Dr. Pepe’s Diploma Casebook: Case 111 – The Wisdom of Dr. Pepe (Chapter 4) – SOLVED!

Dear Friends,
To continue with the fourth chapter of The Wisdom of Dr. Pepe, I am showing PA radiograph of a 57-year-old woman with asthenia.
What do you see?
Check the image carefully, leave your thoughts in the comments section, and come back on Friday for the answer.
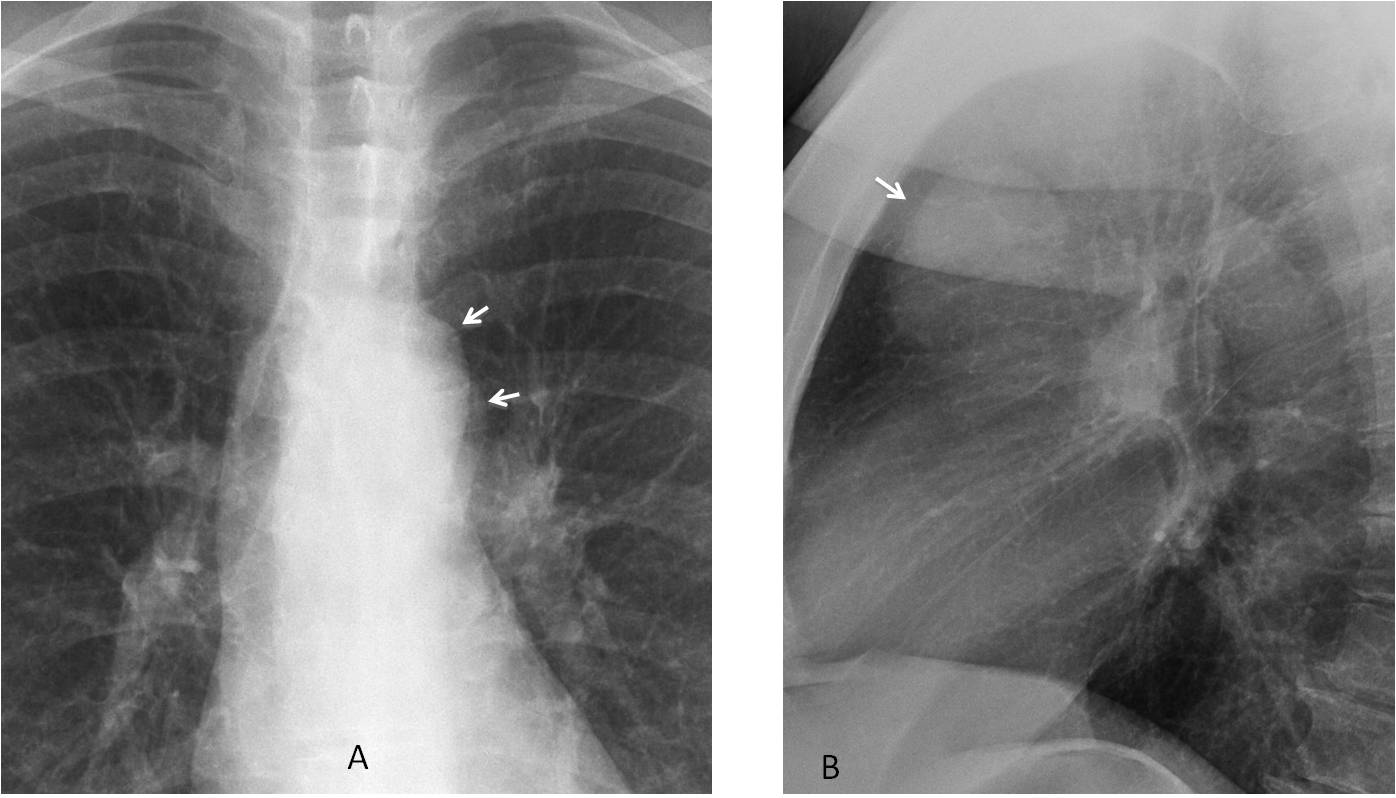
Findings: PA radiograph shows a double contour of the aortic knob (A, arrows). This finding is suspicious of a mediastinal mass that is not in contact with the aorta, placing it either in front or behind it. Lateral view confirms a large rounded mass in the anterior clear space (B, arrow).
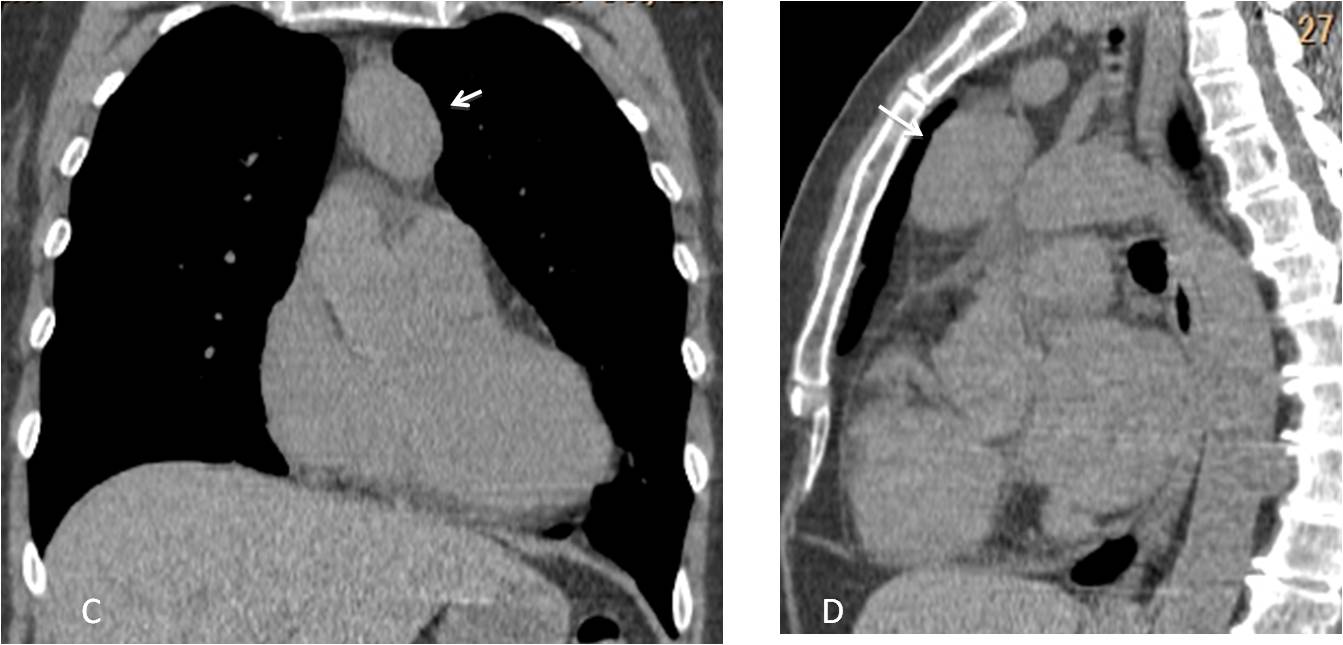
Coronal and sagittal unenhanced CT images confirm an anterior mediastinal mass (C and D, arrows). Given that the patient has asthenia, the most likely diagnosis is thymoma.
Final diagnosis: benign thymoma
In the fourth chapter of The Wisdom of Dr. Pepe I intend to discuss checklists (chl), the fourth component of the equation:
D = (bc + lv + ps + chl) e
As I mentioned previously, about 60%-70% of diagnostic errors result from overlooking visible abnormalities in the chest radiograph. To avoid these errors, it is important to use checklists. Checklists accomplish a double task: discovering subtle abnormalities in apparently normal radiographs and adding information when an abnormality is obvious, thereby avoiding satisfaction of search.
I have a convenient method for using checklists, which implies looking at the PA radiograph from top to bottom and the lateral view from left to right. For practical purposes, the PA radiograph is divided into three areas (upper, middle, and lower) and the lateral view into three areas as well: anterior, middle, and posterior (Fig. 1).
