentic resononance imaging (MRI) may provide key information about the exact anatomic location of the lesion or may help to narrow the differential diagnosis. In certain patients with the diagnosis of a peripheral neuropathy, imaging using either ultrasononography of MRI may help establish the cause of the condition and provide information crucial for conservative management or surgical planning. In addition, imaging is particularly valuable in compex cases with discrepant nerve functions test results.

B-0012 Language impairment and reduced structural connectivity in Rolandic epilepsy
R. Besseling, J. Jansen, W.H. Backes | Thursday, March 7, 10:30 – 12:00 / Room C
Purpose: Rolandic epilepsy (RE) is a childhood epilepsy with mild seizure semiology and epileptic discharges originating from the sensorimotor (Rolandic) area. A serious co-morbidity in RE is language impairment, for which we aim to find a correlate using structural connectivity.
Methods and Materials: Diffusion MRI was performed at 3.0 Tesla and 2×2×2 mm voxel size with b=1200 s/mm2 and 66 diffusion gradient directions in 23 children with RE with proven language deficits and 23 matched controls. Constrained spherical deconvolution provided voxel-wise tract orientations and whole-brain tractography (5M streamlines). For each of the 4 Rolandic areas (bilateral pre- and postcentral gyri), the streamlines to any of the 70 regions, obtained by automatic cortical parcellation (Freesurfer), were selected from the whole-brain tractogram. For reliable connections (top 20 % of number of streamlines), connectivity was quantified by tract fractional anisotropy (FA), compared between groups, and correlated to language scores.
Results: In the left hemisphere, reduced tract FA was found for connections between the Rolandic areas and inferior frontal gyrus (Broca’s area) and supramarginal gyrus (Wernicke’s area), but not for contralateral homologue regions. For the aberrant connection between the left postcentral and inferior frontal gyrus, tract FA decreased with languages score in the RE group (p=0.04).
Conclusion: In RE structural connectivity between Rolandic and language areas is disturbed and correlates with the language dysfunction. This provides a neuronal link between the location of the epileptic discharges and the language impairment. This research was supported by the Dutch Epilepsy Foundation.

A-511 fMRI in epilepsy
N. Bargalló | Sunday, March 10, 16:00 – 17:30 / Room G/H
Functional MRI (fMRI) is a non-invasive tool that is capable to detect the subtle homodynamic changes produced in regional brain activation. The main fMRI clinical application until now is localization and evaluation of brain eloquent areas in surgical planning of brain pathology. fMRI application in epilepsy patients are language lateralization, memory function assessment and localization of ictal and interictal BOLD changes. There are several factors that can influence the results of a fMRI experiment such as the scan noise for the rest condition, the simplicity of the task performance, the monitoring of the experiment during the exam, how to achieve a real baseline condition and the most important, to use the most specific paradigm that would activate the selected brain areas. In practical approach, one must be aware that sometime fMRI studies are applied in paediatric or impaired cognitive epilepsy population when deciding the language or memory paradigm, and is recommended to use multiple and feasibility tasks to assure the results. fMRI for language lateralization is currently used in the clinical practice and provides comparable results to the intracarotid amobarbital test (IAT). In fMRI studies for memory function assessment, results show changes in epileptic patients, but further studies are required to validate this technique to an individual level. A new application is ictal or interictal fMRI with EEG recorded that provide more detailed information about simultaneously electrographic and homodynamic changes in the seizure process, with encouraging results for epileptogenic area localization and propagation patterns.