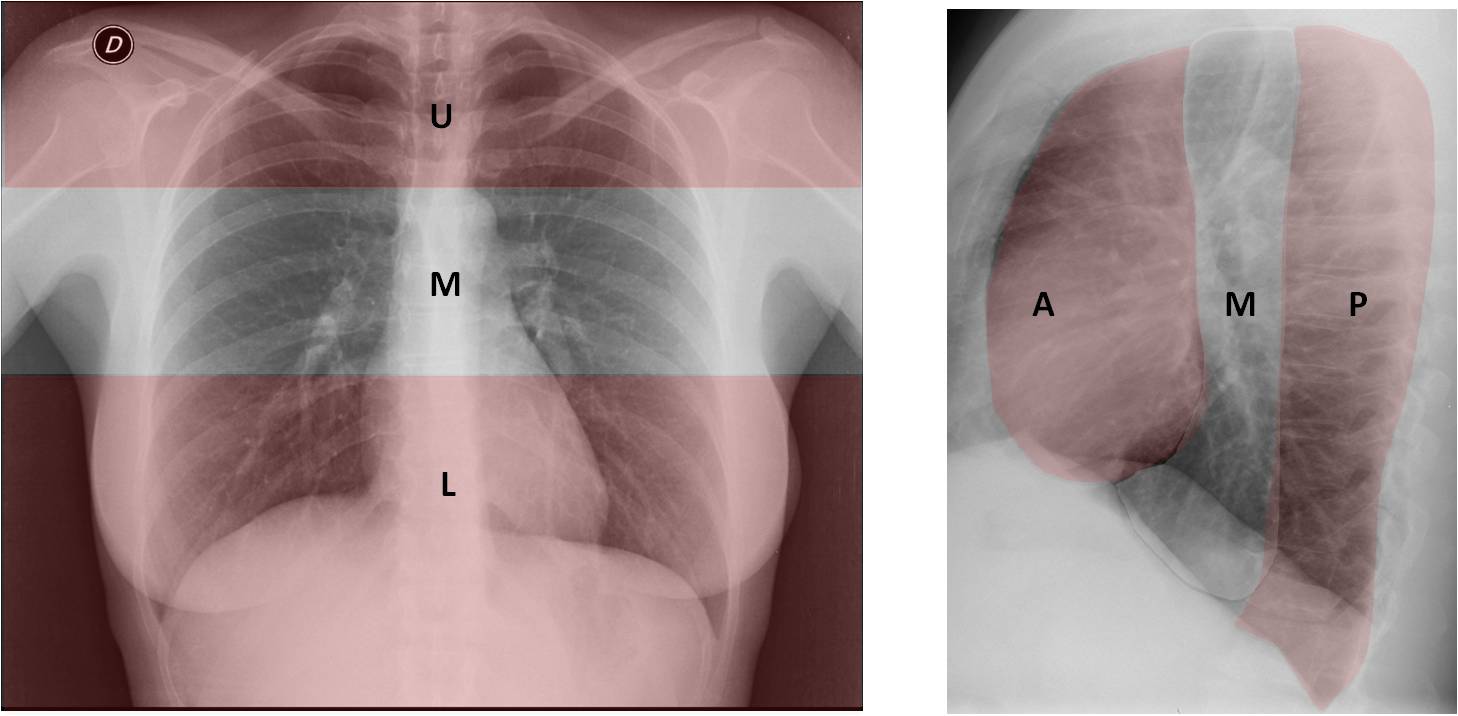
Fig. 1
Fig. 1. In the PA view, the upper area (U) is limited inferiorly by a line traced at the upper level of the aortic knob. The middle area (M) includes the hila in the center, and the lower area (L) reaches down to the end of the film.
In the lateral view, the anterior area (A) is limited by a line drawn along the anterior wall of the trachea and the posterior border of the heart. The posterior area (P) is the area behind a line traced along the anterior aspect of the vertebral bodies, and the middle area (M) is the area between these two lines.
For teaching purposes, I’ll present each area individually, depicting the anatomical regions to be examined and what to look for. After each area, I include a test case so you can practice looking for abnormalities.
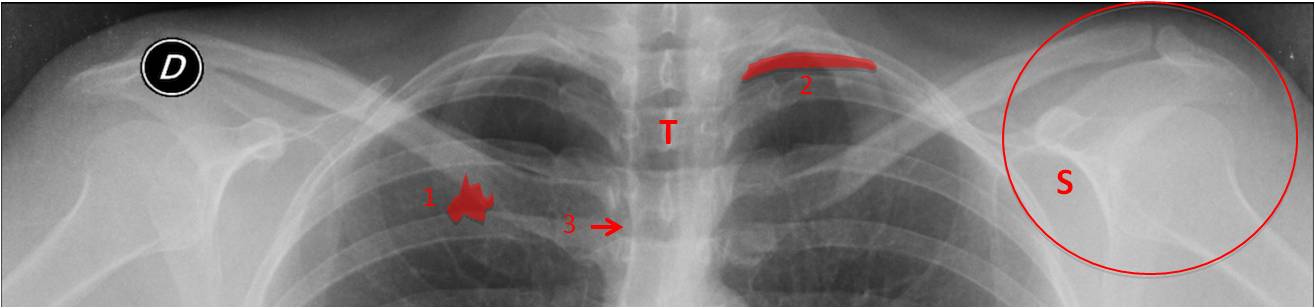
Fig. 2
Fig. 2. UPPER AREA. Regions that should be examined:
Pulmonary apices – Search for pulmonary nodules (1) and Pancoast tumor (2) (see Case #43).
Trachea (T) – Look for caliber changes and displacement by masses (Case #84).
Right paratracheal stripe (3) – Wider than 3 mm is abnormal (Case #72).
Shoulders (S) – Look for periarticular calcifications and osseous lesions (Case #89).
Also examine the ribs and chest wall included in the area.
TEST CASE (Fig. 3). 48-year-old woman with chest pain. What do you see?
(Answer below)
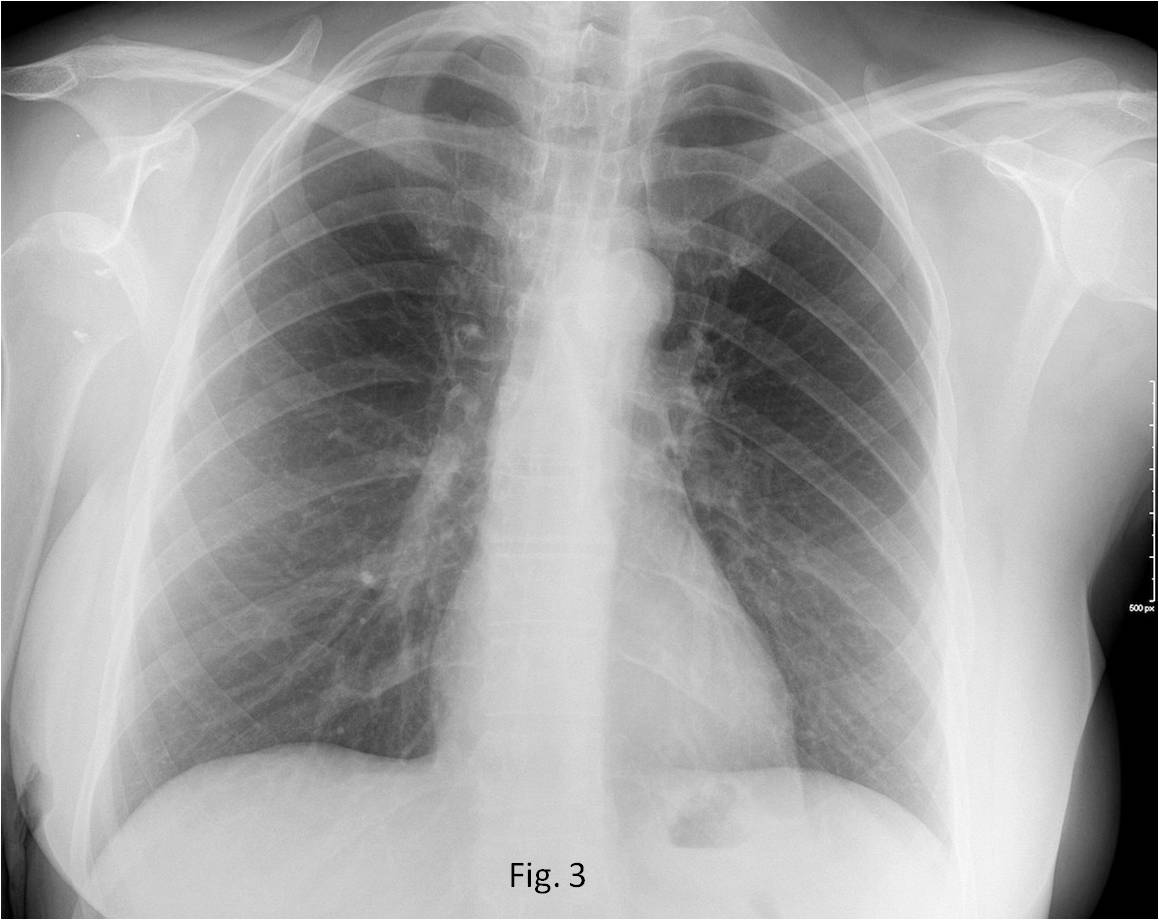
Fig. 3

Answer Fig. 3: PA radiograph was taken after chest trauma. There is an obvious anterior subluxation of the right humeral head (A, arrow). A previous radiograph shows the humeral head in the proper location (B). Metal implants from a previous surgery are visible.
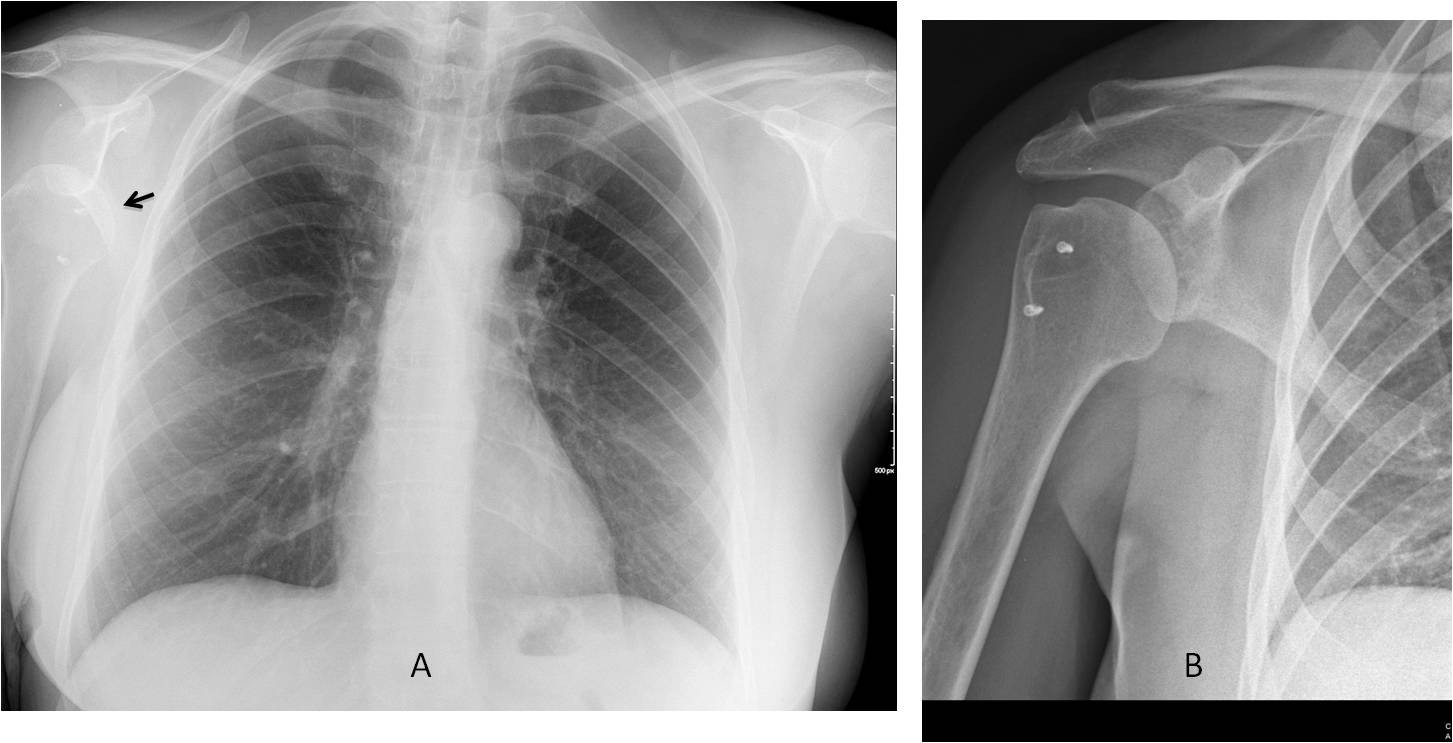
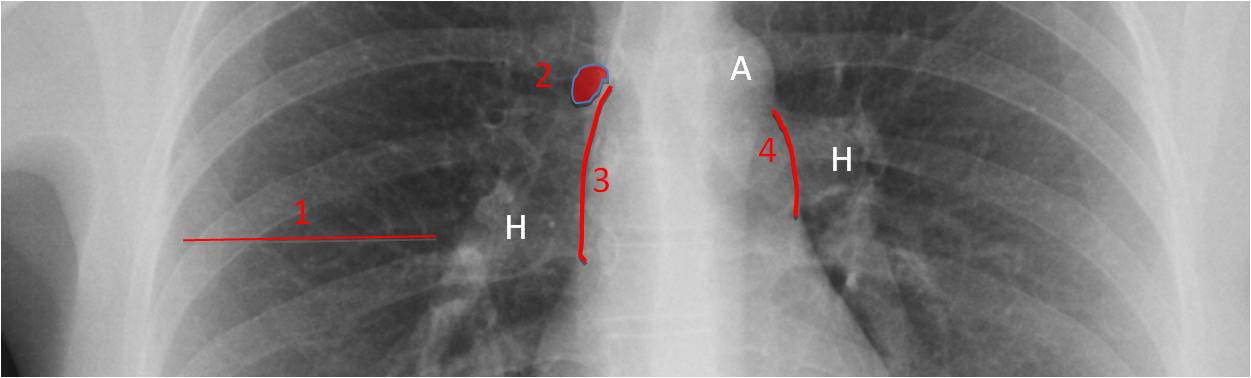
Fig. 4
Fig 4. MIDDLE AREA. Regions to examine:
The hila (H) – Size, density, and displacement (Case #49)
The middle fissure (1) – Displacement (Case #98)
The azygos arch (2) – Larger than 1 cm is abnormal (Case #101)
The ascending aorta (3) – (Case #59)
The aortic knob (A) – (Case #101)
The main pulmonary arch (4) – (Case #52)
Also, the ribs, chest wall, and lung parenchyma included in the area.
TEST CASE (Fig. 5). 59-year-old woman with dyspnoea. What do you see?
(Answer below)
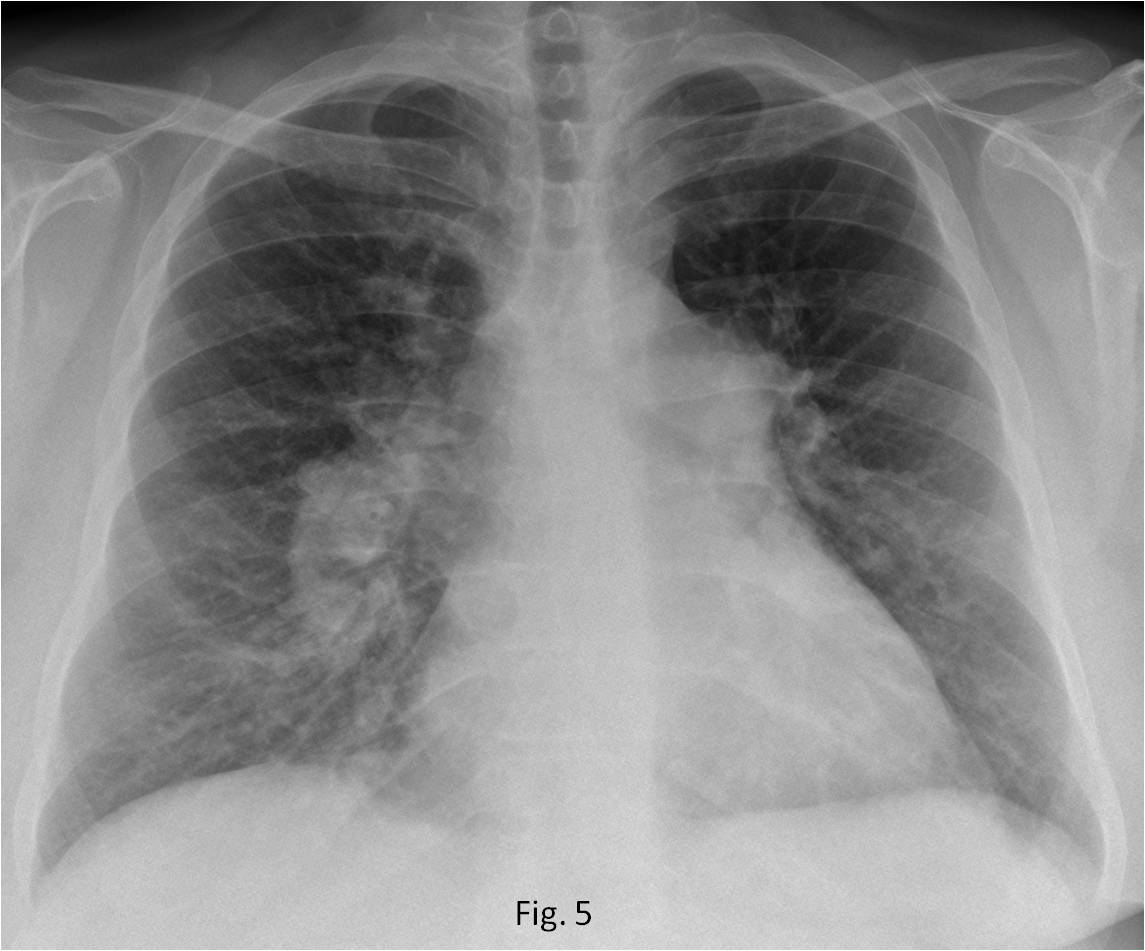
Fig. 5

Answer Fig. 5: PA radiograph shows increased size of both hila (A, white arrows) with diminished peripheral vasculature. The pulmonary arch is convex (A, red arrow). Axial CT confirms the pulmonary artery enlargement (B, red arrow). The main arteries have calcium in the wall (B, white arrows). The findings are practically pathognomonic of long-standing pulmonary arterial hypertension.