Watch this session on ECR Live: Saturday, March 9, 16:00–17:30, Room G/H
Advanced MR imaging techniques such as perfusion and functional imaging have been a great help in improving the diagnosis and staging of brain tumours. Unlike conventional MR techniques, advanced MR techniques can be used to obtain information not only on the morphological, but also on the functional characteristics of tumours.
One of the most common types of brain tumour is glioblastoma, which is highly malignant and has a high cell reproduction rate due to the fact that it is nourished by a large network of blood vessels. According to the American Brain Tumour Association there are two types of glioblastoma: primary glioblastomas, which tend to form and make their presence known quickly by growing aggressively, and secondary glioblastomas, which are also aggressive but show slower growth and only represent 10% of all diagnoses.
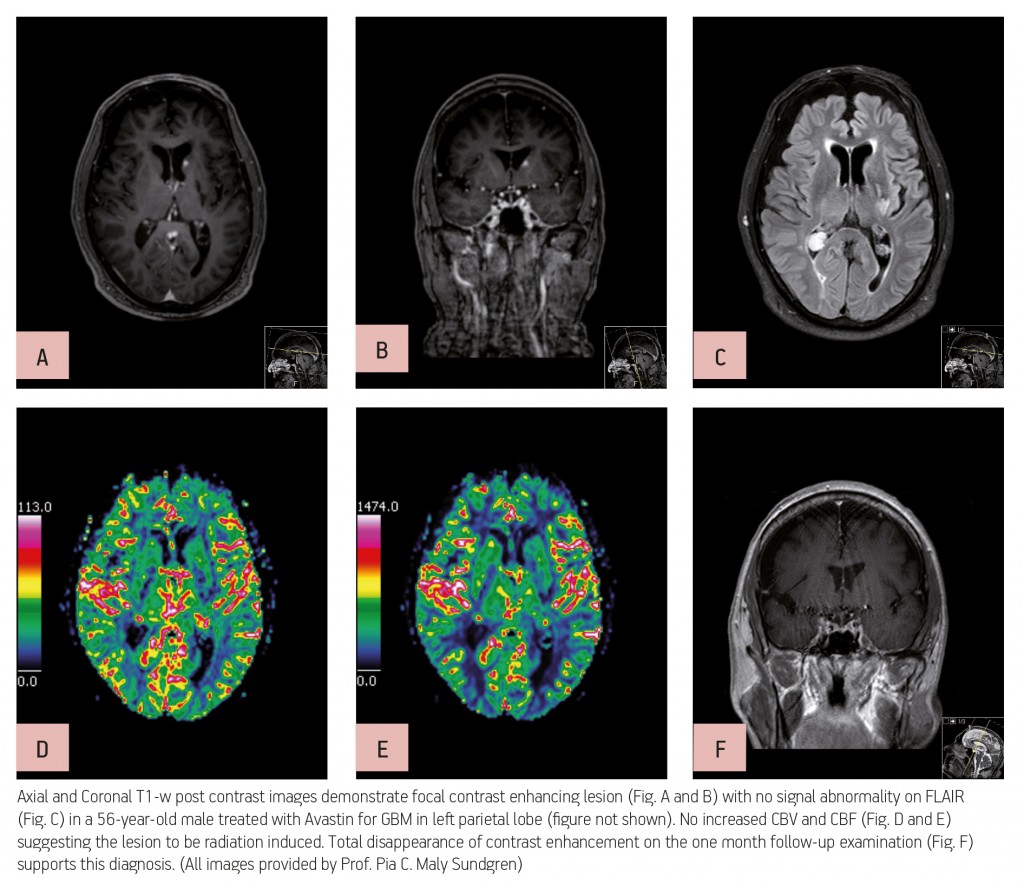
Read more…

Dear friends,
This week I want to show you a neuro/skeletal case, relating to a 25-year-old male with a 3-month history of sciatica.
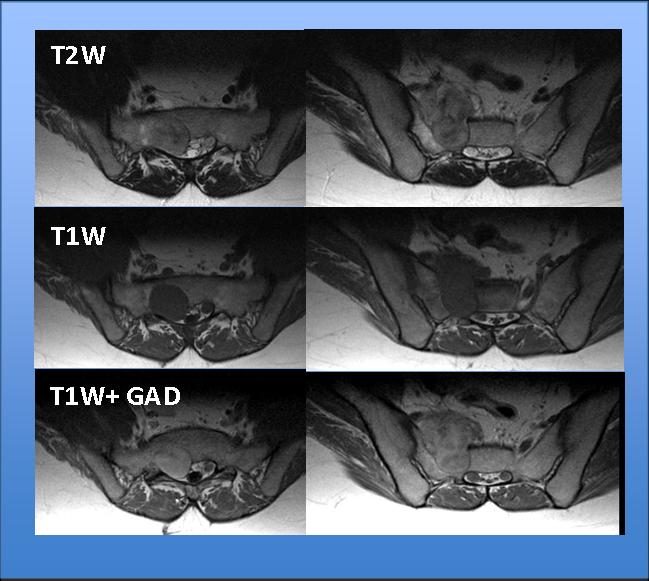
Fig. 1
Read more…

Dear Friends,
Following the usual pattern of an oral examination (mixed cases from all the subspecialities), I challenge you with the following neuro case, below.
Look out for the answer on Thursday. Good luck!
This week’s patient is a 61-year-old immunocompetent male with progressive disorientation and general weakness
Read more…