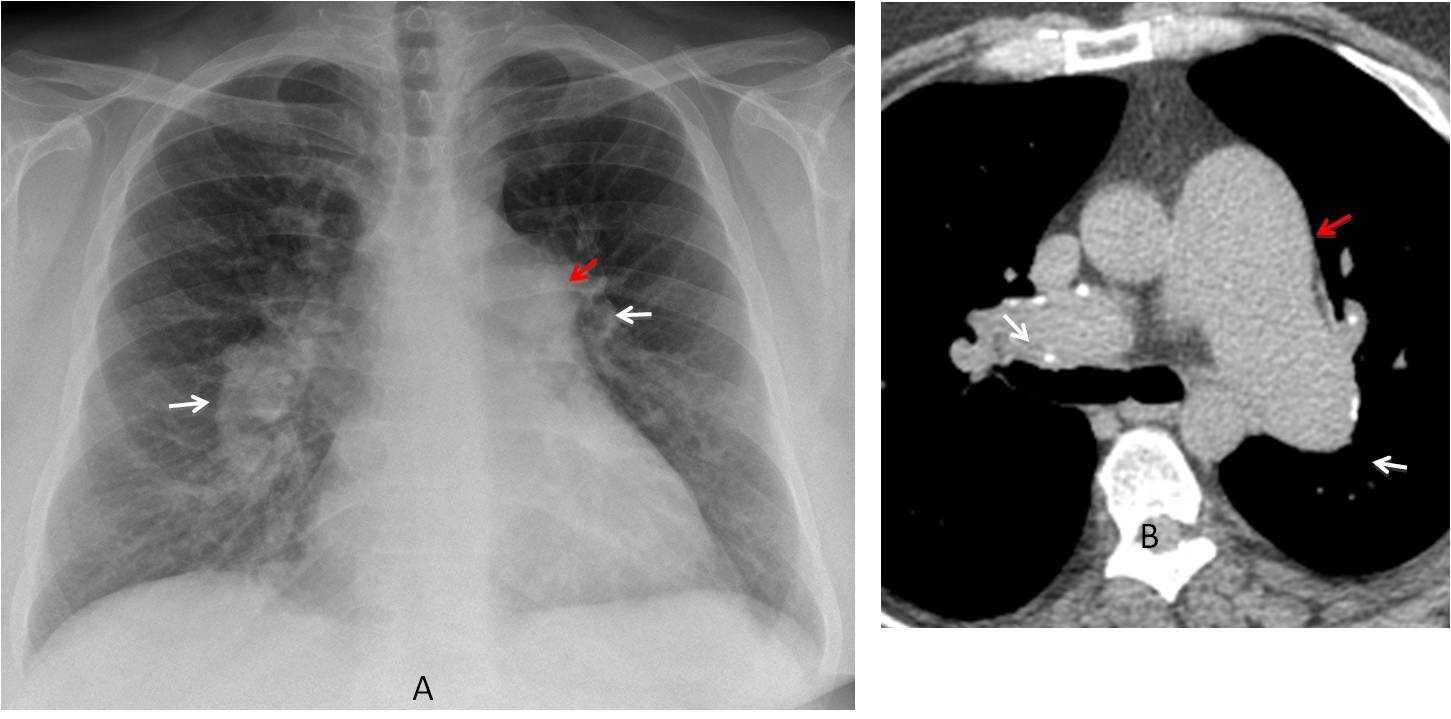
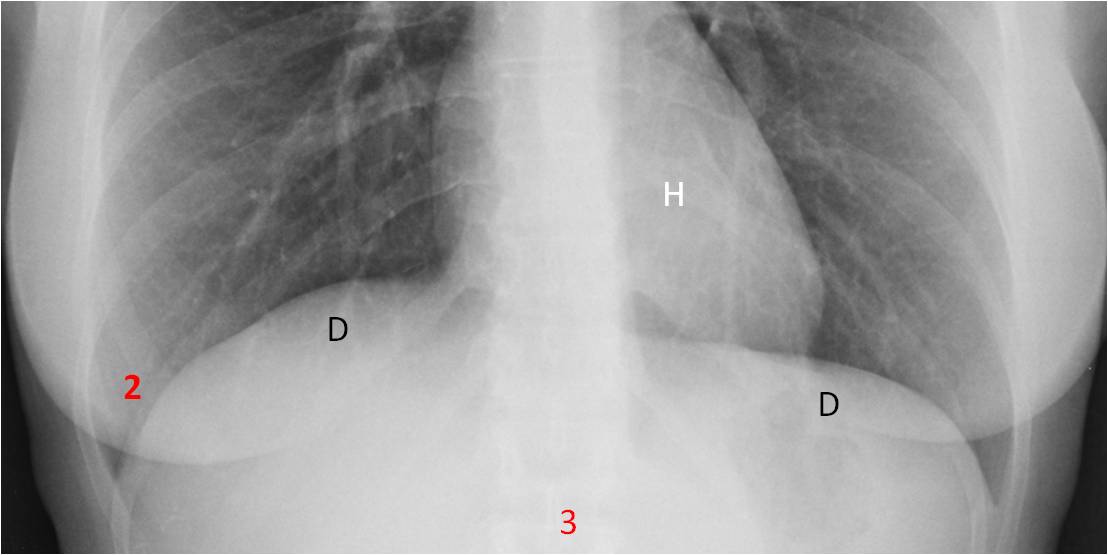
Fig. 6
Fig. 6. LOWER AREA. Regions that should be examined:
The heart (H) – Evaluate the size, contour, and calcifications (Cases #45-60).
Costophrenic sinuses (2) – Investigate blunting and hidden nodules (Case #91).
Diaphragm (D) – Elevation, hernias, and calcium (Case #48).
Upper abdomen (3) – Look for calcium and abnormal air (Case #80).
Also, the ribs, lung parenchyma, and chest wall included in the area.
TEST CASE (Fig. 7). Preoperative chest radiograph in a 62-year-old woman. What do you see?
(Answer below)

Fig. 7

Answer Fig. 7: PA radiograph shows a faint curvilinear calcification in the left upper abdomen (A, arrow). Enhanced axial CT confirms the presence of a calcified splenic cyst (B, arrow).
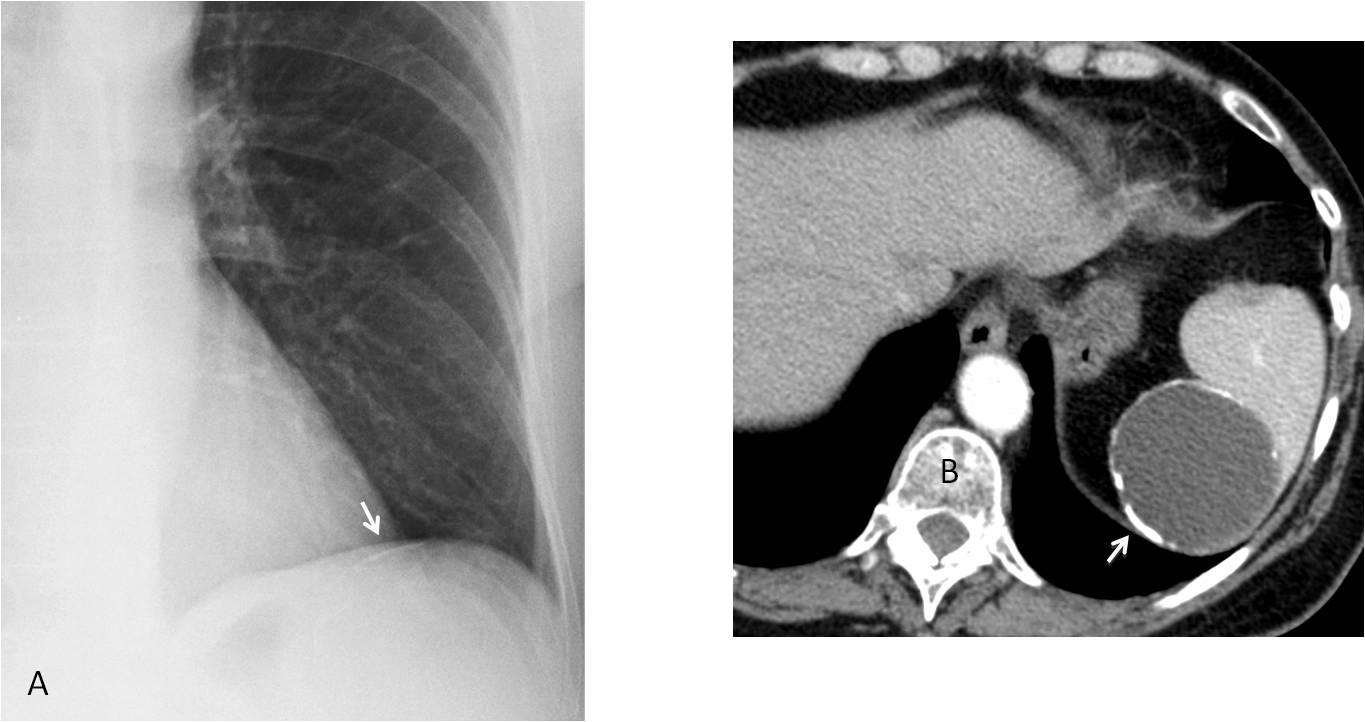
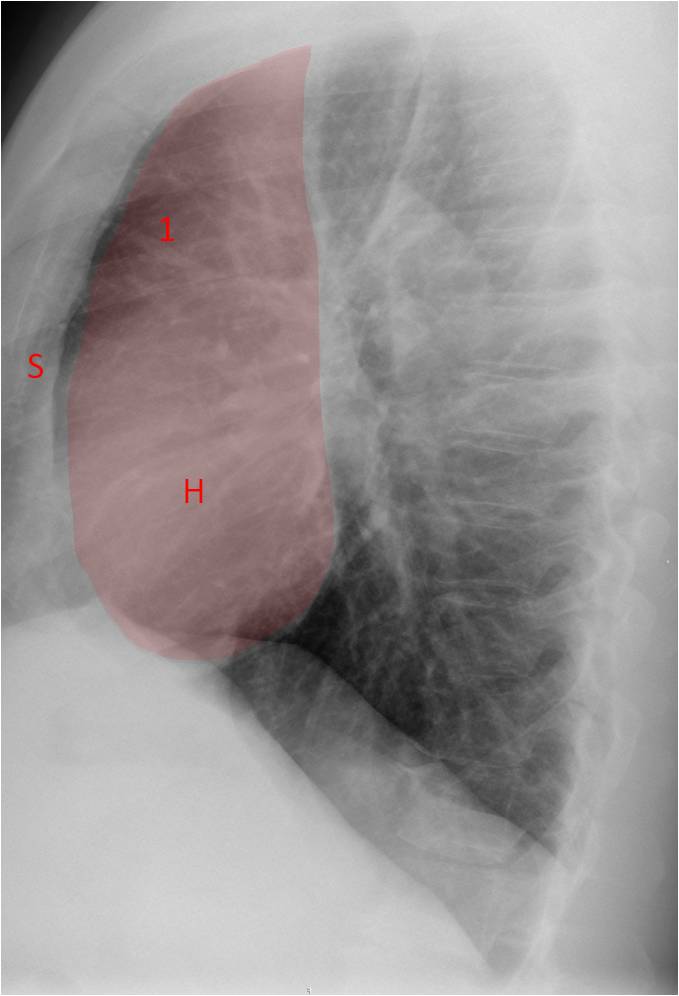
Fig. 8
Fig. 8. ANTERIOR AREA. Regions to examine:
Sternum (S) – Osseous lesions, pectus excavatum (Case #77)
Anterior clear space (1) – Look for opacities (Case #68)
Heart (H) – Size, contour and calcifications (Case #60)
TEST CASE (Fig. 9). 28-year-old man, asymptomatic. What do you see?
(Answer below)
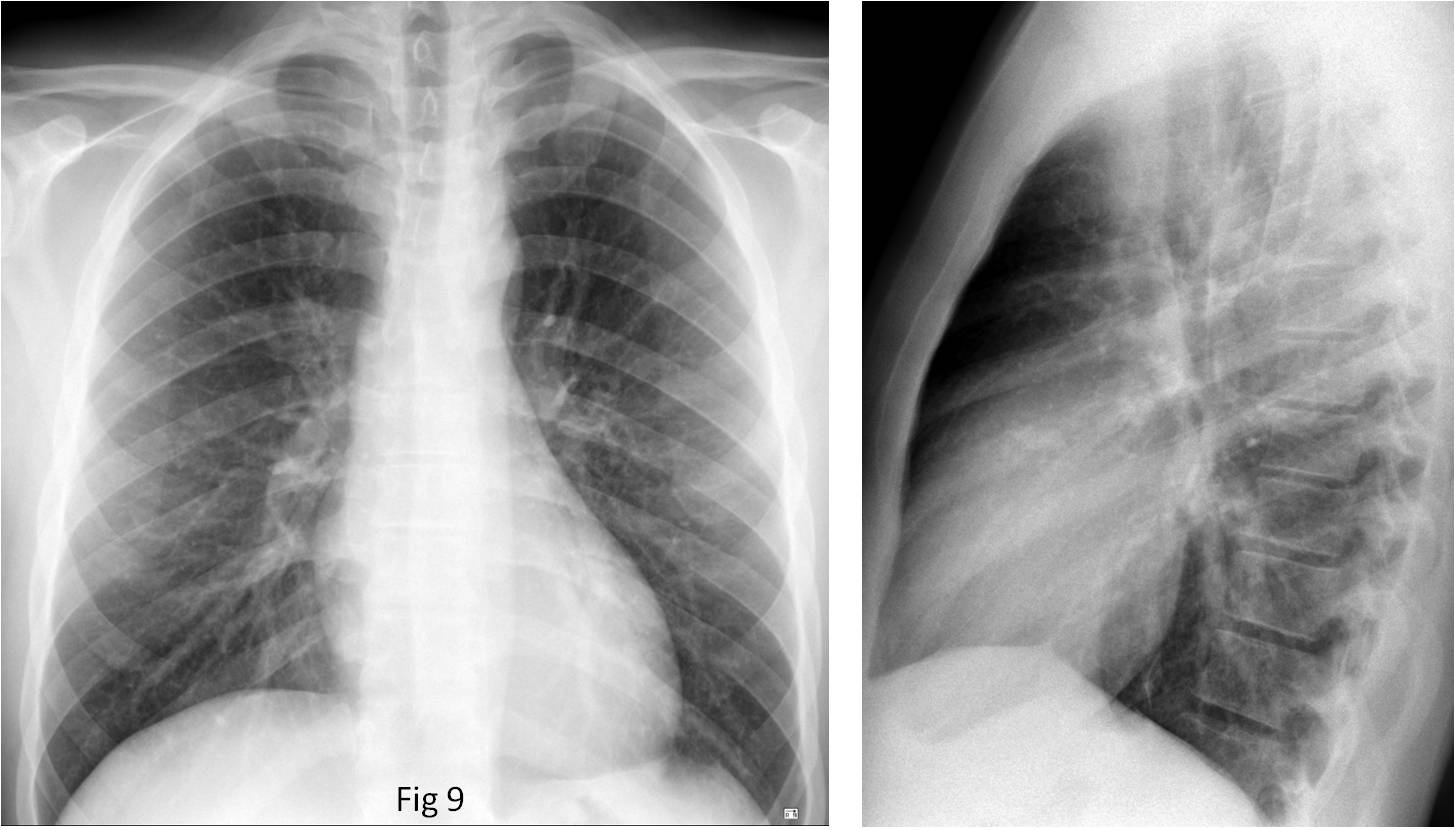
Fig. 9

Answer Fig. 9: Lateral radiograph shows a coarse linear calcification in the area of the aortic valve (A, circle). Unenhanced sagittal CT confirms the calcified aortic valve (B, arrow). Congenital aortic stenosis, surgically proven.
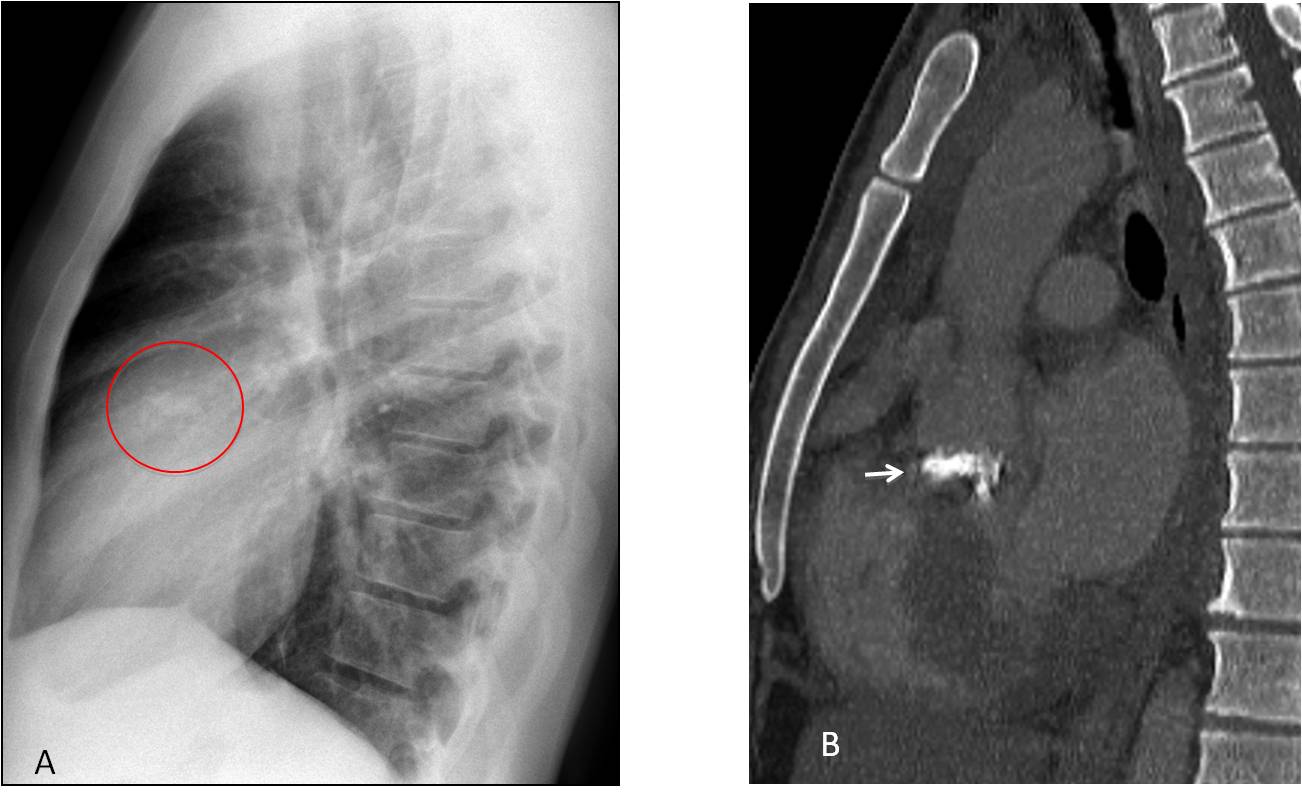
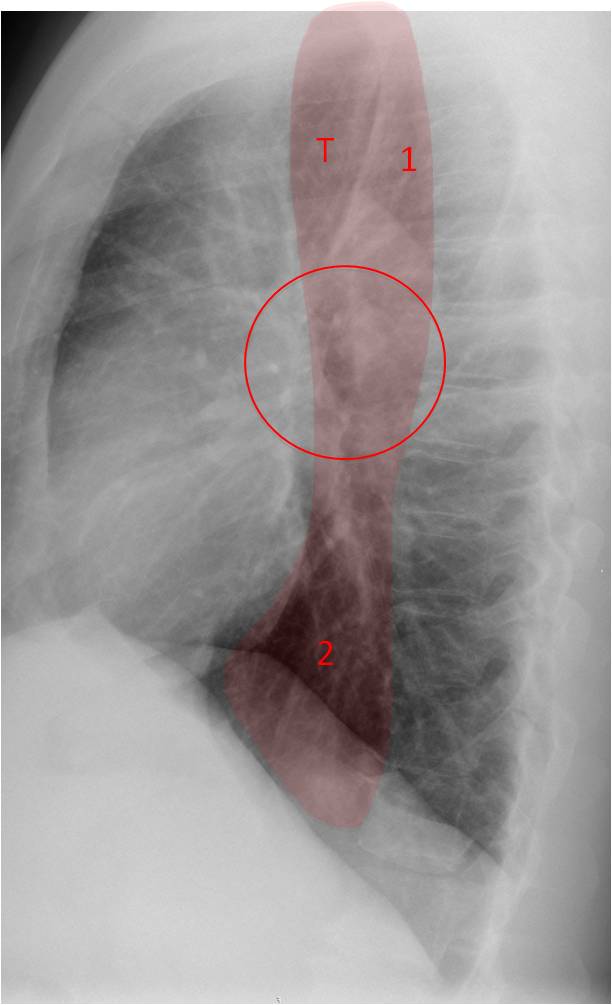
Fig. 10
Fig. 10: MIDDLE AREA. Regions to examine:
Trachea (T) – Caliber changes, displacement (Case #101)
Raider triangle (1) – Opacification (Case #101)
Hila (circle) – Size, donut sign (Case #101)
Retrocardiac space (2) – Opacifications (Case #100)
TEST CASE (Fig. 11). 32-year-old man with fever and malaise. What do you see?
(Answer below)
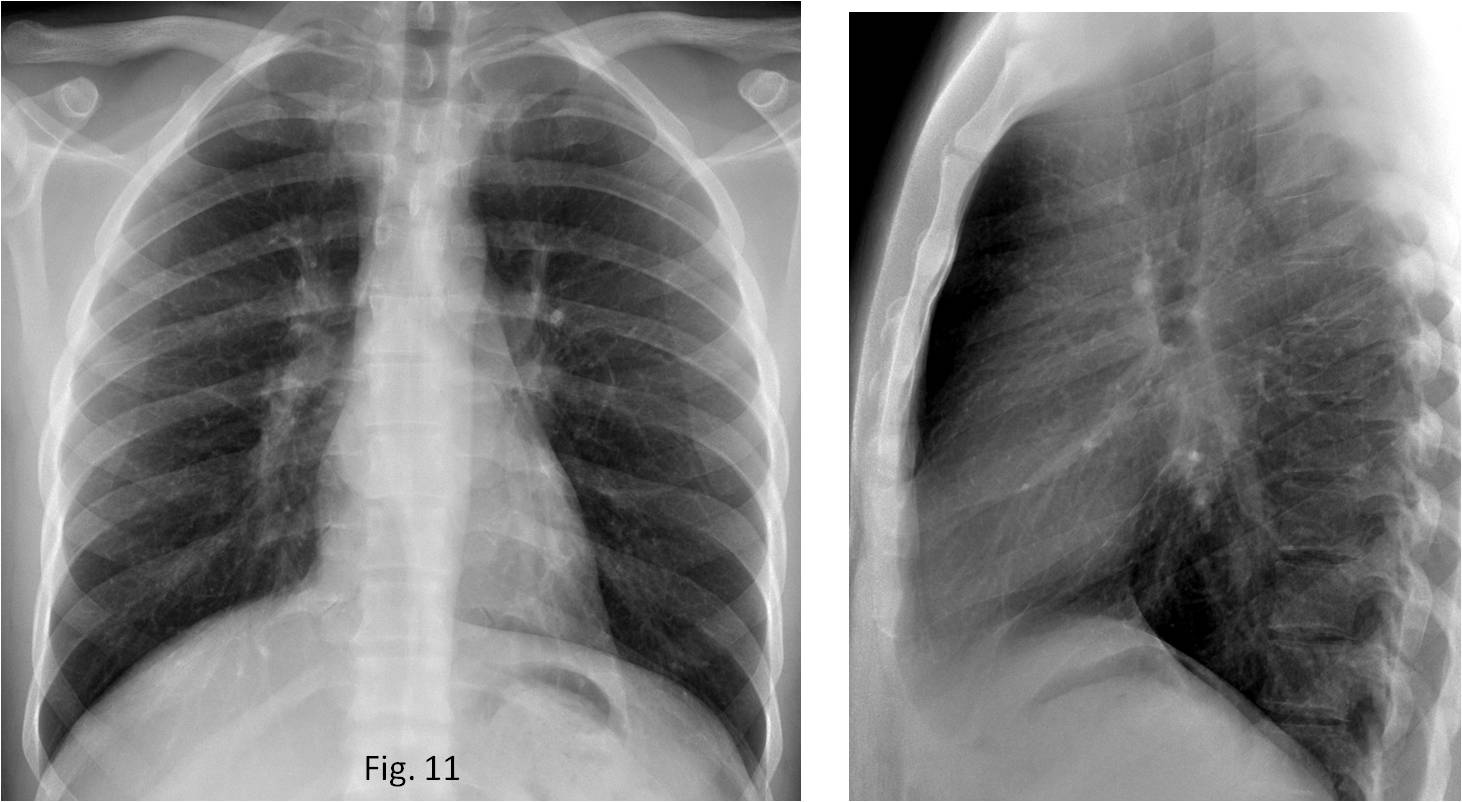
Fig. 11

Answer Fig. 11: PA and lateral radiographs show a subcarinal mass (A and B, arrows). Enhanced coronal CT shows a large subcarinal mass with areas of necrosis (C, arrows). Diagnosis: active TB with necrotic lymph nodes.
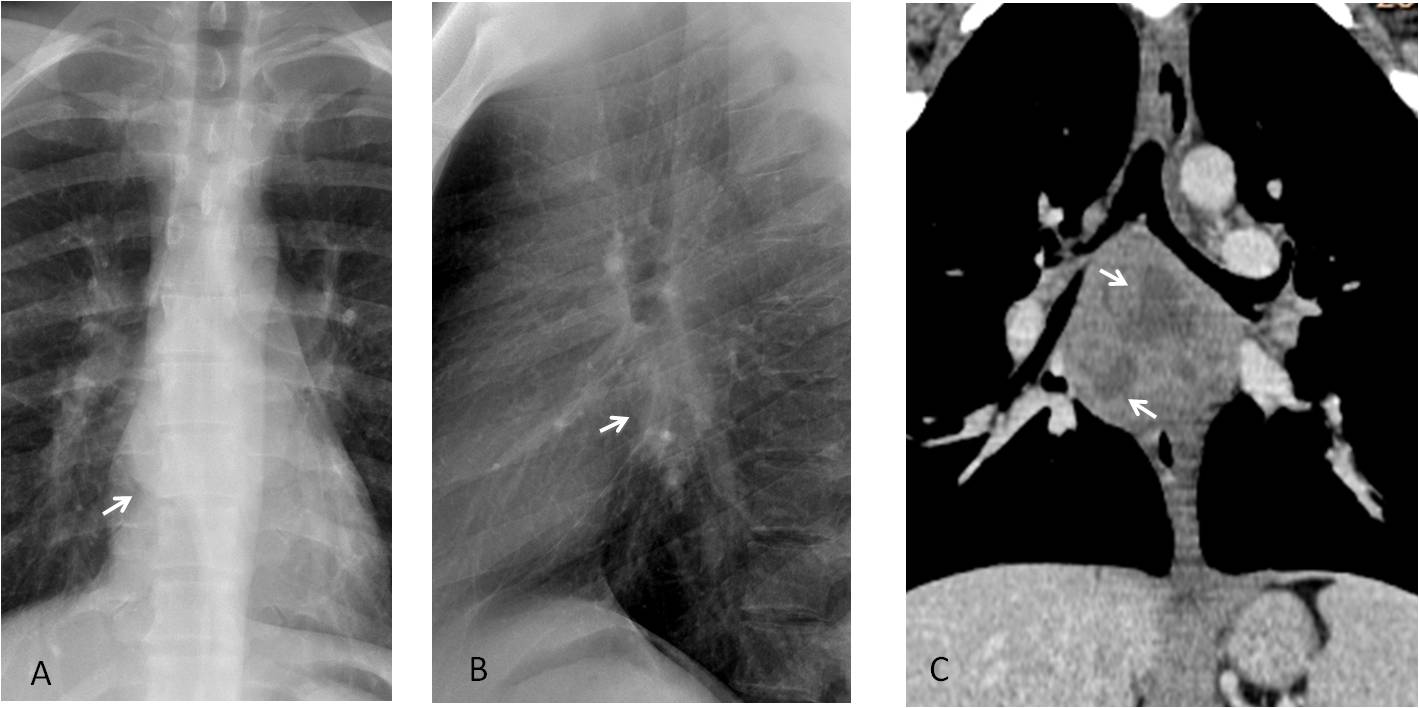
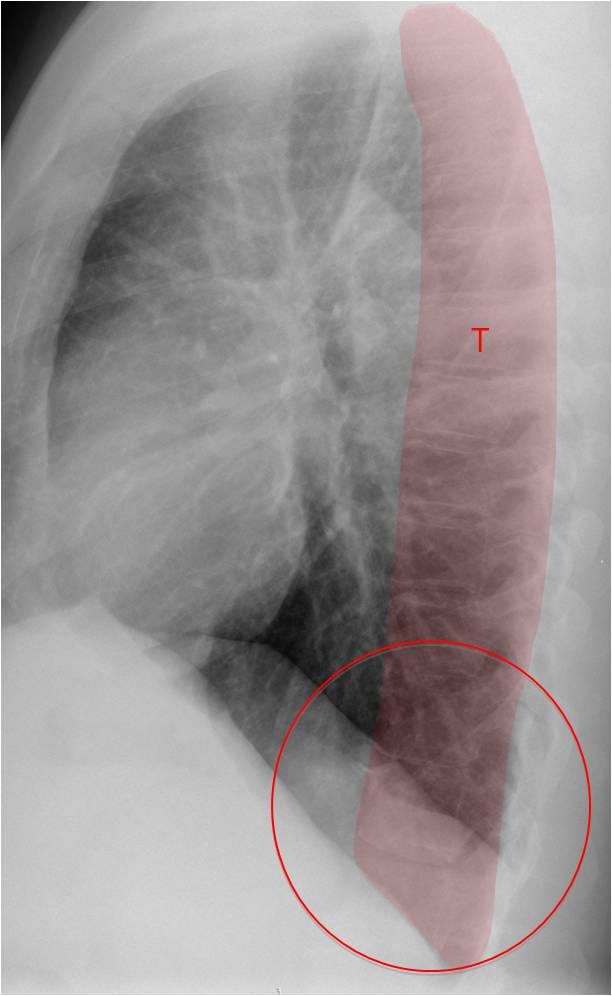
Fig. 12
Fig. 12. POSTERIOR AREA. Regions to examine:
Thoracic spine (T). Vertebral and disk lesions, superimposed lesions (Case #83)
Posterior clear space (circle). Opacifications (Case #71)
TEST CASE (Fig. 13). 62-year-old man, asymptomatic. What do you see?
(Answer below)
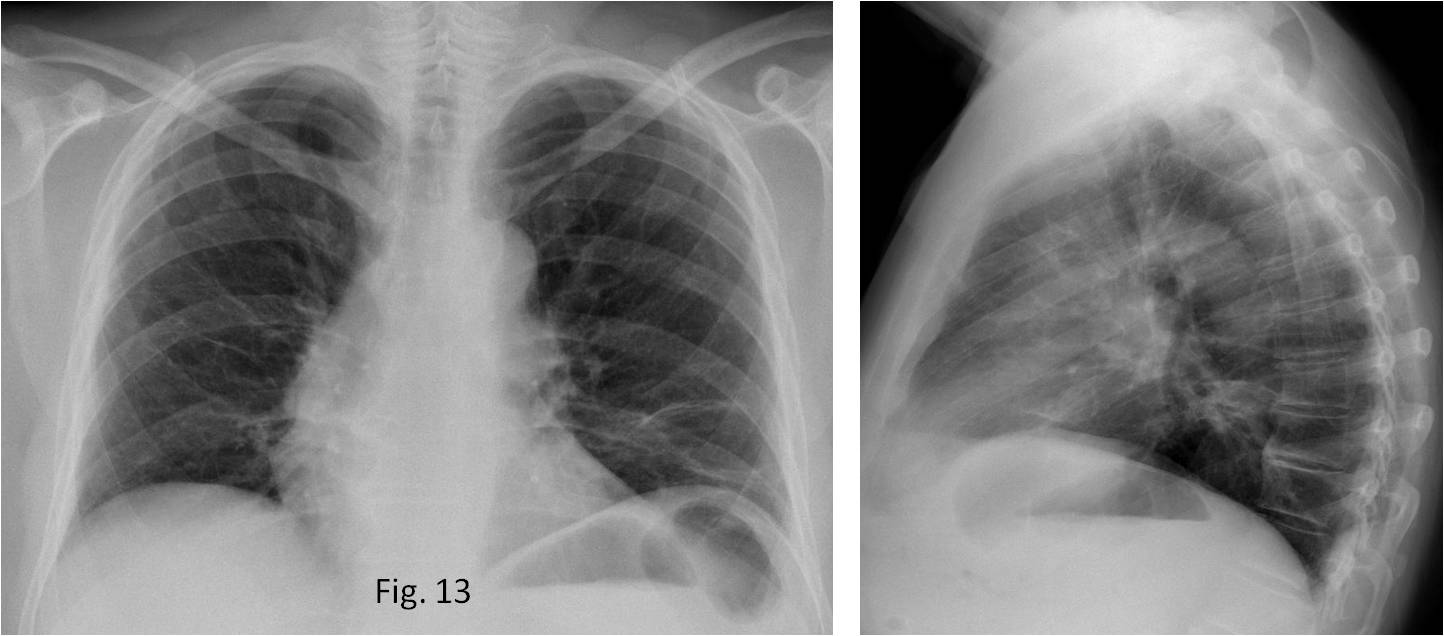
Fig. 13
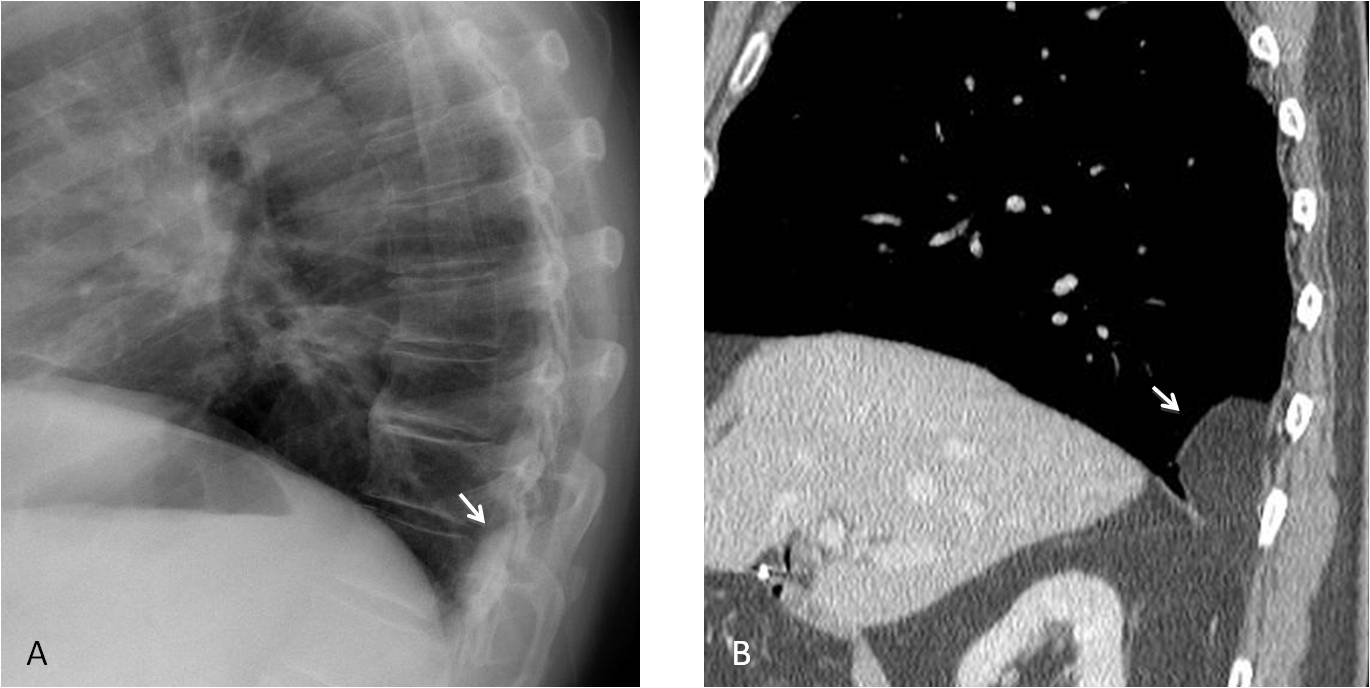
Answer Fig. 13. Lateral radiograph shows a well-defined posterior opacity that seems extrapulmonary (A, arrow). Sagittal CT demonstrates a fatty Bochdalek hernia (B, arrow).
TEST CASE (Fig. 14). 55-year-old male with hypernephroma. What do you see?
(Answer below)
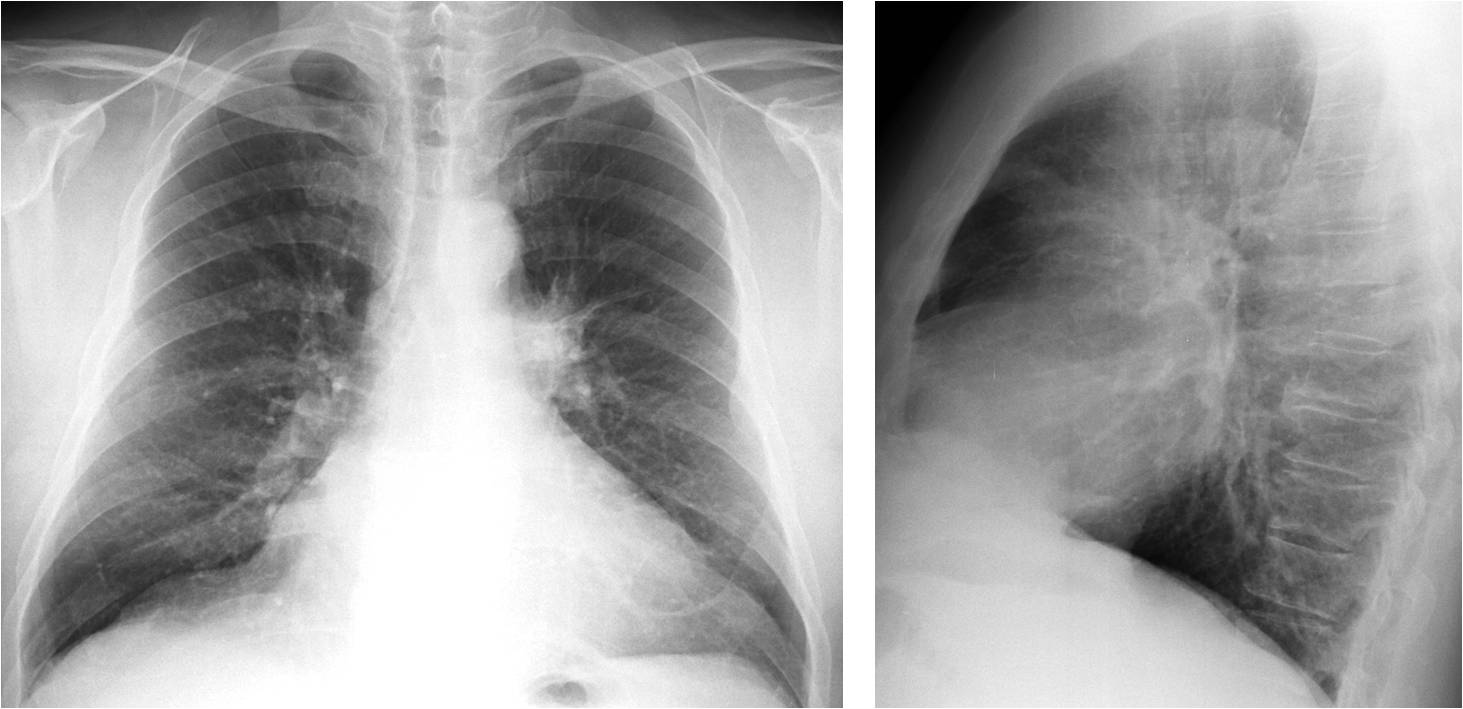
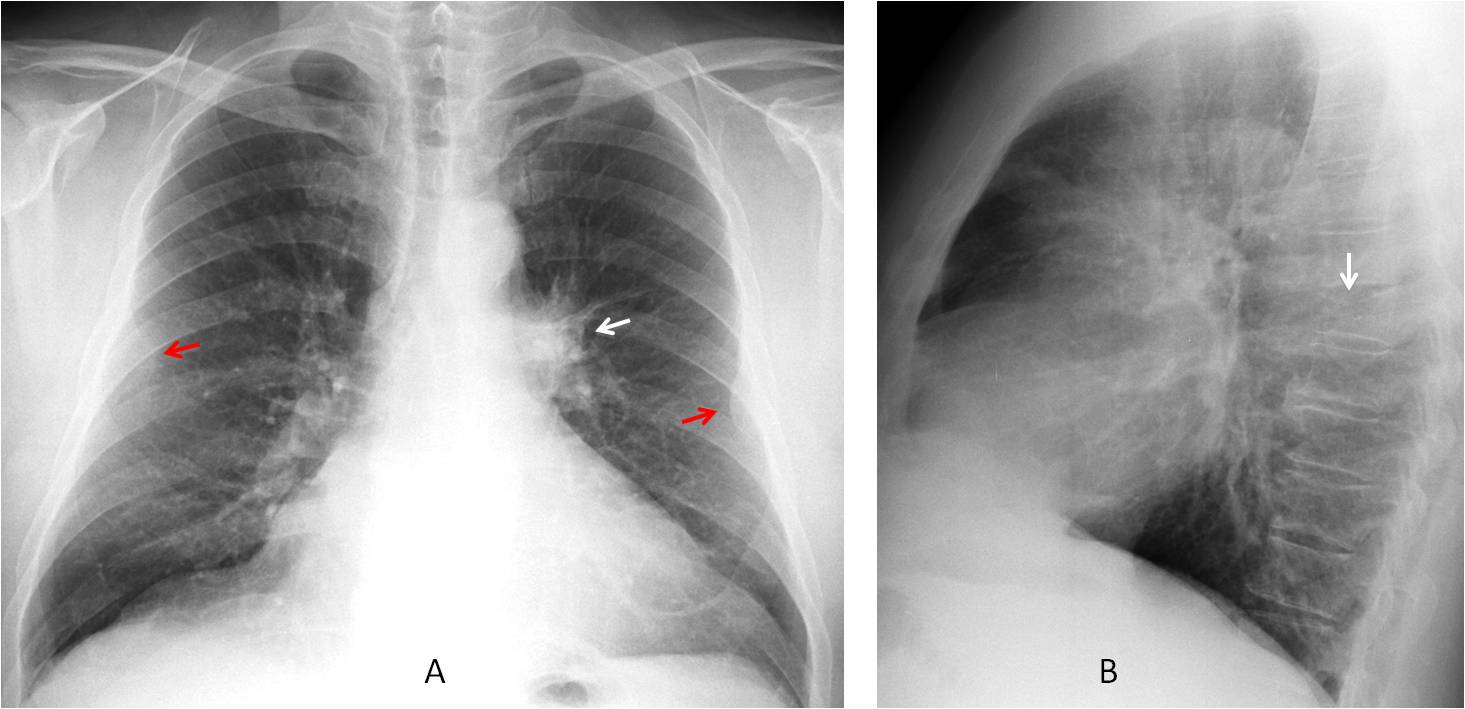
Fig. 14

Answer Fig. 14. PA radiograph shows a dense left hilum (A, white arrow). If we look carefully and use checklists, two extrapulmonary lesions are seen (A, red arrows). The lateral view shows flattening of a thoracic vertebra with destruction of the upper cortex (B, arrow). In a patient with hypernephroma these findings suggest widespread metastasis and emphasize the value of checklists to avoid satisfaction of search.
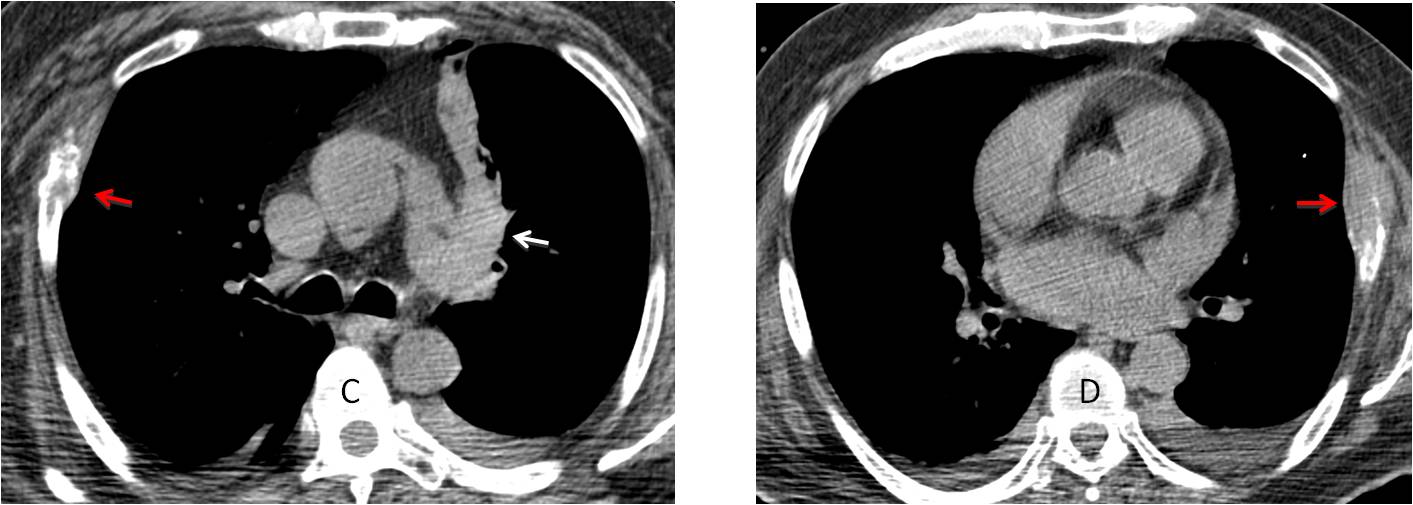
Unenhanced axial CT confirms a left hilar lesion causing segmental atelectasis (C, white arrow) and two lytic rib metastases (C and D, red arrows).

Dr. Pepe’s fourth commandment:
Thou shalt always use checklists:
- To discover lesions in an apparently normal chest
- To avoid satisfaction of search


Good morning!!
Ufff, I think the right paraspinal interface is displaced, perhaps because of osteophytes or neurogenic/spinal disease.
I need the lateral view!!!!
You will have one on Friday
Left paraspinal shadow approximately at the level of aortic knob, giving double contour. Presence of hilum overlay sign indicates lesion on the anterior or posterior mediastinum. Next step – lateral view.
I think there is bilatral paraspinal shadaow in superior mediastiunm with smal Rt displacement of trachea … latral C x ray and CT Scane help. Mybe thymoma
…Prof. io guarderei meglio anche l’ilo di sx….
There is widening of the left paratrachial stripe (exacerbated by rotation) but still there. Slight prominence of the left hilum.
There is also an ill defined opacity overlaying the 9th right posterior rib which does not have the usual apearance of a nipple shadow possible nodule.
I would recommend CT next
double aortic arch shadow ?
Undulating border aortic arch. ?diverticulum
Left hilum enlargement
bulge of the right paraspinal line ?
There is an obvious double contour of the aortic knob. The answer needs a lateral view and,eventually, a CT, which will be shown tomorrow.
Congratulations to Stevan Vasiljevic who was the first to detect the abnormality
Thank you for that excellent presentation. I am not a junior radiologist and have an interest in chest and always learn something.
lateral view needed .